Mixing methadone and alcohol is medically dangerous and can be fatal. Both substances depress the central nervous system, and when combined, they can slow breathing to a life-threatening degree, cause coma, or lead to death.
SAMHSA states plainly that patients should not consume alcohol while taking methadone, and this article explains exactly why that warning exists, what happens in the body, and what to do in an emergency.
Methadone and Alcohol: Why This Combination is Unsafe?
Methadone is a long-acting full opioid agonist used to treat opioid use disorder and manage pain. It works by reducing withdrawal symptoms and cravings over an extended period, which makes it a cornerstone of opioid treatment programs.
But that same long-acting profile creates a serious problem when alcohol enters the picture.
FDA prescribing information states that combining methadone with alcohol or other central nervous system depressants may result in profound sedation, respiratory depression, coma, and death.
That is not cautious legal language. It reflects real pharmacology: two depressants acting on the same brain systems at the same time.
MedlinePlus drug information reinforces this, telling patients directly that alcohol worsens methadone’s side effects and increases the risk of serious, life-threatening breathing problems, sedation, and coma.
How Methadone Works in the Body?
Methadone has a half-life of roughly 15 to 55 hours, which is far longer than most other opioids.
According to National Health Care for the Homeless Council guidance, this prolonged half-life creates an extended window during which sedation and respiratory depression can occur, especially during treatment initiation or dose changes.
This long duration matters for three practical reasons:
- Methadone can build up in the body if doses are increased too quickly, raising toxicity risk before a person notices anything is wrong.
- Its respiratory depressant effects can peak later than expected, meaning a person may feel fine initially and then deteriorate hours afterward.
- Naloxone, the overdose reversal medication, has a much shorter half-life than methadone, so a person who appears to recover after naloxone may relapse into respiratory depression.
What Alcohol Adds to the Risk?
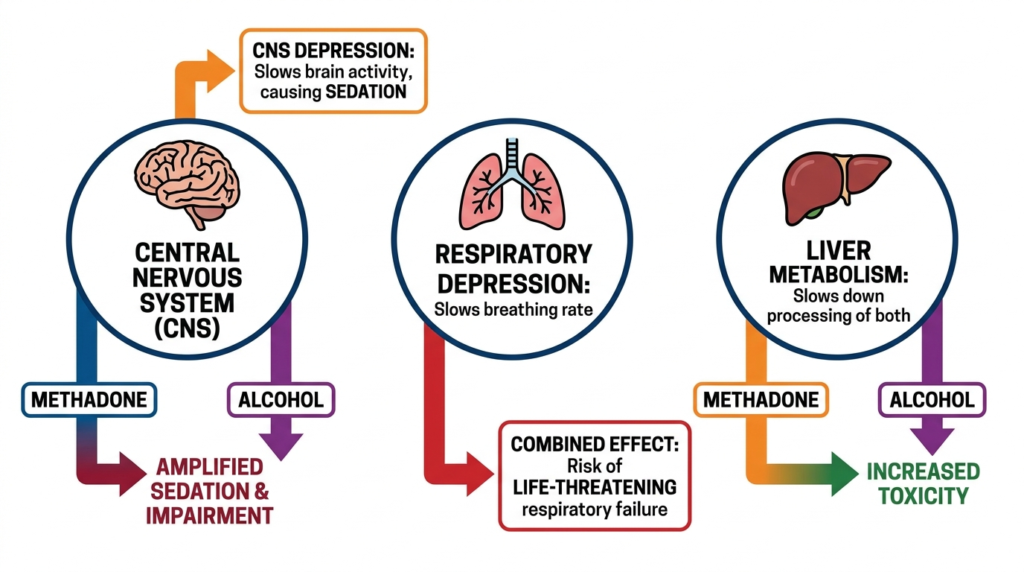
Alcohol is a central nervous system depressant. On its own, it slows reaction time, impairs judgment, and at high doses suppresses breathing. When combined with methadone, the depressant effects stack. The result can be:
- slower and shallower breathing than either substance would cause alone
- deeper sedation and reduced ability to stay awake
- impaired airway reflexes, raising the risk of choking
- reduced arousal from low oxygen levels, so the body does not signal distress effectively
WHO interaction guidance specifically lists alcohol as a substance that increases sedation and respiratory depression when used with methadone. This is not a theoretical concern. It is a documented pharmacologic interaction.
Side Effects of Mixing Methadone and Alcohol
The methadone and alcohol interaction produces a predictable set of side effects, ranging from uncomfortable to fatal. Understanding them helps patients and bystanders recognize danger early.
Common worsened side effects include:
- excessive drowsiness or difficulty staying awake
- dizziness and poor coordination
- slowed thinking and confusion
- nausea or vomiting
- low blood pressure and faintness
- impaired driving ability
Serious and life-threatening effects include:
- slow, shallow, or stopped breathing
- inability to wake up
- blue or purple lips and fingernails
- gurgling or choking sounds
- coma
- death
MedlinePlus lists breathing problems, sedation, and coma as the primary serious risks when alcohol is added to methadone.
The CDC identifies unconsciousness, slow or absent breathing, pinpoint pupils, and discolored skin as key overdose signs that require immediate emergency response.
When Risk is Highest?
Not every moment on methadone carries equal risk. The alcohol and methadone interaction is most dangerous at specific times.
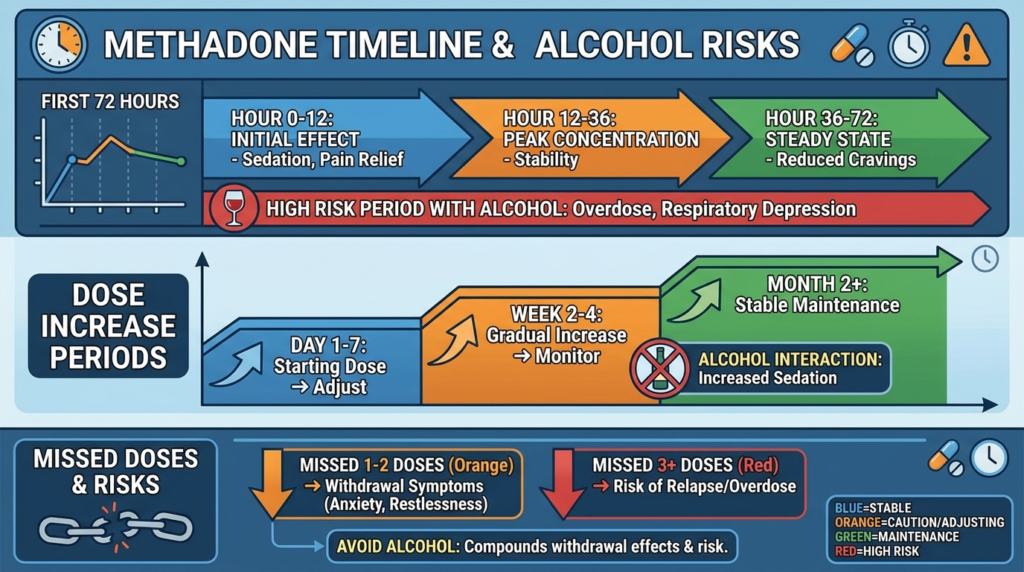
The first 24 to 72 hours after starting methadone and any period after a dose increase are especially high-risk, because breathing problems are most likely during these windows.
A retrospective cohort study of nearly 2,900 methadone-treated patients found that drug-related poisoning mortality was about four times higher in the first four weeks after leaving treatment and about three times higher in the first four weeks of starting treatment, compared with stable treatment periods.
Missed doses also reduce opioid tolerance. If a person restarts methadone after several missed days and then drinks alcohol, the previously tolerated dose may now be dangerous.
| High-Risk Period | Why Alcohol Is Especially Dangerous |
|---|---|
| First 24 to 72 hours of treatment | Methadone effects are still being assessed; alcohol adds unpredictable CNS depression |
| After dose increases | New dose may already raise sedation; alcohol can tip the balance into overdose |
| After missed doses | Reduced tolerance means the usual dose may now be too strong |
| Weeks 1 to 4 after leaving treatment | Loss of tolerance and relapse risk make any sedative combination highly lethal |
| When other sedatives are present | Benzodiazepines, sedating antihistamines, and alcohol together multiply respiratory risk |
What Happens When You Mix Methadone and Alcohol: The Overdose Risk
The most serious consequence of mixing methadone and alcohol is overdose. Because methadone outlasts naloxone by many hours, a person who appears to recover after reversal may deteriorate again.
StatPearls naloxone guidance notes that naloxone’s half-life in adults is about 30 to 80 minutes, far shorter than methadone’s.
Patients who respond to naloxone after a methadone overdose should be monitored continuously for 6 to 12 hours for recurrent respiratory depression, and repeat doses every 2 to 5 minutes may be needed.
The National Association of EMS Physicians identifies methadone as a high-risk long-acting opioid for delayed respiratory depression after naloxone reversal.
This means “wait and see” at home is not a safe strategy when methadone and alcohol have been combined.
Emergency Response Steps
If someone on methadone shows overdose signs after drinking alcohol, act immediately:
- Give naloxone if it is available
- Call 911 right away, even if naloxone was given
- Place the person on their side to prevent choking
- Try to keep them awake and breathing
- Stay with them until emergency help arrives
- Do not assume they are safe because they woke up
SAMHSA overdose guidance recommends that clinicians assess whether to prescribe naloxone proactively for patients on methadone, and that patients and caregivers learn to recognize overdose signs before an emergency occurs.
Alcohol Use Among People on Methadone: How Common Is It?
The methadone and alcohol side effects problem is not rare or theoretical. Research consistently shows that alcohol use is common among people receiving methadone treatment.
A study published in the Journal of Addiction Medicine found that about one-third of methadone-maintained patients have some form of problematic alcohol use, based on international literature.
Among 549 clients in methadone clinics in Wuhan, China, 29 percent reported current drinking and about 10 percent met criteria for hazardous drinking.
A Frontiers in Psychiatry study from Iran found that 41.9 percent of opioid agonist treatment patients reported lifetime alcohol use and 7.3 percent reported past-month use, even in a country with a national alcohol ban.
This shows that alcohol use persists even in highly restrictive environments, which means clinicians should screen for it routinely rather than assuming it is absent.
Alcohol use in methadone treatment populations is linked to more than overdose risk. The Journal of Addiction Medicine study found it was also associated with poorer treatment adherence, relapse to illicit drug use, criminal activity, impaired social functioning, and worse physical and mental health outcomes.
Importantly, evidence does not clearly show that methadone itself causes increased alcohol use.
A Vancouver cohort study found no significant association between methadone formulation and heavy drinking, suggesting the co-occurrence reflects pre-existing patterns rather than a medication effect.
Cardiac Risk: Another Reason to Avoid Alcohol on Methadone
Respiratory depression is the main acute danger, but methadone also carries a separate cardiac risk that alcohol can complicate.
A 2025 systematic review and meta-analysis of 22 observational studies found that methadone maintenance treatment was associated with a 34 percent prevalence of QTc prolongation and a 2 percent incidence of torsades de pointes, a potentially fatal heart rhythm.
The same analysis found a dose-dependent relationship, with risk rising notably at daily doses above 100 mg.
Alcohol does not directly cause QTc prolongation in the same way methadone does, but it complicates the clinical picture. Sedation and low blood pressure from combined use can mask arrhythmia symptoms like dizziness or fainting.
Electrolyte disturbances from heavy drinking can also increase arrhythmic vulnerability. And at high methadone doses, where cardiac risk is already elevated, any additional destabilizing factor matters more.
Should Methadone Be Stopped If a Patient Drinks?
This is where the evidence becomes more nuanced, and it is worth being direct about it.
The instinctive response to alcohol use in a methadone patient might be to stop the medication. But the most reliable modern guidance says that is usually the wrong call.
The CDC 2022 opioid prescribing guideline states that methadone or buprenorphine for opioid use disorder should not be withheld from patients taking benzodiazepines or other CNS depressants, because untreated opioid use disorder may carry even greater harms.
FDA labeling says the same: treatment for opioid addiction should not be categorically denied solely because a patient uses alcohol or other depressants.
This matters because the mortality data is clear. Methadone treatment reduces overdose deaths. Removing someone from treatment pushes them toward illicit opioids with unpredictable potency and no clinical support. The weeks immediately after leaving treatment are among the most dangerous of all.
The right response to alcohol use in a methadone patient is not to stop treatment. It is to intensify monitoring, provide overdose education, ensure naloxone access, screen for alcohol use disorder, and address any underlying mental health needs driving the drinking.
Practical Guidance for Patients and Families
If you or someone you care about is on methadone, these points reflect what the strongest evidence supports.
Do not drink alcohol while taking methadone: This is the clear, consistent message from SAMHSA, MedlinePlus, the FDA, and the CDC. There is no safe level of alcohol use established for people on methadone, and even moderate drinking can worsen sedation and breathing risk.
Know the overdose signs: Slow or stopped breathing, inability to wake up, blue lips, pinpoint pupils, and gurgling sounds are all emergencies. Do not wait to see if the person improves on their own.
Keep naloxone on hand: SAMHSA recommends that patients on methadone and their household members have naloxone available and know how to use it. Because methadone outlasts naloxone, always call 911 even after giving a dose.
Be honest with your treatment provider: If you are drinking while on methadone, tell your care team. Hiding it prevents them from helping you manage the risk. FDA and CDC guidance supports keeping patients in treatment rather than excluding them for alcohol use.
If you are struggling with both alcohol and opioids, integrated treatment helps: Addressing both at the same time, with support for any co-occurring mental health conditions, gives you the best chance of staying safe and building a stable recovery.
If you or someone you love is navigating opioid use disorder alongside alcohol use and needs structured, compassionate support, reach out to explore Summit’s addiction treatment options that address both at once. Call us today!
