GHB withdrawal is a fast-moving, potentially life-threatening syndrome that can begin within hours of the last dose. In one recent detox cohort, about 31% of patients developed delirium and roughly 20% needed ICU-level care, making this one of the most dangerous withdrawal syndromes seen in general hospitals.
This article breaks down the symptoms, timeline, risk factors, and treatment options so you or someone you care about can make informed decisions.
What is GHB Withdrawal?
GHB (gamma-hydroxybutyrate) is a potent central nervous system depressant with a very short half-life of roughly 20 to 60 minutes. Its precursors, GBL and 1,4-butanediol, convert to GHB in the body and carry the same risks. Because the drug clears so quickly, dependent users often dose every one to three hours around the clock. When that supply stops, the brain rebounds hard.
GHB withdrawal shares features with alcohol and benzodiazepine withdrawal because all three involve sedative receptor systems. But GHB acts mainly through GABA-B receptors rather than GABA-A, which helps explain why standard benzodiazepines often fall short during treatment. The result is a syndrome that can escalate faster and resist first-line medications more often than alcohol withdrawal does.
Delirium tremens occurs in about 5% of alcohol withdrawal cases. GHB withdrawal delirium, by contrast, has been reported at rates up to 12 percentage points higher, and one observational study documented it in nearly a third of patients. That gap matters. It means clinicians and families should treat GHB dependence with the same urgency they would give to the most severe alcohol withdrawal presentations.
GHB Withdrawal Symptoms by Phase
GHB withdrawal symptoms follow a recognizable pattern, though severity varies widely based on how much and how often someone used.
Early Phase (6 to 24 Hours)
The first signs usually appear within 6 to 24 hours after the last dose. For very frequent users, symptoms can start even sooner. Early GHB symptoms include:
- Insomnia and restlessness
- Tremor
- Anxiety
- Nausea and vomiting
- Sweating
- Headache
- Poor appetite
Even at this stage, SA Health guidance warns that mild withdrawal can escalate quickly, especially in people who dosed frequently.
Escalation Phase (12 to 48 Hours)
Within 12 to 48 hours, the body’s rebound excitability can spike. This phase often brings:
- Rapid heart rate and high blood pressure
- Marked agitation
- Hallucinations (visual and auditory)
- Disorientation and paranoia
- Myoclonic jerks or convulsions
A systematic review of 57 withdrawal episodes found tremor in 67%, hallucinations in 63%, and tachycardia in 63% of cases. This is the window where delirium most commonly begins and where treatment resistance to benzodiazepines tends to surface.
Severe Complications (Days 2 to 7 and Beyond)
In the most serious cases, withdrawal can produce persistent delirium, psychosis, rhabdomyolysis (muscle breakdown that can damage the kidneys), and dangerous swings in blood pressure and heart rate.
A US case series highlighted rhabdomyolysis and hemodynamic instability among the worst presentations. Seizures are possible, though they appear less consistently in larger clinical cohorts than in individual case reports.
Resolution and Protracted Symptoms
Acute symptoms generally resolve within two weeks. But the story does not end there. Anxiety, depression, insomnia, cognitive fog, and motor complaints can linger for three to six months.
These protracted side effects of GHB withdrawal drive high relapse rates. One program reported about 69% of patients relapsing within three months of detox, underscoring the need for ongoing support well past the acute phase.
GHB Withdrawal Timeline at a Glance
| Phase | Time After Last Dose | Key Features |
|---|---|---|
| Early | 6 to 24 hours | Insomnia, tremor, anxiety, nausea, sweating |
| Escalation | 12 to 48 hours | Agitation, hallucinations, rapid heart rate, high blood pressure, possible delirium onset |
| Severe | Days 2 to 7+ | Persistent delirium, psychosis, rhabdomyolysis, hemodynamic swings |
| Resolution | Up to 2 weeks | Gradual improvement of acute symptoms |
| Protracted | Weeks to months | Insomnia, mood changes, cognitive difficulties, high relapse risk |
Who Faces the Greatest Risk?
Not every person who stops GHB will experience the worst outcomes. Several factors push the needle toward a more dangerous course.
Dosing frequency. People who dose every eight hours or less face higher delirium risk. Those dosing every one to three hours around the clock are at the greatest danger. Early case series linked this pattern to severe dependence and complicated withdrawal.
Daily intake. Clinical guidance suggests that daily use above 30 mL strongly predicts severe withdrawal. In one cohort, patients who developed delirium reported higher average daily intake than those who did not, though the relationship did not reach full statistical significance in multivariate analysis.
Polysubstance use. Mixing GHB with alcohol, benzodiazepines, or opioids amplifies both overdose and withdrawal risks. Most GHB-related deaths involve multiple substances. Clinicians should screen for co-depressant use during every assessment.
Psychiatric burden. In one hospital series, over half of patients needed constant mental health observation and nearly a third were detained under mental health legislation. Pre-existing anxiety, mood disorders, or trauma histories can intensify the neuropsychiatric side effects of GHB withdrawal.

GHB Detox: Treatment Approaches
GHB detox should be treated as a medical event. The speed of onset, the high rate of delirium, and the frequency of benzodiazepine resistance all argue for professional supervision in most cases.
High-Dose Benzodiazepines
Diazepam is the most common first-line choice, often given on a symptom-triggered schedule adapted from alcohol withdrawal protocols. SA Health publishes a practical seven-day taper for milder planned withdrawals, with clear escalation triggers: consult intensive care if more than 120 mg of oral diazepam is needed in the first 24 hours, and consider IV phenobarbital if the total exceeds 200 mg or if confusion appears.
The catch is that benzodiazepines target GABA-A receptors while GHB withdrawal is driven largely by GABA-B rebound. This mismatch explains why resistance is common and why early recognition of treatment failure saves lives.
Phenobarbital for Resistant Cases
When benzodiazepines are not enough, phenobarbital offers broader GABA-A activity. A 13-case series showed that phenobarbital improved symptoms in every patient without causing drug-related adverse events.
Most patients were managed safely on general wards with oral dosing, while a smaller number received IV phenobarbital in the ICU. The authors of that case series call for prospective trials to standardize dosing, but the existing data support phenobarbital as a reliable second-line option.
Pharmaceutical GHB Taper
In specialized centers, particularly in the Netherlands, clinicians replace illicit GHB with pharmaceutical-grade sodium oxybate and then gradually taper the dose. This approach achieved an 85% detox completion rate over a median of 12.5 days in one national program.
Matched comparisons suggest it produces fewer complications and less delirium than benzodiazepine-based tapers. The main barriers are regulatory access and the intensive dosing schedule of up to 12 doses per day.
Adjuncts: Baclofen and Beyond
Baclofen is a GABA-B agonist, which makes it a logical add-on for a GABA-B-driven withdrawal syndrome. Case reports describe it controlling seizures and delirium where benzodiazepines alone failed. A registered feasibility trial has been designed to test baclofen as an adjunct in both planned and unplanned GHB detox settings.
For the most extreme cases, pentobarbital or thiopental-based deep sedation in the ICU has been described. These are last-resort measures that demand airway protection and continuous monitoring.
A Note on Antipsychotics
Antipsychotics do not address the underlying receptor imbalance in GHB withdrawal. They can lower the seizure threshold and, in rare cases, trigger reactions resembling neuroleptic malignant syndrome.
If psychotic features persist despite adequate sedative therapy, antipsychotics may be added cautiously, but they should never replace the GABAergic backbone of treatment.
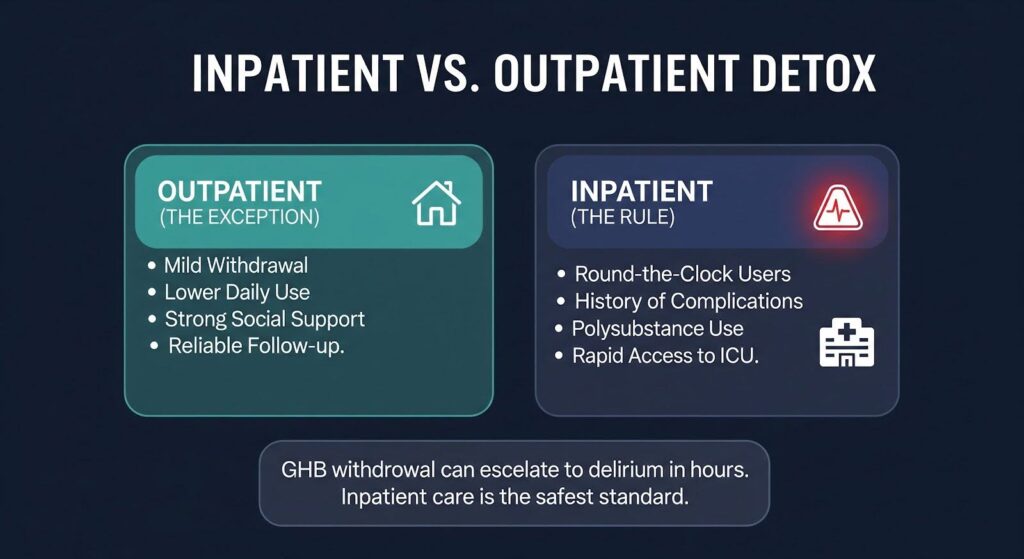
Outpatient vs. Inpatient GHB Detox
Planned, mild withdrawal in someone with lower daily use, strong social support, and reliable follow-up may be managed in the community with a structured benzodiazepine taper and close check-ins. This is the exception, not the rule.
Most people with significant GHB dependence need inpatient care. Round-the-clock users, anyone with a history of complicated withdrawal, and those using multiple depressants should be managed in a hospital setting with rapid access to intensive care. The speed at which GHB withdrawal can escalate from mild tremor to full delirium leaves little room for delayed response.
Why GHB Withdrawal Matters?
Compared to other withdrawal syndromes, GHB withdrawal sits in the highest risk tier alongside severe alcohol withdrawal. It surpasses alcohol in delirium frequency and often proves more unpredictable.
Opioid withdrawal, while deeply uncomfortable, is rarely life-threatening on its own. Stimulant withdrawal causes fatigue and low mood but not the autonomic storms seen with GHB. Benzodiazepine withdrawal can be equally severe in extreme cases, yet GHB’s compressed timeline and dosing culture add a layer of volatility that catches many clinicians off guard.
These realities mean that anyone dependent on GHB, GBL, or 1,4-butanediol should not attempt to stop abruptly without medical guidance. The window between “I feel a little anxious” and “I need a ventilator” can be disturbingly short.
Building a Path Forward
Surviving acute detox is only the first step. Protracted GHB withdrawal symptoms like insomnia, anxiety, and cognitive fog can persist for months and fuel relapse. Structured aftercare, including therapy, relapse prevention planning, and ongoing mental health support, is not optional. It is the bridge between getting clean and staying that way.
If you or someone you love is struggling with GHB dependence, waiting is the most dangerous choice you can make. Reach out to a treatment team that understands the medical complexity of this withdrawal and can match you with the right level of care. You can start by exploring Summit Wellness Group’s evidence-based treatment options today.
