Mixing Lamictal and alcohol is risky, and most people on this medication should think carefully before drinking. Lamotrigine already causes dizziness, drowsiness, and poor coordination in many patients, and alcohol amplifies every one of those effects.
Beyond the immediate impairment, alcohol can undermine the very conditions Lamictal is prescribed to treat, including epilepsy and bipolar disorder.
This article walks through what the evidence actually shows about the Lamictal and alcohol interaction, overdose risks, and what happens if you stop the medication suddenly.
Lamictal and Alcohol: Why the Combination is Risky?
Lamotrigine, sold as Lamictal, is an anticonvulsant and mood stabilizer approved by the FDA for epilepsy and maintenance treatment of bipolar I disorder.
It works by stabilizing neuronal membranes through voltage-sensitive sodium channels and reducing glutamate release, which helps prevent seizures and reduce mood-episode recurrence.
The drug is often described as better tolerated than older antiepileptic medications because it tends to cause fewer cognitive side effects. That reputation can lead patients to underestimate its real risks.
According to FDA prescribing information, lamotrigine carries a boxed warning for serious rash, including Stevens-Johnson syndrome and toxic epidermal necrolysis, and requires slow, careful dose titration from the very start.
When alcohol enters the picture, the problem is not simply that you feel a little sleepier than usual. Alcohol acts as a risk multiplier across the same neurological and psychiatric domains that lamotrigine is meant to protect.
How Lamictal and Alcohol Interact in the Body?
There is no single large human study that maps the precise pharmacokinetic interaction between lamotrigine and alcohol.
What the evidence does show, clearly and consistently, is that the two substances share overlapping effects on the central nervous system, and those effects add up.
StatPearls notes that concurrent use of lamotrigine with CNS depressants may increase the potency of CNS depression.
MedlinePlus already advises patients to avoid driving or operating machinery until they know how lamotrigine affects them. Alcohol makes that caution more urgent, not less.
Additive Sedation and Impaired Coordination
Lamotrigine commonly causes dizziness, drowsiness, blurred vision, double vision, ataxia, and slowed thinking. Alcohol independently impairs alertness, balance, reaction time, and judgment. When you combine them, the result is predictably worse than either alone.
The practical consequences include:
- Increased fall and injury risk
- Impaired driving ability
- Difficulty recognizing early signs of lamotrigine toxicity
- Poor decision-making, including missed doses
- Worsened performance at work or school
This risk is highest when starting lamotrigine, after a dose increase, or when another interacting medication has recently changed your lamotrigine blood levels.
Seizure Risk and Sleep Disruption
For patients taking lamotrigine for epilepsy, alcohol can directly oppose the medication’s purpose. Heavy drinking and alcohol withdrawal can both lower seizure threshold, meaning the brain becomes more prone to abnormal electrical activity. Poor sleep from alcohol use further compounds this risk.
As Choosing Therapy explains, alcohol may counteract lamotrigine’s seizure-protective effects even when the medication is being taken exactly as prescribed.
Patients sometimes assume that being on an anticonvulsant shields them from alcohol-related seizure risk. The evidence does not support that assumption.
Mood Destabilization in Bipolar Disorder
For patients using lamotrigine to maintain mood stability, alcohol can work directly against that goal. Alcohol may trigger agitation, depression, impulsivity, or mixed mood states, all of which lamotrigine is meant to prevent over time.
A 12-week open-label study published in PubMed followed 28 outpatients with bipolar disorder and alcohol dependence. Lamotrigine was associated with significant improvements in depressive symptoms, manic symptoms, overall psychiatric functioning, and alcohol craving.
The drug was well tolerated with no dropouts due to adverse events. This finding is encouraging, but it should not be read as proof that drinking while on lamotrigine is safe.
The study evaluated lamotrigine as a treatment for people who had alcohol dependence, not as evidence that ongoing alcohol use alongside the medication is harmless.
Lamictal and Alcohol Side Effects to Watch For
The overlap between lamotrigine’s known adverse effects and alcohol intoxication creates a specific danger: you may not be able to tell which substance is causing a symptom, and that delay in recognition can matter clinically.
Common signs that alcohol is worsening lamotrigine tolerability include unusual sleepiness, dizziness that feels stronger than expected, blurred or double vision, nausea, poor coordination, and slowed thinking.
These are all documented lamotrigine adverse effects listed in DailyMed prescribing information, and alcohol can make each one worse.
More serious warning signs that need prompt medical attention include:
- Severe ataxia or inability to walk steadily
- Repeated vomiting
- Pronounced confusion or loss of consciousness
- Breakthrough seizures
- Sudden worsening of mood or suicidal thoughts
- Any new rash, especially with fever, mouth sores, or blistering
- Breathing difficulty, particularly if other sedating medications are involved
A new rash in a patient on lamotrigine should never be casually attributed to alcohol or a minor allergy. It requires urgent clinical evaluation every time.
Lamictal and Alcohol Overdose: What the Evidence Shows?
Lamotrigine overdose is sometimes described as broadly mild, but that characterization is outdated and incomplete. The evidence now shows that large overdoses can be severely toxic, and alcohol co-ingestion makes the clinical picture harder to read.
A 2018 systematic review of lamotrigine overdose cases found that among published severe cases, seizures occurred in 55%, a Glasgow Coma Scale score of 8 or below in 20%, hypotension in 12%, and wide-complex tachycardia or cardiac arrest in 6%.
These figures reflect a selected group of serious published cases rather than all overdoses, but they clearly show that severe toxicity is real.
More recent prospective data from the ATOM-10 study, which followed 54 patients with large lamotrigine overdoses of 2 grams or more, found sedation in 81%, endotracheal intubation in 54%, tachycardia in 72%, hypotension in 39%, and seizures in 20%.
These are not rare edge cases. In large overdoses, serious toxicity is common.
The systematic review also found that cardiovascular toxicity in adults appeared primarily at serum concentrations above about 25 mg/L, suggesting a concentration-dependent threshold for the most dangerous effects.
When Alcohol is Also Involved?
A published case report by Schwartz and Geller described a patient who ingested lamotrigine and ethanol together and developed coma requiring ventilatory support, paradoxical seizure activity, and altered mental status.
Alcohol does not protect against lamotrigine toxicity. It can mask it, delay recognition, and add its own CNS depression on top.
If someone appears sedated or confused after possibly taking extra lamotrigine and drinking, do not assume it is simple intoxication. Lamotrigine toxicity can progress to seizures, hypotension, and cardiac conduction problems. Emergency evaluation is appropriate.
Drug Interactions That Change Your Lamictal Risk
The Lamictal and alcohol interaction does not happen in isolation. Lamotrigine has several major drug interactions that can shift blood levels dramatically, and those shifts change how dangerous alcohol becomes.
| Interacting Factor | Effect on Lamotrigine | Approximate Change |
|---|---|---|
| Valproate | Raises levels | More than 2-fold increase |
| Estrogen-containing oral contraceptives | Lowers levels | About 50% decrease |
| Stopping estrogen-containing oral contraceptives | Raises levels | Often clinically significant |
| Pill-free week of combined oral contraceptives | Raises levels transiently | May double by end of week |
| Carbamazepine, phenytoin, phenobarbital, primidone, rifampin | Lower levels | About 40% decrease |
| Lopinavir/ritonavir | Lowers levels | About 50% decrease |
Sources: Guideline Central, NPS MedicineWise, DailyMed prescribing information.
Valproate is the most important interaction. It inhibits lamotrigine’s metabolism and can more than double blood levels. A patient already at higher lamotrigine exposure who then drinks alcohol is much closer to the toxicity threshold. Dizziness, ataxia, blurred vision, and somnolence become more likely and more severe.
Estrogen-containing oral contraceptives create a different problem. They can cut lamotrigine levels by about half during active hormone weeks, reducing seizure and mood protection.
During the pill-free week, levels can rise sharply, sometimes doubling by the end of that interval. Alcohol during either phase worsens the situation: it can amplify toxicity symptoms during high-level periods and further destabilize seizure or mood control during low-level periods.
Lamictal and Alcohol Withdrawal: What Actually Happens?
The question of lamotrigine withdrawal is more nuanced than many sources suggest. The formal evidence does not strongly support a classic, well-defined withdrawal syndrome comparable to what occurs with alcohol, opioids, or benzodiazepines.
What is clearly established is that abrupt discontinuation can cause breakthrough seizures in epilepsy and mood destabilization in bipolar disorder.
StatPearls states that the risk of withdrawal seizures is reduced by tapering over two weeks rather than stopping suddenly. That recommendation is grounded in solid clinical evidence.
Patients and some clinical sources also report transient symptoms after stopping lamotrigine, including anxiety, headache, dizziness, irritability, nausea, fatigue, and sleep disturbance.
These typically begin within days and often improve within one to two weeks. They are real and worth knowing about, but they should be understood as rebound or discontinuation effects rather than a formally characterized withdrawal syndrome.
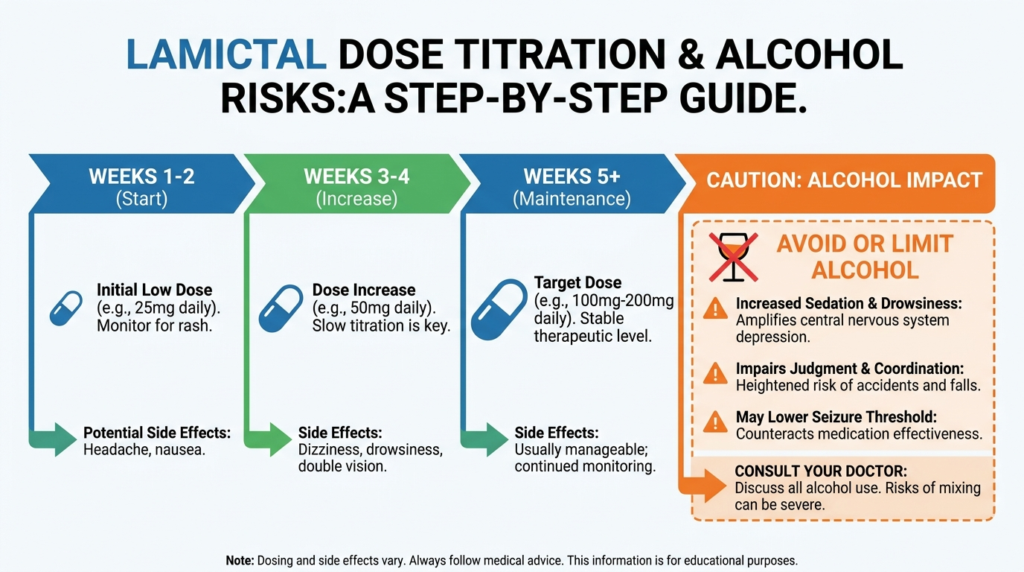
The Restart Problem!
One of the most underappreciated risks with lamotrigine is what happens after missing several days. Resuming the previous full dose after a multi-day gap may not be safe.
The body has effectively lost its gradual adaptation to the drug, and restarting at a high dose can recreate the conditions that increase serious rash risk, including Stevens-Johnson syndrome.
Patients who have missed several days should contact their prescriber before resuming, rather than simply picking up where they left off.
If someone is also reducing heavy alcohol use at the same time they stop lamotrigine, the risks compound. Alcohol withdrawal itself can provoke seizures.
Lamotrigine discontinuation removes seizure protection and can destabilize mood. Stopping both at once without medical supervision is not safe.
Who Faces the Highest Risk From Mixing Lamictal and Alcohol?
Not every person on lamotrigine faces identical risk from alcohol, but some groups face substantially higher danger:
- People just starting lamotrigine or recently increasing their dose
- Patients with epilepsy, especially those with recent breakthrough seizures
- Patients with unstable bipolar disorder
- Anyone also taking valproate, which raises lamotrigine levels significantly
- Reproductive-age women on estrogen-containing contraceptives, given the large level fluctuations
- People taking other CNS depressants such as opioids, benzodiazepines, or pregabalin
- Those with a history of heavy or binge drinking
- Older adults and people with liver or kidney problems
For patients in these groups, the evidence supports a clear recommendation to avoid alcohol. For others in stable situations, the evidence does not prove that any alcohol use is categorically forbidden, but it does not support casual drinking either.
The safest approach is to discuss alcohol use openly with your prescriber rather than making that call alone.
What to Do If You Are Concerned?
If you are taking lamotrigine and struggling with alcohol use, that combination deserves honest attention. Alcohol can quietly erode the protection lamotrigine provides, make side effects worse, and increase the chance of a serious event. The fact that you may feel fine most of the time does not mean the risk is absent.
If you or someone you care about is dealing with alcohol use alongside a psychiatric or neurological medication, speaking with our treatment professional is a practical next step.
The Summit Wellness Group addresses both substance use and mental health conditions together. So, you can learn more about our substance interactions treatment and find support that fits your situation.
