Stopping 7-hydroxymitragynine (7-OH) after regular use often triggers withdrawal symptoms within 6 to 24 hours.
The syndrome typically resembles opioid withdrawal, with muscle aches, anxiety, sweating, nausea, and insomnia peaking around days 1 to 3, then improving over the next several days.
This article explains what to expect, how long symptoms last, and when professional support becomes essential.
What is 7-Hydroxymitragynine and Why Does Withdrawal Happen?
7-hydroxymitragynine is a potent alkaloid found in kratom that acts as a partial mu-opioid receptor agonist. While traditional kratom leaf contains only trace amounts of 7-OH under natural conditions, the U.S. market increasingly offers concentrated, enriched, or semi-synthetic 7-OH products marketed as kratom but chemically distinct from botanical preparations.
Recent evidence shows that 7-OH has stronger mu-opioid receptor activity and more opioid-like behavioral effects than mitragynine, the main alkaloid in kratom leaf. This stronger receptor activity explains why concentrated 7-OH products can produce rapid tolerance, physical dependence, and withdrawal when use stops. Repeated exposure drives neuroadaptation at the receptor level, and cessation reveals that adaptation as withdrawal.
The distinction between traditional kratom leaf and concentrated 7-OH products matters clinically. A 2024 public health review emphasized that oral dried leaf produces measurable but limited 7-OH exposure, while concentrated commercial products may expose users to far higher opioid-receptor-active doses. That difference shapes withdrawal severity.
Core 7-OH Withdrawal Symptoms
Withdrawal from concentrated 7-OH products typically produces a mixed symptom pattern that includes both opioid-like physical symptoms and psychological distress.
Physical Symptoms
The most common physical symptoms include:
- Muscle aches and body pain
- Sweating and chills
- Nausea and vomiting
- Diarrhea and abdominal cramping
- Runny nose and watery eyes
- Insomnia
- Fatigue and weakness
- Tremors
- Yawning
These symptoms align with classic opioid withdrawal and reflect the body’s adjustment to the absence of mu-opioid receptor stimulation.
Psychological Symptoms
Psychological symptoms are often prominent and may persist longer than physical discomfort:
- Anxiety and restlessness
- Irritability and mood swings
- Depressed mood
- Intense cravings
- Difficulty concentrating
- Emotional sensitivity
A 2025 case report described withdrawal from concentrated 7-OH as producing opioid-like symptoms such as myalgia, insomnia, anxiety, and gastrointestinal distress, plus stimulant-like features including irritability and restlessness.
This mixed profile distinguishes 7-OH withdrawal from purely opioid-driven syndromes.
Severe or Complicated Presentations
While most withdrawal cases remain manageable, severe presentations can occur, especially with high doses, frequent redosing, polysubstance use, or co-occurring psychiatric conditions. Warning signs include:
- Severe dehydration from vomiting or diarrhea
- Marked agitation or psychosis
- Inability to sleep for prolonged periods
- Crisis-level depression or self-harm risk
- Return to illicit opioids
One documented case involved a person using approximately 800 mg daily of concentrated 7-OH who experienced severe agitation, psychosis, respiratory compromise, and required ICU-level care.
While this represents an extreme outcome complicated by polysubstance history and concurrent nicotine withdrawal, it demonstrates that concentrated 7-OH withdrawal can become medically serious.
7-OH Withdrawal Timeline: When Symptoms Start, Peak, and Improve?
The withdrawal timeline varies by product potency, dose, frequency, duration of use, and individual factors, but a consistent pattern emerges across multiple evidence sources.
Early Onset: 6 to 24 Hours
Symptoms often begin within the first day after stopping use. Some heavy users of concentrated products report symptoms starting within 6 to 8 hours, while others notice onset closer to 12 to 24 hours.
This rapid onset reflects the short duration of effect common with concentrated 7-OH products, which may require frequent redosing throughout the day.
Early symptoms typically include anxiety, restlessness, insomnia, mild muscle aches, and cravings.
Peak Acute Withdrawal: Days 1 to 3
The most intense symptoms usually occur during the first 24 to 72 hours. Multiple sources converge on days 1 to 3 as the peak period, when physical discomfort reaches its worst.
During this phase, users commonly experience severe muscle aches, nausea, vomiting, diarrhea, sweating, chills, strong cravings, and marked anxiety.
A 2025 inpatient case documented a Clinical Opiate Withdrawal Scale (COWS) peak of 14, consistent with moderate opioid withdrawal, supporting the clinical framing of 7-OH withdrawal as opioid-like.
Improvement Phase: Days 4 to 7
Physical symptoms often begin easing by the fourth or fifth day. By the end of the first week, most acute physical discomfort has substantially improved, though fatigue, mood disturbance, and sleep problems may remain.
Post-Acute Symptoms: Weeks or Longer
Insomnia, low mood, anxiety, fatigue, and cravings can persist for weeks after the acute phase resolves. These residual symptoms represent the brain’s slower readjustment to normal function and pose the greatest relapse risk. Some heavy users may experience intermittent cravings and mood instability for months.
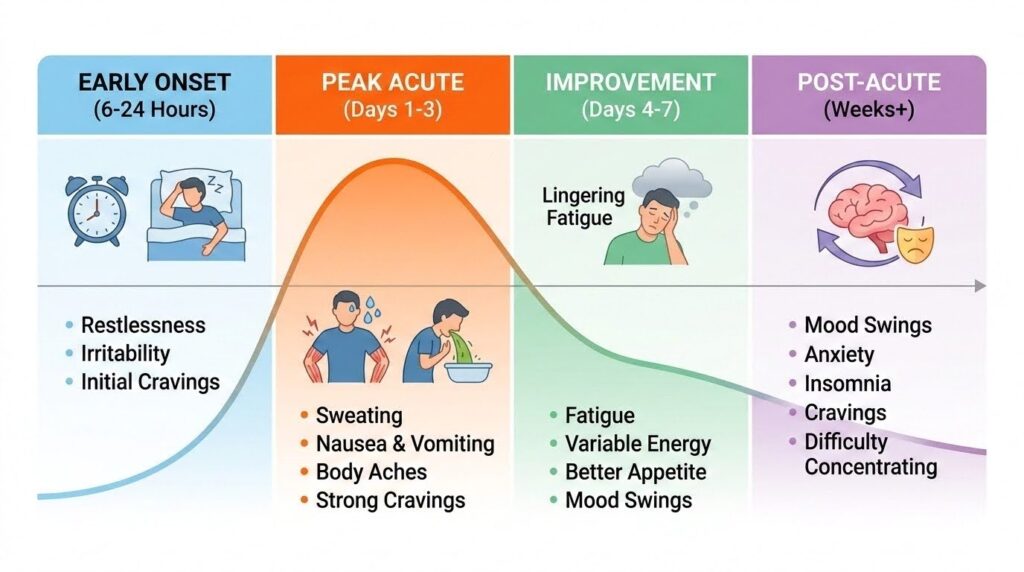
| Phase | Timing | Typical Symptoms |
|---|---|---|
| Early onset | 6–24 hours | Anxiety, restlessness, insomnia, cravings, mild aches |
| Peak acute | Days 1–3 | Severe muscle pain, GI distress, sweating, chills, strong cravings |
| Improvement | Days 4–7 | Physical symptoms ease; fatigue and mood issues continue |
| Post-acute | Weeks to months | Insomnia, low mood, anxiety, cravings |
Why Withdrawal Severity Varies?
Not everyone experiences the same withdrawal intensity. Several factors shape the severity and duration of symptoms.
Product Potency and Formulation
The strongest driver of variation is whether someone used traditional kratom leaf or concentrated 7-OH products. Recent public health literature argues that concentrated 7-OH products display respiratory depression, tolerance, dependence, and withdrawal in preclinical models, aligning them more closely with classical opioids than with botanical kratom.
Daily Dose and Frequency
Higher doses and more frequent use predict greater withdrawal severity. The 800 mg daily case provides a concrete example of very high human exposure linked to severe withdrawal. Frequent redosing throughout the day can also create mini-withdrawal states between doses, reinforcing compulsive use and accelerating dependence.
Duration of Use
Longer exposure allows deeper physiologic adaptation. Chronic use over months or years generally produces more entrenched dependence than short-term experimentation.
Concurrent Substance Use
Polysubstance use complicates withdrawal and increases severity. CDC poison center data show that multiple-substance exposures are associated with higher hospitalization rates, more serious outcomes, and most kratom-associated deaths.
Concurrent use of opioids, benzodiazepines, alcohol, nicotine, or stimulants can create mixed withdrawal syndromes that challenge diagnosis and management.
Individual Metabolism and Health Status
Metabolism, psychiatric vulnerability, and medical comorbidity all influence onset, severity, and duration. People with co-occurring mental health conditions or prior substance use disorders may experience more intense psychological symptoms and higher relapse risk.
Concentrated 7-OH Products vs Traditional Kratom Leaf
One of the most important findings from recent evidence is that concentrated 7-OH products should not be treated as equivalent to traditional kratom leaf. A 2026 CDC analysis explicitly noted that the market has shifted toward high-potency alkaloid extracts, and that 7-OH-enriched products are distinct from traditional leaf preparations.
Traditional kratom leaf generally contains multiple alkaloids with only trace natural 7-OH. Withdrawal after moderate leaf use is often described as mild to moderate and sometimes variable or absent. One controlled observation cited in a 2024 review found an absence of withdrawal symptoms upon discontinuation of daily kratom use in three formulations, suggesting that withdrawal after traditional products may not be inevitable.
By contrast, concentrated 7-OH products appear to generate a more opioid-like profile in both intoxication and withdrawal. The stronger receptor activity, higher potency, and frequent-redosing pattern associated with these products likely explain why withdrawal can feel worse than traditional kratom withdrawal even when users do not think of themselves as taking opioids.
When 7-OH Withdrawal Becomes Dangerous?
While 7-OH withdrawal is often described as uncomfortable rather than life-threatening, that framing can be misleading if interpreted too casually.
The core withdrawal syndrome may often be nonfatal, but severe complications, psychiatric destabilization, dehydration, relapse to stronger opioids, and product unpredictability can create genuine medical danger.
Emergency Warning Signs
Seek urgent or emergency medical care if any of these occur:
- Trouble breathing or blue lips
- Loss of consciousness or severe sedation
- Seizure
- Chest pain
- Severe confusion or psychosis
- Inability to keep fluids down
- Signs of dehydration
- Suicidal thoughts or self-harm risk
Severe illness after 7-OH use can include respiratory depression, altered consciousness, seizures, tachycardia, and hypertension, warranting emergency evaluation. These are not typical simple withdrawal features but red-flag toxicity or complication signs.
When Professional Evaluation is Appropriate?
Professional evaluation is appropriate when there is:
- High-dose concentrated 7-OH use
- Failed prior quit attempts
- Severe vomiting, diarrhea, or dehydration
- Concurrent use of opioids, alcohol, or benzodiazepines
- Co-occurring psychiatric symptoms
- Significant medical comorbidity
- Prior precipitated withdrawal
Treatment and Management Options
There are no FDA-approved medications or established evidence-based guidelines specifically for 7-OH withdrawal. Current management is primarily supportive and symptomatic.
Supportive Care
Common symptomatic approaches include:
- Hydration support, including IV fluids when needed
- NSAIDs for muscle aches
- Antiemetics such as ondansetron for nausea
- Loperamide for diarrhea
- Clonidine for autonomic symptoms such as sweating and agitation
- Hydroxyzine or other adjuncts for anxiety and sleep support
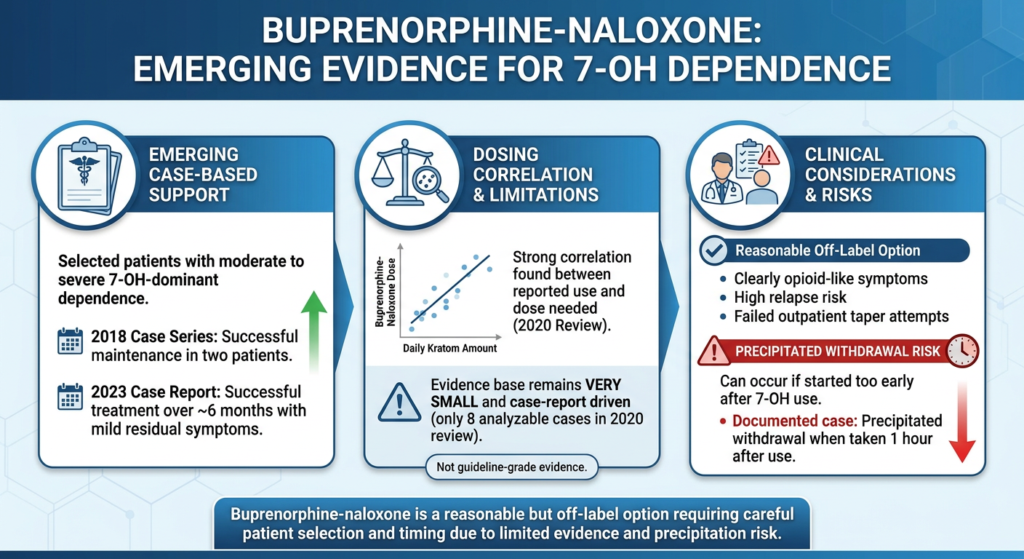
Buprenorphine-Naloxone: Emerging Evidence
Buprenorphine-naloxone has emerging case-based support for selected patients with moderate to severe 7-OH-dominant dependence.
A 2018 case series reported successful buprenorphine-naloxone maintenance in two kratom-dependent patients, and a 2023 case report described successful treatment over approximately six months with only mild residual symptoms.
A 2020 case series and systematic review found a strong correlation between reported daily kratom amount and buprenorphine-naloxone dose needed, suggesting exposure level may help guide initial dosing. However, the evidence base remains very small and case-report driven, with only eight analyzable cases in that review.
Buprenorphine-naloxone is a reasonable off-label option for selected patients with clearly opioid-like symptoms, high relapse risk, or failed outpatient taper attempts.
However, it is not yet a universal default because the evidence base is tiny and not guideline-grade. Additionally, buprenorphine started too early can precipitate withdrawal, just as in other opioid-dependent states. One case documented precipitated withdrawal after buprenorphine-naloxone taken one hour after 7-OH use.
Tapering vs Abrupt Discontinuation
There is limited standardized research guiding taper protocols for concentrated 7-OH products. From a practical standpoint, abrupt stopping is more likely to produce a clear withdrawal spike, while tapering may reduce peak symptom intensity. However, the optimal taper for 7-OH products is not established.
Rising Exposure and Public Health Concern
Poison center surveillance suggests a sharp increase in kratom-related exposures. America’s Poison Centers reported 1,690 kratom exposure cases from January 1 to July 31, 2025, already exceeding all of 2024, with a growing subset involving 7-OH.
The CDC’s 2026 MMWR reported an approximately 1,200 percent increase in kratom-related poison center exposure reports from 258 to 3,434 between 2015 and 2025.
Among reported 7-OH-only exposures, 35 percent had serious health effects and 67 percent were treated at a healthcare facility, suggesting clinically significant acute toxicity. This is one of the clearest signals that concentrated 7-OH products deserve separate clinical treatment from generic kratom.
What You Should Expect?
For most dependent users of concentrated 7-OH products, the acute physical timeline likely resembles short-acting opioid withdrawal over several days, but with substantial variability.
Symptoms may begin the same day or within the first day after stopping, the worst physical symptoms are usually in the first three days, improvement often starts by day four to day seven, and sleep, mood, and cravings can continue for weeks.
For heavier users, especially those repeatedly dosing concentrated tablets or extracts, onset may be rapid, severity may be substantial, and unsupported outpatient quitting may fail or become clinically unsafe.
The field does not yet have enough data to make highly precise universal duration claims, but it already has enough evidence to justify a higher-risk clinical posture.
Help and Support Resources
For people in the United States seeking help with substance use or withdrawal-related care:
- SAMHSA National Helpline: 1-800-662-HELP (4357), free, confidential, 24/7, English and Spanish
- HELP4U text locator: text ZIP code to 435748
- FindTreatment.gov and related resources are listed via SAMHSA’s Find Help page
- If there is immediate crisis, suicidal thinking, or severe mental distress, call or text 988
If you or someone you care about is struggling with 7-OH dependence or withdrawal, our professional support can make a meaningful difference.
Consider reaching out to The Summit Wellness Group’s addiction treatment programs that offer evidence-based care, medical supervision, and individualized support designed to help you safely navigate withdrawal and build a foundation for lasting recovery.
