Mixing prednisone and marijuana is a question many patients face when managing pain, sleep problems, or anxiety alongside a steroid prescription.
The short answer is that some people do use both without obvious immediate harm, but the combination is not risk-free, and certain cannabis products, especially those rich in CBD, can meaningfully change how prednisone works in your body.
This article walks through what the evidence actually shows so you can have an informed conversation with your doctor.
Prednisone and Marijuana: What the Research Shows?
Prednisone is a synthetic corticosteroid prescribed for a wide range of conditions, from asthma and rheumatoid arthritis to inflammatory bowel disease and transplant care. It works by suppressing inflammation and dialing down immune activity.
That power comes with a real side-effect burden. Even short courses can raise blood sugar, disturb sleep, trigger mood swings, and increase infection risk.
A large claims-data analysis summarized by the AAFP found that short systemic steroid courses were linked to a roughly fivefold increase in sepsis risk and a nearly twofold increase in fracture risk within 5 to 30 days of starting treatment.
Marijuana, meanwhile, is not one drug. Smoked flower, THC edibles, CBD oils, and balanced THC/CBD products all behave differently in the body.
That distinction matters enormously when you ask whether prednisone and marijuana interact, because the evidence points in very different directions depending on which cannabis product you are talking about.
How Prednisone and Marijuana Can Interact?
The most credible interaction concern involves a liver enzyme called CYP3A. Prednisone is converted to its active form, prednisolone, and both are partly cleared through CYP3A-related pathways. CBD, the non-intoxicating cannabinoid found in many cannabis products, is a known inhibitor of that same enzyme.
A human crossover study in 18 healthy adults found that a CBD-dominant brownie containing 640 mg of CBD increased exposure to a CYP3A probe drug by 56%, while a THC-dominant brownie produced no significant effect on the same enzyme.
That is direct human evidence that high oral CBD can inhibit CYP3A in a clinically meaningful way.
A peer-reviewed review published in PMC specifically named corticosteroids such as prednisolone as drugs metabolized by CYP3A and warned that CBD, as a potent inhibitor of that pathway, may decrease glucocorticoid clearance and increase the risk of steroid-related side effects.
The NCBI Bookshelf monograph on cannabidiol confirms that CBD is metabolized by CYP2C19 and CYP3A4 and can alter the toxicity or efficacy of other drugs through enzyme inhibition.
THC alone appears less likely to drive this kind of pharmacokinetic change. That does not make THC harmless, but it does mean the interaction story is more nuanced than a blanket warning about “weed and prednisone.”
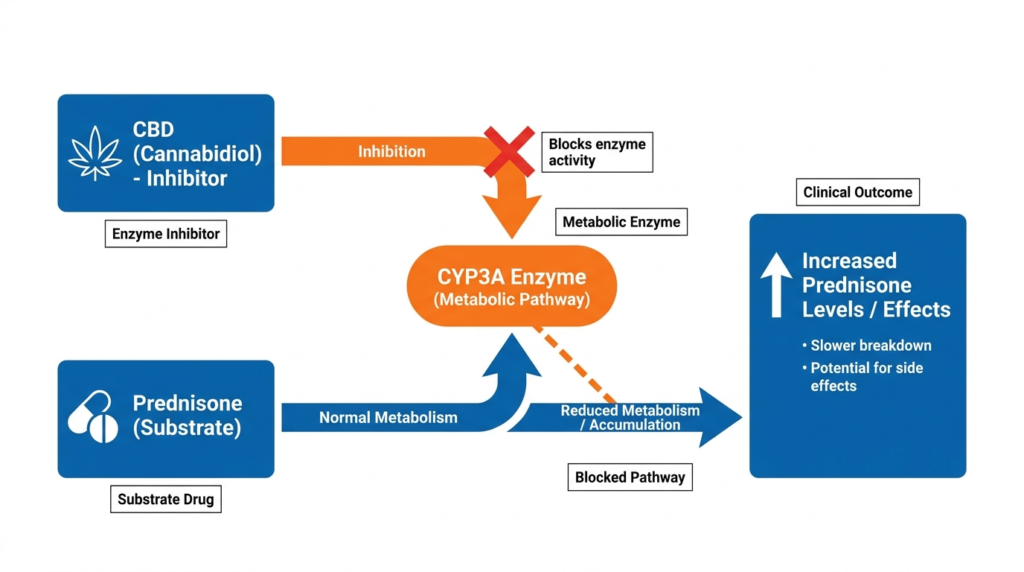
What Happens If CBD Raises Prednisone Exposure?
If CBD slows the clearance of prednisone or prednisolone, you effectively get more steroid effect than your dose was intended to deliver. That could mean:
- worse insomnia and anxiety
- higher blood sugar readings
- more fluid retention
- stronger appetite increase and weight gain
- greater immune suppression
- a harder time tapering off the drug
These outcomes are mechanistically consistent with steroid toxicity, even though no dedicated prednisone-plus-CBD clinical trial has measured each one directly.
Smoking Weed and Taking Prednisone: The Specific Question
Many people asking about prednisone and weed are thinking specifically about smoking. The pharmacokinetic picture here is actually somewhat reassuring on one narrow point.
A controlled study found that cigarette smoking did not significantly alter the pharmacokinetics of prednisone, prednisolone, or dexamethasone in healthy male adults. Smoking itself is not the main driver of enzyme-based interaction.
That same study, however, found roughly two- to threefold variability in oral steroid clearance between individuals even without any cannabis exposure.
That baseline variability matters because it means some patients are already at the high end of steroid exposure before any interaction is added.
Smoking marijuana while on prednisone is still generally a poor choice for reasons that have nothing to do with enzyme pathways:
- Prednisone suppresses immune function, and smoking can worsen respiratory vulnerability and increase the risk of lung-related complications.
- Long-term corticosteroid use is already associated with bone loss. Some sources cite a possible link between heavy cannabis use and lower bone density, which could compound skeletal risk in patients on prolonged steroid therapy.
- Smoked cannabis can mask symptoms. A cough or respiratory change in someone on prednisone may deserve medical attention rather than casual attribution to smoking.
So the clearest statement on smoking weed and taking prednisone is this: smoking probably does not dramatically change prednisone blood levels the way oral CBD can, but it is still not a good idea given the immune, pulmonary, and bone-health context.
Prednisone and Weed Interaction: Side Effects That Can Overlap
Even when cannabis does not significantly alter prednisone pharmacokinetics, it can still change how the drug’s side effects feel. That is a pharmacodynamic interaction, and it runs in both directions.
Prednisone commonly causes insomnia, anxiety, irritability, mood swings, appetite increase, and in some cases confusion or rare psychosis-like symptoms at higher doses, as noted in StatPearls and clinical guidance sources. Cannabis can overlap with every one of those domains.
Some patients feel that marijuana helps them sleep or feel calmer during a prednisone course. That subjective relief is real for some people, but it does not mean the combination is safer.
A systematic review of long-term medical cannabis harms found psychiatric adverse events in about 13.5% of users, with anxiety in about 7.4% and paranoia in about 5.6%. Those numbers sit alongside prednisone’s own psychiatric risk profile, and the two can add up.
THC can also stimulate appetite, which may amplify one of prednisone’s most common complaints rather than offset it.
And when both substances are on board, it becomes harder to tell whether a new symptom reflects a steroid side effect, a cannabis effect, an interaction, or a sign of something that needs medical attention.
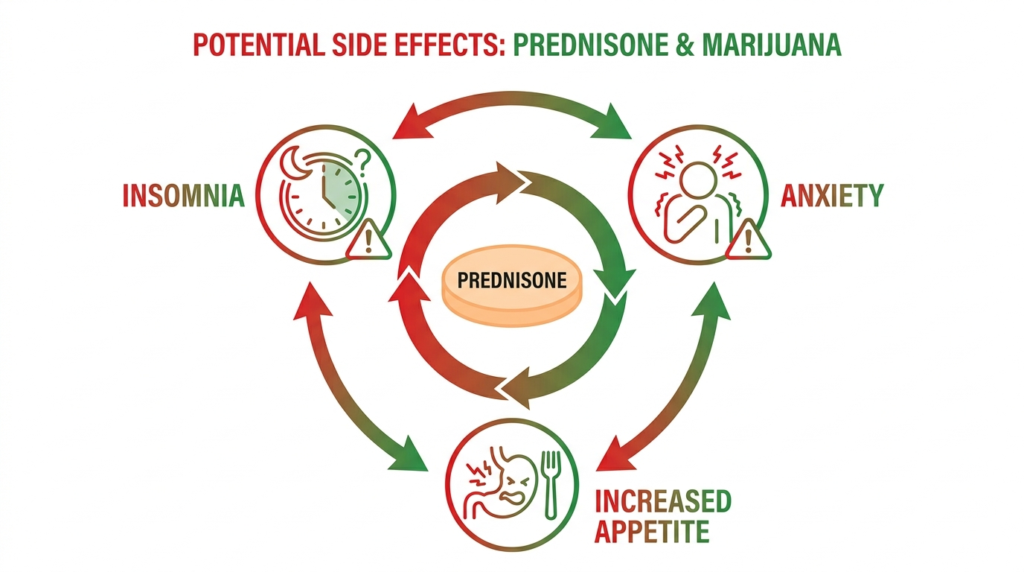
Who Faces the Most Risk from Mixing Marijuana and Prednisone Together?
Risk is not equal across all patients or all cannabis products. The following situations call for the most caution:
- Daily or high-dose oral CBD use alongside any prednisone regimen
- High-dose prednisone, generally considered 40 mg per day or more
- Long-term steroid therapy, where cumulative toxicity is already a concern
- Diabetes or prediabetes, since both prednisone and possible steroid-exposure increases can worsen blood sugar
- A history of anxiety, panic, mood disorders, or prior steroid psychiatric reactions
- Active respiratory disease or recurrent infections
- Osteoporosis or high fracture risk
- Multiple medications that also rely on CYP3A metabolism
A patient taking a short five-day prednisone burst and occasionally using a low-THC product with no meaningful CBD is in a very different risk category than someone on chronic high-dose prednisone using daily oral CBD oil. The evidence supports treating those two situations differently.
Can You Smoke Weed and Take Prednisone? A Practical Summary
The honest answer is that some people do, and not everyone experiences obvious immediate harm. But “not immediately obvious” is not the same as safe, and the evidence does not support casual reassurance.
Here is what the research actually supports:
- CBD-rich products are the main pharmacokinetic concern. Oral CBD oils, capsules, gummies, and mixed THC/CBD edibles carry the clearest risk of raising prednisone exposure through CYP3A inhibition.
- THC-dominant products are less likely to change prednisone blood levels but can still worsen mood, sleep, appetite, and cognitive clarity.
- Smoking marijuana probably does not strongly alter prednisone pharmacokinetics by itself, but it remains a poor choice in an immunosuppressed patient with elevated infection and bone-health risk.
- The combination can make side effects harder to interpret, which matters when prednisone management depends on recognizing problems early.
- There is no good evidence that cannabis can replace prednisone or serve as a reliable steroid-sparing treatment in real-world use today.
A 2024 systematic review in Frontiers in Pharmacology identified more than 600 cannabinoid users across 31 papers showing direct links between cannabis use and changed drug metabolism or therapeutic outcomes. The phenomenon is clinically real, even if the specific prednisone data remain limited.
The most evidence-consistent position is selective caution. Occasional low-CBD cannabis may be tolerable for some patients during a short steroid course.
CBD-rich and heavily smoked use during significant prednisone therapy is a different matter entirely, and co-use in high-risk patients should ideally happen only after a clinician has reviewed the full picture.
Why This Matters Beyond the Immediate Question?
Prednisone is a powerful drug with a narrow comfort margin in many patients. Its side effects are dose-sensitive, time-sensitive, and highly variable between individuals. Adding cannabis, especially CBD-containing products, introduces another layer of variability into an already unpredictable pharmacokinetic picture.
If you are using marijuana while taking prednisone and you notice worsening insomnia, more anxiety, higher blood sugar, unusual mood changes, or difficulty tapering, the combination may be a contributing factor. That is worth raising with your prescriber rather than managing alone.
If your cannabis use has become a way of coping with pain, anxiety, or sleep problems that feel out of control, that pattern is worth exploring on its own terms. Sometimes what starts as symptom management becomes something more complicated.
If you are concerned about how cannabis use is affecting your health or your relationship with substances, speaking with our specialist can help you sort through what is going on and find a path forward.
Reach out to our team to learn more about our addiction treatment programs and get the support you deserve.
