Mixing oxycodone and alcohol is never safe. The FDA-approved oxycodone label warns that combining these two substances can cause profound sedation, respiratory depression, coma, and death.
This article explains exactly what happens when you mix oxycodone and alcohol, why even a low dose like 5 mg carries real danger, and what to do if an overdose is suspected.
Oxycodone and Alcohol: Why the Combination is Dangerous?
Both oxycodone and alcohol are central nervous system (CNS) depressants. That means they both slow down the brain circuits that keep you alert and breathing.
When you take them together, their effects do not simply add up. According to the NIAAA, the interaction can be synergistic, meaning the combined impact on your breathing and consciousness can exceed what either substance would cause on its own.
The CDC puts it plainly: mixing drugs is never safe because the effects may be stronger, less predictable, and potentially deadly. Oxycodone and alcohol together represent one of the most well-documented examples of dangerous polysubstance use.
How Each Substance Affects the Body?
Oxycodone works primarily by binding to mu-opioid receptors in the brain and brainstem.
This suppresses pain signals but also reduces the drive to breathe. Alcohol acts on GABA-A and NMDA receptor systems, producing sedation and impairing the brain’s ability to regulate vital functions. Although they work through different receptor pathways, both converge on the same brainstem circuits that control breathing and arousal.
That convergence is the core problem. A person may tolerate a prescribed oxycodone dose on its own, or drink moderately on a separate occasion without obvious crisis. But when both are present at the same time, the threshold for dangerous respiratory depression can drop sharply and unpredictably.
What the Human Research Shows?
The clearest direct evidence comes from a controlled study by van der Schrier and colleagues, cited by NIAAA. In that study, 20 mg of oxycodone alone reduced baseline breathing by 28 percent.
When alcohol was added at a blood alcohol concentration of 0.1 percent, breathing fell by an additional 19 percent, and apnea episodes increased. Older participants were affected more severely than younger ones.
This is not a theoretical warning. It is a measured, quantifiable worsening of breathing in real human subjects taking a single therapeutic dose of oxycodone.
What Happens If You Mix Oxycodone and Alcohol?
The effects of mixing oxycodone and alcohol occur on a spectrum, from impaired coordination to fatal respiratory arrest. Understanding that range helps explain why no amount of alcohol is considered safe while taking oxycodone.
Short-Term Effects
Even before life-threatening toxicity sets in, the combination can cause:
- Marked drowsiness and dizziness
- Impaired balance and increased fall risk
- Slowed thinking and poor judgment
- Nausea and vomiting
- Memory impairment
- Slowed reaction time
These effects matter beyond discomfort. Impaired judgment can lead a person to drink more or redose oxycodone, compounding the danger.
Alcohol also suppresses the gag reflex at higher concentrations, which means a sedated person who vomits may aspirate and suffocate. The NIAAA specifically warns that an unconscious person may choke on vomit and die from asphyxiation.
Severe and Life-Threatening Effects
At the dangerous end of the spectrum, oxycodone and alcohol interactions can produce:
- Respiratory depression and apnea
- Oxygen desaturation and hypoxia
- Loss of consciousness
- Coma
- Brain damage from oxygen deprivation
- Death
The CDC advises patients to avoid taking prescription opioids with alcohol because combining opioids with alcohol and other drugs that cause drowsiness is very dangerous.
That guidance is not a soft suggestion. It reflects the same evidence base that drives FDA labeling language.
The Sleep Risk Factor
One of the most underappreciated dangers is what happens when a person falls asleep after mixing oxycodone and alcohol. During wakefulness, the brain has a cortical backup system that helps maintain breathing even when opioids are present.
During sleep, that backup is reduced. Alcohol and opioids together can suppress medullary reflex ventilatory drive during sleep, making the combination especially lethal at night.
Clinical observations have documented severe oxygen desaturation and repeated apnea events after relatively modest opioid doses taken near bedtime.
This means the danger is not limited to the hours immediately after taking the substances. It can emerge or worsen hours later, while the person is asleep and unable to recognize or respond to distress.
Can You Mix Oxycodone and Alcohol at a Low Dose Like 5 mg?
No. Even oxycodone 5 mg and alcohol can cause dangerous effects in some people, and there is no evidence-supported safe threshold for this combination.
This is one of the most common misconceptions about oxycodone and alcohol interactions. People assume that a low prescribed dose creates a wide margin of safety. The evidence does not support that assumption for several reasons.
First, official drug information from the U.S. National Library of Medicine instructs patients not to drink alcoholic beverages while taking oxycodone. There is no carve-out for 5 mg or any other low dose.
Second, real-world clinical observations show that serious respiratory disturbances can occur at modest opioid doses, particularly during sleep and in vulnerable individuals. Documented cases include severe oxygen desaturation after doses in the range of 7.5 mg hydrocodone and 15 mg oxycodone taken at night.

While these are not exactly 5 mg, they demonstrate that danger does not require extreme doses.
Third, risk is not determined by dose alone. The following factors can make even 5 mg of oxycodone dangerous when combined with alcohol:
- Older age and reduced physiologic reserve
- Being opioid-naive with no built-up tolerance
- Having sleep apnea or other breathing disorders
- Taking benzodiazepines, gabapentinoids, muscle relaxants, or sedating antihistamines
- Drinking near bedtime
- Having liver or kidney impairment
- Using a CYP3A4 inhibitor that raises oxycodone blood levels
A preclinical study also found that low-dose ethanol reversed tolerance to oxycodone-induced respiratory depression in mice, suggesting that even opioid-experienced users cannot rely on tolerance to protect them when alcohol is present.
The correct practical answer is that 5 mg of oxycodone with alcohol should be treated as potentially dangerous, not trivially low-risk.
Oxycodone and Alcohol Interactions: What Makes the Risk Worse?
The direct oxycodone and alcohol interaction is dangerous on its own, but several additional factors can sharpen that danger considerably.
Benzodiazepines
Adding benzodiazepines to the oxycodone-alcohol combination creates a particularly hazardous triad. Oxycodone suppresses breathing via mu-opioid receptors, benzodiazepines suppress CNS activity via GABA-A receptors, and alcohol acts on both GABA-A and NMDA systems.
All three converge on the same brainstem circuits. The FDA issued boxed warnings specifically about combining opioids with benzodiazepines or other CNS depressants, including alcohol.
Gabapentinoids
Patients prescribed oxycodone for pain are often also taking gabapentin or pregabalin.
The FDA has warned that these drugs can cause serious breathing problems, especially when combined with opioids or other CNS depressants. Adding alcohol to that combination raises the risk further.
CYP3A4 Inhibitors
Oxycodone is metabolized by the CYP3A4 enzyme. Certain medications, including some antibiotics, antifungals, and even grapefruit juice, can inhibit this enzyme and raise oxycodone blood levels above expected ranges.
A patient taking oxycodone with a CYP3A4 inhibitor may already have higher oxycodone exposure than their dose suggests. Adding alcohol to that scenario can push the combination past a dangerous threshold sooner than expected.
Age, Lung Disease, and Sleep Apnea
The FDA oxycodone label specifically identifies older age, chronic obstructive pulmonary disease, and sleep-disordered breathing as factors that increase the risk of respiratory depression. Alcohol worsens all of these vulnerabilities.
Recognizing an Overdose: Oxycodone and Alcohol Effects Combined
Because both substances impair consciousness and breathing, a combined overdose can be mistaken for ordinary intoxication. A bystander may assume the person is simply very drunk and sleeping it off. The NIAAA warns explicitly that this assumption can be fatal.
Warning signs that require immediate emergency response include:
- Unconsciousness or inability to wake up
- Slow, shallow, or stopped breathing
- Choking, gurgling, or snoring sounds from an unresponsive person
- Blue or purple lips, fingernails, or skin
- Pinpoint pupils that do not react to light
- Limp body and pale or clammy skin
These signs can reflect the opioid component, the alcohol component, or both. Do not wait to see if the person improves on their own.
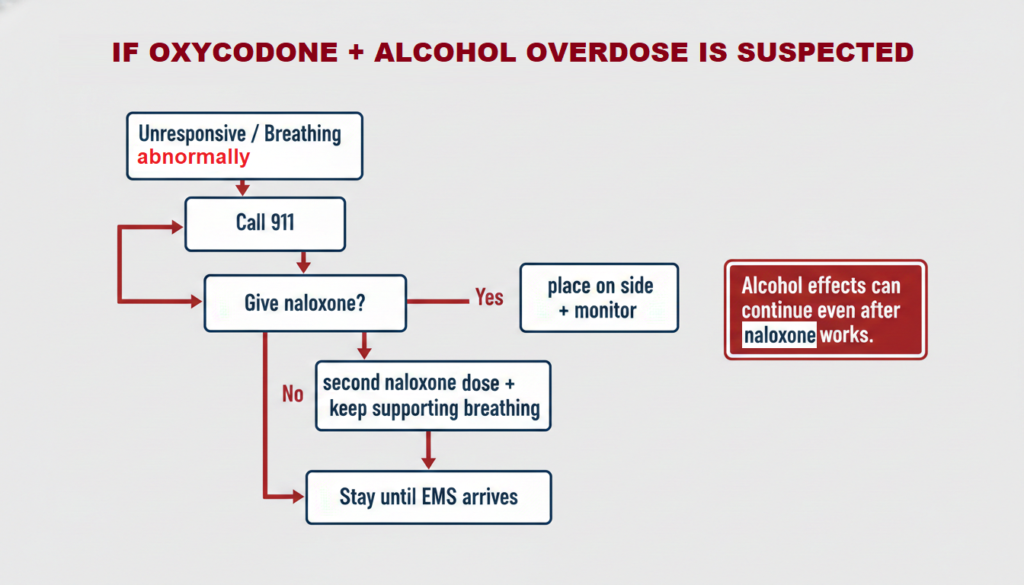
What to Do in an Emergency?
If someone who has mixed oxycodone and alcohol shows any of the warning signs above, act immediately.
1. Call 911 right away and report that the person is unresponsive or breathing abnormally.
2. Give naloxone if it is available. The CDC recommends administering naloxone whenever opioid involvement is possible.
3. Place the person on their side in the recovery position to reduce aspiration risk if they are breathing.
4. Try to keep them awake and breathing.
5. Give a second dose of naloxone after two to three minutes if there is no response, and continue until EMS arrives.
One critical limitation: naloxone reverses the opioid component of the overdose but cannot reverse alcohol toxicity. Even if naloxone improves breathing, the person still needs emergency medical evaluation. Alcohol may continue to suppress the CNS, and opioid effects can outlast naloxone’s duration of action, meaning overdose can recur.
Alcohol is Involved in a Significant Share of Opioid Deaths
The scale of this problem is not small. A CDC MMWR report found that in 2010, alcohol was involved in about 18.5 percent of opioid pain reliever abuse-related emergency department visits and 22.1 percent of opioid pain reliever drug-related deaths in the United States.
NIAAA has reported that alcohol plays a role in about one in five overdose deaths related to prescription opioids each year.
These numbers show that alcohol is not a rare or unusual cofactor in opioid harm. It is a common one. That reality reinforces why the guidance from the CDC, FDA, and NIAAA is categorical rather than cautionary: avoid the combination entirely.
The Bottom Line on Mixing Oxycodone and Alcohol
The answer to “can you mix oxycodone and alcohol” is no, and the evidence behind that answer is strong. Federal public health agencies, FDA drug labeling, controlled human research, and sleep medicine observations all point in the same direction. The combination suppresses breathing through converging mechanisms, impairs the judgment needed to recognize danger, and becomes especially lethal during sleep.
There is no safe dose threshold. There is no safe waiting period that applies universally. Even oxycodone 5 mg and alcohol can be dangerous in the wrong circumstances, and those circumstances include factors that many people do not know they have, such as undiagnosed sleep apnea, a CYP3A4-inhibiting medication, or simply being older.
If you or someone you care about is struggling with opioid use, alcohol use, or both at the same time, our professional support can make a real difference. So, reach out to our team at The Summit Wellness Group to learn about our oxycodone addiction treatment and take the first step toward recovery.
