Mixing Benadryl and alcohol is not safe, and the risks go well beyond feeling extra sleepy.
A single standard dose of diphenhydramine, the active ingredient in Benadryl, can impair driving performance as much as a blood alcohol concentration around 0.10%, which already exceeds the legal limit in every U.S. state, and adding alcohol on top of that makes things significantly worse.
This article explains exactly what happens when you combine these two substances, who faces the greatest danger, and what to do if you or someone you care about has already mixed them.
Benadryl and Alcohol: What the Interaction Actually is?
Benadryl’s active ingredient, diphenhydramine, is a first-generation antihistamine that crosses the blood-brain barrier easily and causes sedation.
It also blocks muscarinic acetylcholine receptors, which produces a range of effects beyond allergy relief, including dry mouth, blurred vision, urinary retention, and cognitive slowing. Alcohol is a central nervous system (CNS) depressant that reduces alertness, slows reaction time, and disrupts coordination.
When you take both together, the result is additive CNS depression. Official FDA labeling states plainly that diphenhydramine has additive effects with alcohol and other CNS depressants.
In practice, the combined effect often behaves as more than simple addition because both substances degrade the same safety systems at the same time: alertness, balance, reaction time, situational awareness, and protective reflexes.
This is not a subtle pharmacological footnote. It is a recognized, clinically significant interaction built into the drug’s prescribing information.
What Happens If You Mix Benadryl and Alcohol?
The most common short-term effects of combining these two substances include:
- Excessive drowsiness and sedation
- Dizziness and impaired balance
- Slowed reaction time
- Difficulty concentrating and cognitive slowing
- Poor judgment and reduced situational awareness
- Blurred vision and dry mouth
- Confusion, especially in older adults
One of the most important things to understand is that self-perceived drowsiness is not a reliable measure of actual impairment.
Research on driving performance found that people who took diphenhydramine did not rate themselves as particularly drowsy, yet their lane-keeping, hazard detection, and reaction times were significantly compromised. A person may genuinely believe they are fine to drive or handle machinery while being dangerously impaired.
The danger is not just about feeling sleepy. The combination undermines multiple systems that protect you from injury: your ability to detect hazards, respond to threats, maintain balance, form accurate memories, and judge whether you need help.
Can You OD on Benadryl and Alcohol?
Yes. You can experience an overdose-level emergency when Benadryl and alcohol are combined, even when the Benadryl dose itself is within the normal therapeutic range. The reason is that once alcohol is added, the medically relevant exposure is the interaction between two CNS depressants, not the Benadryl dose alone.
Poison Control states directly that mixing alcohol and Benadryl is a bad idea because it increases the chance of severe side effects, especially sedation.
MedlinePlus lists the overdose symptoms of diphenhydramine as including agitation, confusion, seizures, delirium, hallucinations, low blood pressure, rapid heartbeat, and loss of consciousness. Alcohol can intensify several of these features and impair the protective reflexes that might otherwise prevent a bad outcome from becoming a fatal one.
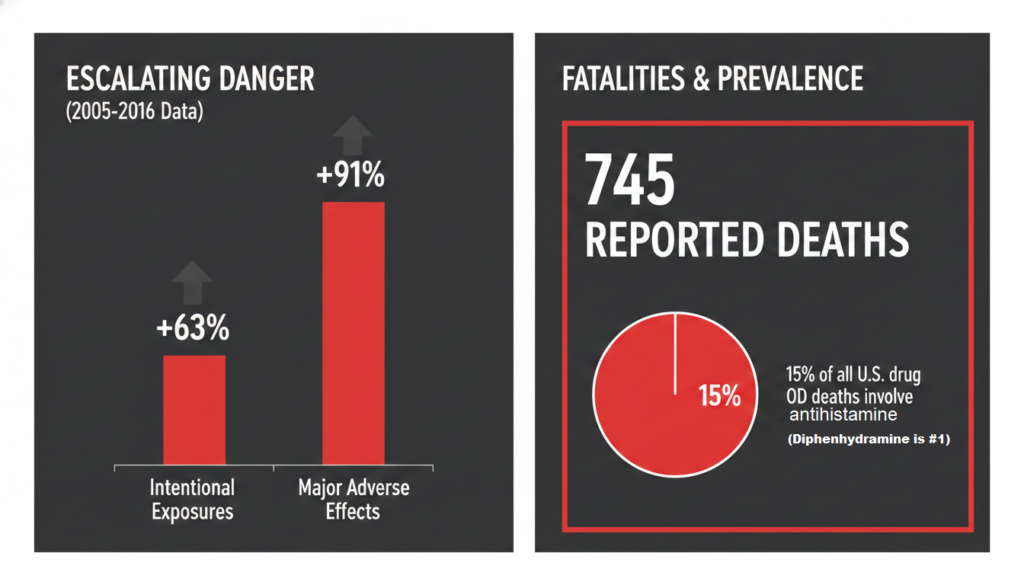
Intentional diphenhydramine exposures increased 63% between 2005 and 2016, major adverse clinical effects rose 91%, and 745 deaths were reported during that period in poison surveillance data.
A separate review found that from 2019 to 2020, antihistamines were identified in 15% of all U.S. drug overdose deaths, with diphenhydramine being the most common antihistamine involved.
Alcohol worsens overdose presentations by deepening CNS depression, impairing airway protection, masking mental-status changes, and increasing the chance that a person delays seeking help.
Severe symptoms that require emergency care
If you or someone nearby has mixed Benadryl and alcohol and experiences any of the following, call 911 immediately:
- Extreme drowsiness or inability to stay awake
- Difficulty breathing or shallow breathing
- Severe confusion or delirium
- Hallucinations
- Seizures
- Fainting or loss of consciousness
- Irregular or rapid heartbeat
- Chest symptoms
Who Faces the Greatest Risk?
Older adults
The evidence is clearest and most consistent for people over 65. The 2023 American Geriatrics Society Beers Criteria recommends avoiding first-generation antihistamines like diphenhydramine in older adults because of anticholinergic burden, reduced drug clearance, and elevated risks of confusion, falls, delirium, constipation, and urinary retention.
A recent retrospective review of first-generation antihistamine use in geriatric emergency department patients found that adverse drug effects occurred in 15% of encounters.
Delirium was the most common adverse effect at 7.7%, followed by urinary retention at 4.2%. Patients aged 85 and older had a risk ratio of 5.5 for adverse drug effects, and those with prior cognitive impairment had a risk ratio of 3.1. Notably, 92% of indications were classified as potentially inappropriate.
Diphenhydramine’s half-life may extend up to 18 hours in older adults compared with roughly four hours in younger people. This means that “waiting a few hours” before drinking may not be enough, and alcohol consumed the next morning may still overlap with residual sedation.
People taking other sedating medications
If you are also taking benzodiazepines, opioids, sleep medications, muscle relaxants, or gabapentinoids, the risk multiplies significantly. Official labeling confirms that diphenhydramine has additive effects not only with alcohol but with all CNS depressants.
Emergency department surveillance frequently finds multiple sedatives co-implicated in adverse drug events. This stacking effect can turn a manageable interaction into a life-threatening one.
People with certain health conditions
Those with respiratory disease such as asthma, COPD, or sleep apnea face greater risk because sedating drugs can worsen breathing control and airway safety. People with liver or kidney disease clear both substances more slowly.
Those with glaucoma, enlarged prostate, or cognitive impairment are more vulnerable to diphenhydramine’s anticholinergic effects, and alcohol compounds all of these risks.
Benadryl and Alcohol Together: The Hidden Exposure Problem
Many people mix Benadryl and alcohol without realizing it. Diphenhydramine is an ingredient in many “PM” pain relievers, nighttime cold formulas, and sleep aids.
Someone may drink alcohol while taking one of these products without ever intending to combine Benadryl and alcohol at all.
Common scenarios include:
- Taking a nighttime cold medicine after having drinks
- Using a “PM” pain reliever without reading the label
- Taking Benadryl to help sleep after drinking
- Using multiple OTC products that each contain diphenhydramine
Reading labels carefully is one of the most practical harm-reduction steps available.
Can You Take Benadryl and Drink Alcohol If You Wait?
The safest answer is no. If you have taken diphenhydramine, avoiding alcohol for at least 24 hours is a conservative but reasonable general rule, especially if you are older, sensitive to sedating medications, or taking other CNS depressants.
Because the drug’s half-life can extend significantly in older adults, even a full day may not be enough in some cases.
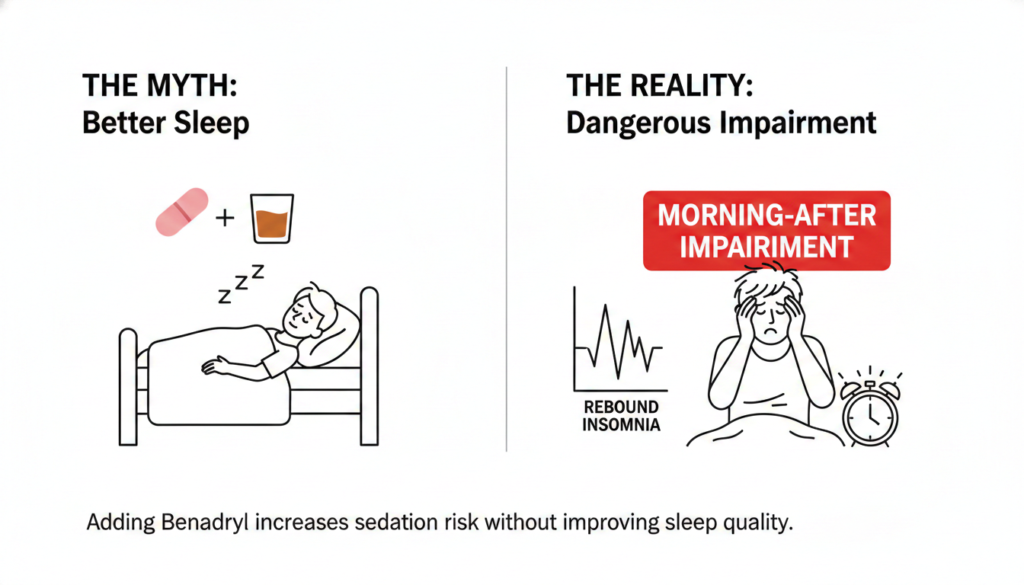
The idea of using Benadryl as a sleep aid after drinking is particularly misguided. Alcohol already disrupts sleep quality and causes rebound insomnia.
Adding diphenhydramine increases sedation risk without improving sleep outcomes, and the combination can produce dangerous morning-after impairment, especially in older adults.
Safer Alternatives Worth Knowing
For allergies, second-generation antihistamines are a much better choice when sedation is a concern or alcohol exposure is possible. Options like fexofenadine, loratadine, and cetirizine are less likely to cross into the brain and far less likely to impair thinking, alertness, and balance.
The Beers Criteria guidance specifically favors these options over diphenhydramine in older adults.
For sleep, cognitive behavioral therapy for insomnia (CBT-I) is more effective long-term than diphenhydramine-based sleep treatment and carries none of the interaction risks. If medication is needed, a doctor can recommend age-appropriate options that do not carry the same sedation and anticholinergic burden.
| Feature | Diphenhydramine (Benadryl) | Second-Generation Options |
|---|---|---|
| Sedation | High | Much lower |
| Anticholinergic burden | High | Lower |
| Brain penetration | Significant | Less |
| Fall and confusion risk in older adults | Higher | Lower |
| Beers Criteria concern | Yes, avoid in older adults | Generally safer |
| Suitability when alcohol may be present | Poor | Better, though caution still advised |
Why This Matters Beyond the Label Warning?
The Benadryl and alcohol interaction is not a theoretical concern buried in fine print. It shows up in emergency departments, poison center calls, and overdose statistics. It affects people who take a normal dose of an over-the-counter medication and then have a drink, not just people who intentionally misuse substances.
The combination is especially dangerous because impaired insight is part of the problem. A person who has taken Benadryl and had a few drinks may sincerely believe they are fine to drive, climb stairs, or take more medication, while their reaction time, balance, and hazard detection are significantly compromised.
That gap between how impaired someone feels and how impaired they actually are is one of the most clinically important features of this interaction.
The practical guidance from official labeling, toxicology resources, and geriatric prescribing standards all point in the same direction: do not combine Benadryl and alcohol, choose non-sedating antihistamines when possible, avoid first-generation antihistamines in older adults unless specifically indicated, and seek emergency care immediately if severe symptoms develop.
If you or someone you love is struggling with alcohol use or concerns about substance interactions, reaching out to a professional is the right next step. The Summit Wellness Group offers evidence-based treatment for alcohol use and related concerns, with individualized programs designed to support lasting recovery.
