Stopping Adderall after long‑term use can feel like hitting a wall. Within days, many people experience crushing fatigue, mental fog, and a collapse in focus that disrupts work, school, and daily life.
According to the ASAM/AAAP guideline on stimulant use disorder, acute withdrawal symptoms typically begin within 24 hours and can extend into post‑acute phases lasting weeks to months, depending on dose, duration, and individual factors.
This article explains the Adderall withdrawal timeline, what symptoms to expect, and how to navigate detox safely with medical support.
What is Adderall Withdrawal?
Adderall withdrawal refers to the cluster of physical, cognitive, and emotional symptoms that emerge when someone who has been taking mixed amphetamine salts regularly stops or sharply reduces their dose.
The drug works by increasing dopamine and norepinephrine in the brain, which enhances attention, alertness, and motivation. When you stop, your brain must readjust to functioning without that chemical boost.
Withdrawal is not the same as addiction, but it is a real physiological response. Even people who take Adderall exactly as prescribed for ADHD can experience withdrawal symptoms when they discontinue. The ASAM/AAAP guideline recognizes stimulant withdrawal as a phase‑based process that includes acute, post‑acute, and recovery periods, each with distinct symptoms and care needs.
Adderall Withdrawal Timeline: What to Expect?
Understanding the typical withdrawal timeline can help you prepare and recognize when symptoms are likely to peak or improve. While individual experiences vary, research and clinical guidelines outline a predictable pattern.
Days 1–2: The Crash
The first 24 to 48 hours after your last dose often bring a sudden “crash.” Catecholamine depletion and sleep deprivation drive this early phase. You may feel:
- Extreme tiredness or hypersomnia
- Irritability and mood swings
- Increased appetite
- Strong cravings for the medication
This crash reflects your body’s rebound from prolonged stimulation. Many people sleep heavily during this window as their brain catches up on rest.
Days 3–5: Peak Symptoms
Between days three and five, withdrawal symptoms often intensify. Clinical timelines describe this as the peak period, when dysphoria, anxiety, and sleep disturbances are most pronounced. Common experiences include:
- Depressed mood or emotional flatness
- Anxiety or restlessness
- Insomnia or disrupted sleep patterns
- Headaches and body aches
- Difficulty concentrating
This is a critical window for safety monitoring. The ASAM/AAAP guideline recommends routine suicidality screening during stimulant withdrawal, as mood symptoms can spike during this phase.
Days 6–10: The Withdrawal Wall
Around days six through ten, many people encounter what clinicians call the “withdrawal wall.” This phase is marked by persistent fatigue, low motivation, mental fog, and attention failures. For professionals and students, this period can be especially disabling because cognitive tasks feel nearly impossible.
The wall represents a transition from acute to post‑acute withdrawal. Pediatric randomized‑withdrawal studies show that health‑related quality of life and functioning can deteriorate within six weeks of stopping stimulants, underscoring that clinically meaningful effects extend well beyond two weeks for many individuals.
Week 2 and Beyond: Post‑Acute Withdrawal
After the first week, physical symptoms like headaches and sleep disruption typically ease. However, mood and cognitive symptoms may linger. The ASAM/AAAP guideline explicitly recognizes that post‑acute stimulant withdrawal can last weeks to months, with symptoms including:
- Residual depression or anxiety
- Attention and concentration problems
- Episodic cravings
- Slow return to baseline energy and motivation
Some sources describe this as post‑acute withdrawal syndrome (PAWS), though authoritative reviews caution that PAWS is not a formal DSM diagnosis and rigorous evidence outside alcohol withdrawal remains limited. Nonetheless, chronic stimulant exposure induces neuroadaptations that can fuel lingering symptoms.
Common Symptoms of Adderall Withdrawal
Adderall withdrawal symptoms fall into three broad categories: physical, cognitive, and emotional.
Physical symptoms:
- Fatigue and low energy
- Hypersomnia or insomnia
- Increased appetite and weight gain
- Headaches and muscle aches
- Slowed movements
Cognitive symptoms:
- Difficulty focusing or sustaining attention
- Mental fog or sluggish thinking
- Impaired memory and decision‑making
- Disorganization and task initiation problems
Emotional symptoms:
- Depressed mood or anhedonia
- Anxiety and irritability
- Mood swings
- Cravings for the medication
- In severe cases, suicidal thoughts
It is important to distinguish withdrawal symptoms from the return of underlying ADHD symptoms. When Adderall is stopped, core ADHD features like inattention and impulsivity often re‑emerge, compounding the withdrawal experience.
Real‑world adult data confirm that stopping ADHD medications increases the risk of symptom exacerbation and may reduce quality of life.
How Long Does Adderall Detox Take?
The duration of Adderall detox depends on several factors, including how long you have been taking the medication, your daily dose, whether you stop abruptly or taper, and your individual physiology.
For most people, acute physiologic withdrawal symptoms improve within one to two weeks. However, functional recovery and stabilization commonly require six to twelve weeks or longer, especially without an optimized alternative treatment plan.
Pediatric randomized‑withdrawal evidence demonstrates measurable deterioration in functioning within six weeks of discontinuation, and adult clinical experience during recent stimulant shortages shows that multi‑week gaps often lead to significant work and school impairment.
A realistic detox is not a fixed calendar date. It is a staged clinical process that may include tapering, cross‑titration to alternative medications, behavioral supports, and close monitoring.

Adderall Detox Symptoms: What Makes Them Worse?
Certain factors can intensify withdrawal symptoms and prolong recovery:
- Abrupt cessation: Stopping suddenly, especially after high doses or long‑term use, tends to produce more severe symptoms than a gradual taper.
- High doses and long duration: The higher your dose and the longer you have been taking Adderall, the more pronounced your withdrawal may be.
- Co‑occurring mental health conditions: Anxiety, depression, or trauma can amplify mood symptoms during withdrawal.
- Sleep debt: Chronic sleep deprivation accumulated during stimulant use can worsen fatigue and cognitive fog.
- Lack of support: Isolation, high‑stress environments, and absence of medical or social support increase the risk of relapse and functional collapse.
Conversely, a structured taper, medical supervision, sleep hygiene, nutrition, and behavioral strategies can all reduce symptom severity and shorten recovery time.
Does Adderall Have Withdrawal Symptoms Even at Prescribed Doses?
Yes. Withdrawal symptoms can occur even when Adderall is taken exactly as prescribed for ADHD. The ASAM/AAAP guideline and clinical experience confirm that therapeutic use does not prevent physiologic dependence or withdrawal.
The key distinction is between physical dependence and addiction. Physical dependence means your body has adapted to the medication and will react when it is removed. Addiction involves compulsive use despite harm, loss of control, and continued use in risky situations. Many people who experience withdrawal from prescribed Adderall do not have a stimulant use disorder.
That said, individuals with co‑occurring stimulant use disorder require enhanced monitoring and risk‑adjusted care during discontinuation, including preference for extended‑release formulations and more frequent follow‑up.
How to Detox From Adderall Safely?
Safe Adderall detox begins with medical assessment and a tailored plan. Here are the core steps:
1. Consult a Healthcare Provider
Do not stop Adderall abruptly without medical guidance, especially if you have been taking it for months or years. A provider can assess your dose, duration, comorbidities, and functional demands to design a safe discontinuation strategy.
2. Consider a Gradual Taper
Tapering means slowly reducing your dose over days to weeks. While adult stimulant trials do not specify taper schedules, clinical rationale supports dose reduction to minimize withdrawal severity and allow monitoring of symptom relapse in a controlled way.
3. Explore Alternative Medications
If you are stopping Adderall due to side effects, shortages, or concerns about misuse risk, alternatives may help maintain ADHD symptom control:
- Lisdexamfetamine (Vyvanse): Another long‑acting stimulant with strong efficacy and a smoother pharmacokinetic profile.
- Methylphenidate: A different stimulant class that may be better tolerated.
- Non‑stimulants: Atomoxetine, guanfacine, clonidine, and viloxazine are recommended when stimulant risks outweigh benefits or when stimulants are unavailable.
Cross‑titration to an alternative can prevent functional collapse during the transition.
4. Prioritize Sleep, Nutrition, and Routine
- Sleep hygiene: Consistent sleep and wake times, a dark and quiet bedroom, and limited screen time before bed can help reset your sleep‑wake cycle.
- Nutrition: Regular, balanced meals with adequate protein support neurotransmitter synthesis and stabilize energy.
- Structured routines: Daily schedules and to‑do lists scaffold task initiation and reduce cognitive load during periods of low motivation.
5. Use Behavioral and Therapeutic Supports
Cognitive‑behavioral therapy, mindfulness, and ADHD coaching can help you manage symptoms and develop coping strategies. Family involvement and peer support also improve outcomes.
6. Monitor for Safety Risks
The ASAM/AAAP guideline recommends routine suicidality screening during stimulant withdrawal using validated tools like the Columbia Suicide Severity Rating Scale. If you experience suicidal thoughts, contact a healthcare provider or emergency services immediately.
7. Plan for Shortages and Access Challenges
The ongoing stimulant shortage has forced many patients into unplanned discontinuation. Proactive steps include:
- Notifying your prescriber early if refills are delayed
- Identifying multiple pharmacies that stock your medication
- Discussing backup plans and alternative agents before a gap occurs
- Avoiding unregulated sources, which carry counterfeit and overdose risks
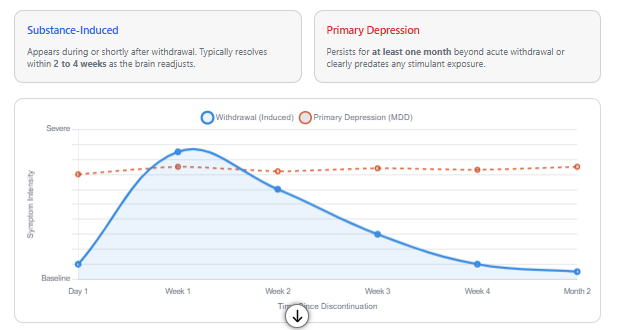
Withdrawal From Adderall vs. Primary Depression: How to Tell the Difference?
One of the most common clinical errors is diagnosing major depressive disorder during the withdrawal window. DSM‑based guidance provides clear temporal anchors:
- Substance‑induced depression typically appears during or shortly after withdrawal and resolves within days to several weeks once the substance is cleared.
- Primary major depressive disorder persists for at least one month beyond acute withdrawal or clearly predates stimulant exposure.
If depressive symptoms track the withdrawal timeline and improve within two to four weeks, they are likely stimulant‑induced. Premature MDD diagnosis can lead to unnecessary long‑term antidepressants and delay appropriate withdrawal management.
Clinicians should also consider ADHD symptom rebound, which can mimic depression. Inattention, low task persistence, and disorganization often return quickly after stopping stimulants and may be misread as anhedonia or low motivation.
When to Seek Professional Help?
You should seek professional support if you experience:
- Severe or worsening depression or anxiety
- Suicidal thoughts or self‑harm urges
- Inability to function at work, school, or home
- Relapse to stimulant misuse or other substance use
- Physical symptoms like chest pain, seizures, or high fever
Medically supervised detox programs offer 24‑hour monitoring, symptom management, and a safe environment during the most challenging phases of withdrawal. Partial hospitalization and intensive outpatient programs provide structured support while allowing you to maintain some daily responsibilities.
The Role of Comprehensive Treatment Programs
Adderall withdrawal is not just a physical process. It often involves emotional, cognitive, and functional challenges that benefit from integrated care. Evidence‑based treatment programs combine medical management, individual and group therapy, family support, and holistic approaches like yoga, nutrition counseling, and mindfulness.
For individuals with co‑occurring mental health conditions or stimulant use disorder, dual‑diagnosis treatment addresses both issues simultaneously, reducing the risk of relapse and improving long‑term outcomes.
If you or someone you care about is struggling with Adderall withdrawal or stimulant dependence, reaching out for help is a sign of strength, not weakness. Professional guidance can make the difference between a safe, supported recovery and a prolonged, isolating struggle.
Ready to take the next step? Contact The Summit Wellness Group to speak with a compassionate care team about individualized detox and recovery options customized to your needs.
