Mixing cocaine and alcohol is more dangerous than using either substance alone, and the reason goes deeper than simply combining two harmful drugs.
When both are present in the body at the same time, the liver produces a third active compound called cocaethylene, which lasts longer than cocaine and carries greater toxicity for the heart and liver.
This article explains exactly what happens during co-use, why the experience can feel deceptively different, and which warning signs demand immediate medical attention.
Cocaine and Alcohol: What Actually Happens in Your Body?
Most people assume a stimulant and a depressant cancel each other out. The evidence says otherwise.
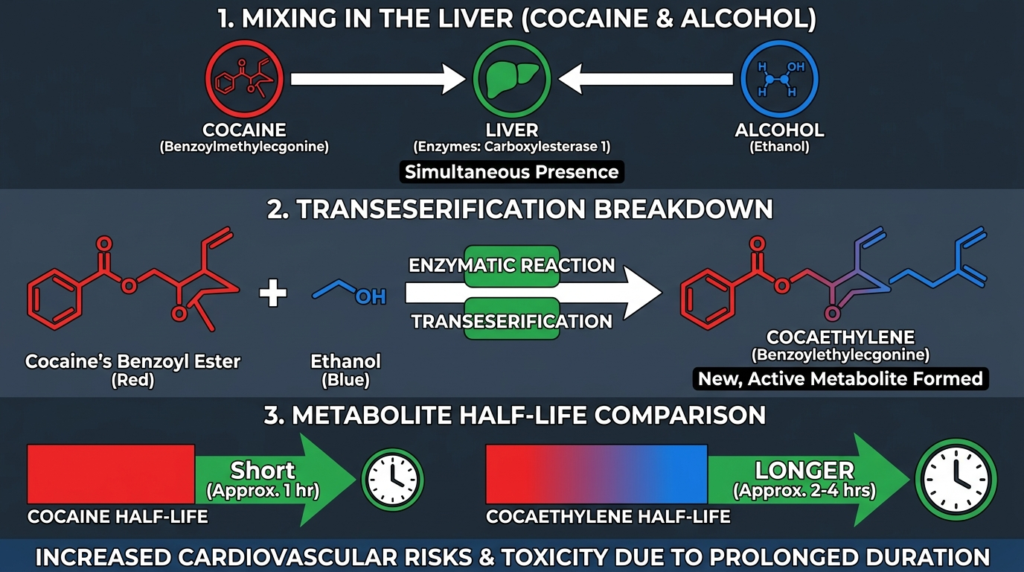
When cocaine and ethanol are present simultaneously, the liver diverts part of cocaine’s normal breakdown pathway toward a process called transesterification, producing cocaethylene, a psychoactive metabolite that does not form when either substance is used alone.
This matters for several reasons. Cocaethylene has cocaine-like effects on the brain, stays active roughly twice as long as cocaine itself, and is considered more toxic to the cardiovascular and hepatic systems than cocaine alone.
Human studies found that about 17% of a cocaine dose is converted into cocaethylene during co-use, while urinary excretion of a standard cocaine metabolite dropped by about 48%, meaning the body clears the active compounds more slowly.
The practical result is a longer, more intense exposure to toxic compounds, not a balanced or softened experience.
Why Mixing Cocaine and Alcohol Feels Different?
One of the most dangerous features of this combination is that it can feel better than either drug alone. Human laboratory studies found that people reported the cocaine-plus-alcohol mixture as more pleasurable and more intoxicating than either substance by itself.
That enhanced reward is not a sign of safety. It reflects the formation of cocaethylene and altered metabolism, both of which increase toxic burden.
Several overlapping effects explain why the experience feels distinct:
- Cocaethylene has a plasma elimination half-life of about 2 hours compared with roughly 1 hour for cocaine, so the high lasts longer
- Alcohol reduces the subjective sense of sedation, which can make a person feel more alert and in control than they actually are
- The combination blunts awareness of cocaine-related distress signals such as chest tightness, overheating, or racing heart
- Users may keep drinking because they do not feel drunk enough, and keep using cocaine because the edge feels softer
- Redosing stacks cocaethylene exposure before earlier doses have cleared
This false sense of control is not a minor side effect. It is a central mechanism of harm. A person who feels capable is more likely to drive, take more substances, delay calling for help, or miss the early signs of a cardiac or neurologic emergency.
The Cardiovascular Danger: Where the Evidence is Strongest?
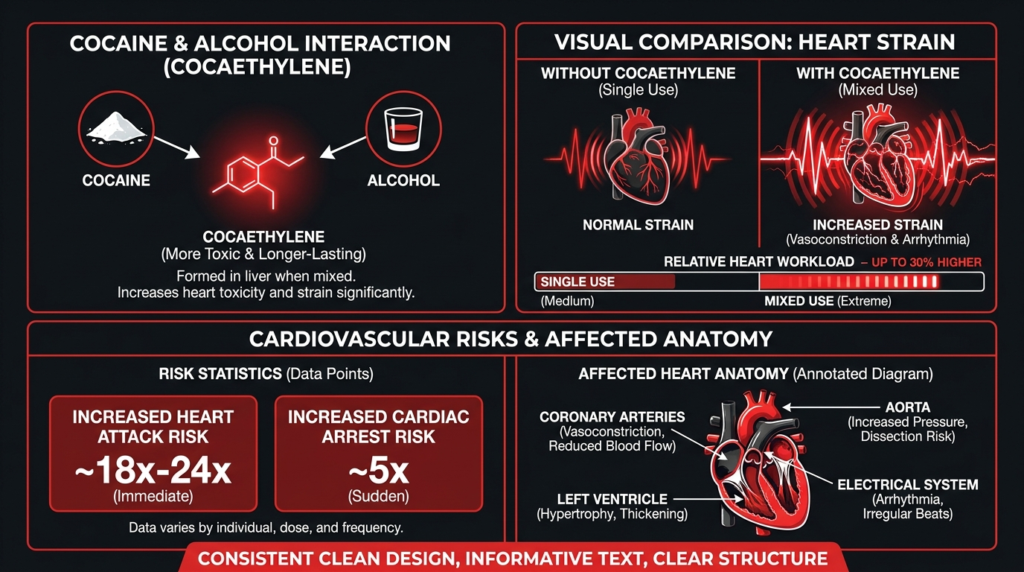
The clearest and most serious evidence against mixing cocaine and alcohol involves the heart. Cocaine alone already strains the cardiovascular system through tachycardia, hypertension, coronary vasospasm, and increased myocardial oxygen demand.
Adding alcohol and cocaethylene to that picture makes things measurably worse.
A 2024 systematic review concluded that simultaneous cocaine and alcohol use increases cardiovascular fatality risk compared with cocaine alone, even accounting for variation in how symptoms present across different patients.
The same review reported that cocaethylene may contribute to cardiac arrest and myocardial injury through cardiac ion-channel inhibition, and that its presence is associated with an 18 to 25 times higher risk of sudden death compared with cocaine use without cocaethylene.
Emergency department data make this concrete. A 2023 cohort analysis of 199 adult overdose patients with cocaine-positive toxicology found that cardiac arrest occurred in 6.1% of patients with cocaethylene exposure compared with 0.67% in those with cocaine alone.
Initial lactate levels were also higher in the cocaethylene group, indicating greater physiologic stress on the body.
Chest pain is the most common presenting complaint among cocaine users in emergency settings, and cocaine-associated myocardial infarction occurs in roughly 0.7% to 6% of cases depending on the population.
That range is not small enough to dismiss. Chest pain after co-use should be treated as a cardiac emergency until a clinician says otherwise.
Neurologic Risks: Stroke and Seizure
The combination also raises the risk of serious brain events. A review of cocaine and ethanol co-use found increased incidence of cerebral infarction and intracranial hemorrhage associated with the combination compared with either drug alone.
Cocaine causes vasospasm and blood pressure surges that can trigger stroke, and alcohol impairs the judgment needed to recognize early neurologic warning signs.
More recent observational data from a study of unstably housed women found cocaethylene positivity associated with stroke, with an adjusted odds ratio of 3.22, though that study had limitations including small sample size.
The finding aligns with the broader mechanistic concern and should not be dismissed.
Seizures are also a recognized complication of severe cocaine toxicity and can occur even in people who have used cocaine before without incident.
Warning Signs That Need Immediate Attention
The following signs after cocaine and alcohol co-use require emergency evaluation or an immediate call to emergency services. Do not wait to see if they pass on their own.
- Chest pain or pressure
- Shortness of breath
- Irregular pulse or palpitations
- Seizure
- Confusion or altered mental status
- Severe agitation
- High body temperature or overheating
- New weakness on one side, facial droop, or trouble speaking
- Sudden severe headache
- Collapse or inability to be awakened
If the person collapses, has a seizure, cannot be awakened, or stops breathing normally, call 911 immediately. If the situation is serious but the person is conscious and stable, Poison Help at 1-800-222-1222 can provide expert guidance.
The MedlinePlus drug use first aid guide recommends checking airway, breathing, and pulse, placing an unconscious but breathing person in the recovery position, keeping them calm and warm, and bringing any containers or information about what was taken to help emergency responders.
The Addiction Cycle: Why Co-Use Repeats Itself?
The enhanced pleasure and prolonged high that people report from mixing cocaine and alcohol are not random.
They reflect a real pharmacologic state that the brain can learn to seek out. Among people who use cocaine, alcohol use is common, and dependence on both substances often develops together.
Alcohol can also act as a direct trigger for cocaine relapse. Someone trying to reduce cocaine use may find that drinking pulls them back toward it, because the two substances are linked in the brain’s reward and memory systems.
This means treating cocaine use while leaving alcohol use unaddressed is often not enough. The pattern of concurrent substance use needs to be addressed as a whole.
Liver Damage: A Risk That Builds Over Time
The heart gets most of the attention, but the liver is also at serious risk. Because cocaethylene is formed in the liver, that organ bears the direct burden of the metabolic interaction.
A 2022 human study examined cocaethylene levels and liver health in 649 participants.
Those with detectable cocaethylene in their blood had 3.17 times the odds of liver fibrosis compared with people who did not use cocaine, after adjusting for HIV status, hepatitis C infection, and other relevant factors.
This is one of the strongest pieces of human evidence showing that co-use causes chronic organ damage, not just acute toxicity.
The implication is that the danger does not end when the night is over. Repeated co-use may quietly accumulate liver injury over time, even in the absence of obvious symptoms.
Take Your Next Step Towards Real Recovery, Call Now!
The research across pharmacology, emergency medicine, cardiology, and liver disease all points in the same direction. Mixing cocaine and alcohol is not a matter of two risks adding together.
It creates a third active compound, changes how the body processes both substances, amplifies subjective reward in ways that encourage more use, and produces disproportionately greater harm to the heart, brain, and liver.
The feeling that the combination is smoother or more enjoyable is part of the danger, not a sign that it is working safely. That sensation reflects cocaethylene formation and altered metabolism, both of which increase the risk of cardiac arrest, sudden death, stroke, and chronic organ damage.
If you or someone you care about is struggling with cocaine and alcohol use together, integrated treatment that addresses both substances at the same time gives the best chance of real recovery.
Reach out to the team at Summit Wellness Group to learn about evidence-based programs designed for exactly this kind of complex, co-occurring substance use.
