GHB and Alcohol Interaction: Can You Mix Alcohol & GHB?
Mixing GHB and alcohol is one of the most dangerous drug combinations a person can make. Even modest amounts of alcohol can turn a recreational GHB dose into a medical emergency, because both substances suppress the central nervous system at the same time.
A controlled human study found that combining the two produced six times more vomiting episodes than either drug alone, along with greater drops in blood pressure and oxygen levels.
This article explains exactly what happens when you mix alcohol and GHB, why the danger is greater than most people expect, and what the science says about the symptoms and overdose risks you need to know.
GHB and Alcohol: Why the Combination is So Dangerous?
GHB, or gamma-hydroxybutyrate, is a short-acting central nervous system depressant. At low doses it can produce euphoria, relaxation, and disinhibition. At higher doses it can cause confusion, vomiting, respiratory depression, and abrupt coma.
The gap between those two states is narrow, and that narrow margin is what makes GHB uniquely risky even before alcohol enters the picture.
Alcohol is also a CNS depressant. It slows breathing, lowers blood pressure, impairs coordination, and reduces the reflexes that protect your airway if you vomit.
When you combine two substances that do the same harmful things to your body, the effects do not simply add up neatly. They can amplify each other in ways that are hard to predict and fast to escalate.
Alcohol is the most common substance co-ingested with GHB in acute poisoning cases. That is not a coincidence. GHB is often used in nightlife, party, and sexual settings where alcohol is already present.
People may drink before taking GHB, underestimate how much they have consumed, or re-dose because the effects seem delayed. Each of those behaviors raises the risk of a serious or fatal outcome.
The Narrow Margin Between Pleasure and Poisoning
One of the most important things to understand about GHB is its steep dose-response curve. A small increase in dose can push someone from feeling relaxed to being completely unresponsive. Illicit GHB preparations vary widely in concentration, so a person may not know how much they are actually taking.
Alcohol makes this problem worse in two ways: it directly worsens the toxic effects of GHB, and it impairs the judgment needed to dose carefully or recognize early warning signs.
GHB and Alcohol Interactions: What the Science Shows?
The clearest direct evidence comes from a double-blind, crossover study in 16 healthy adults who received GHB alone, alcohol alone, both together, or a placebo. The human interaction study found that combining the two drugs produced more vomiting, more hypotension, and greater drops in oxygen saturation than either substance alone.
Six of eight vomiting episodes across all sessions occurred during the combined condition. Two episodes of brief but significant hypotension, with systolic blood pressure dropping to 71 to 73 mm Hg, occurred only in the combined group.
The researchers also measured GHB blood levels and found that alcohol did not dramatically increase how much GHB stayed in the body. Peak GHB concentration rose by about 16 percent and half-life extended by about 29 percent, but neither change reached statistical significance.
That finding carries an important practical message: the danger of mixing GHB and alcohol is not mainly that alcohol makes GHB levels skyrocket. The danger is that alcohol makes GHB’s depressant effects on the brain and body substantially worse, even when blood levels look relatively normal.
A 2023 toxicology review reached the same conclusion, finding that GHB-ethanol co-administration enhances sedation and cardiovascular dysfunction through additive action on inhibitory brain systems, while pharmacokinetic changes remain minimal.
The mechanism is best understood as two depressants loading the same inhibitory pathways at the same time.
What Real Emergency Data Show?
Controlled studies use modest doses in healthy volunteers. Real-world emergency data tell a different story about what happens when people mix GHB and alcohol in actual recreational settings.
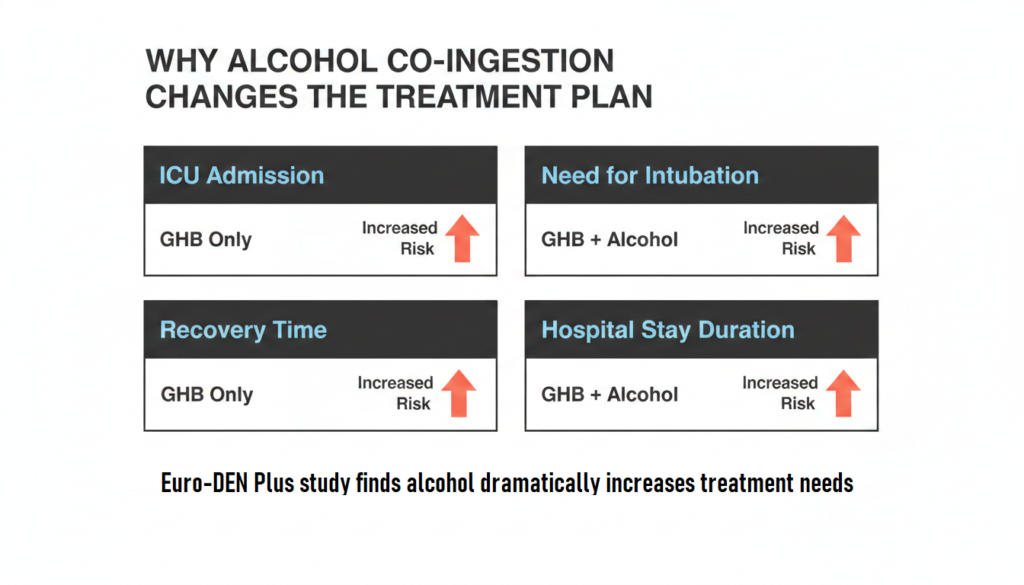
A multicenter analysis of emergency department presentations involving GHB and GBL intoxication found that patients who had also consumed alcohol showed greater depression of consciousness, greater need for treatment, more ICU admissions, and longer hospital stays than those who had taken GHB or GBL alone.
A broader Euro-DEN Plus study of 43,633 emergency presentations involving CNS depressant drugs found that ethanol co-ingestion increased adverse effects and treatment needs across the group, with GHB and GBL cases showing a particularly strong impact.
A Swiss emergency department series found that coma occurred in 77 percent of GHB patients who had also used alcohol, compared with 62 percent of those who had not, and that alcohol co-users tended to have longer recovery times.
These differences did not always reach statistical significance, likely because of sample size, but the clinical pattern was consistent enough for the authors to consider it relevant.
GHB and Alcohol Symptoms: What Happens to Your Body?
Understanding the specific symptoms that emerge when you mix GHB and alcohol helps explain why this combination can be fatal even when neither substance alone would have caused the same outcome.
Symptoms at Lower Combined Doses
At lower doses, a person mixing GHB and alcohol may initially feel:
- Intense euphoria and disinhibition
- Warmth, relaxation, and increased sociability
- Reduced coordination and slurred speech
- Nausea, which can escalate quickly
- Confusion and difficulty tracking conversations
These effects can feel manageable at first, which is part of what makes the combination so deceptive. The transition from this state to a dangerous one can happen within minutes.
Symptoms as Toxicity Develops
As the combined depressant load increases, the following symptoms become more likely and more severe than with GHB alone:
- Deepening sedation that becomes impossible to fight
- Vomiting while consciousness is reduced, creating a serious aspiration risk
- Significant drops in blood pressure
- Slowed or shallow breathing
- Falling oxygen levels
- Loss of the gag reflex that normally protects the airway
- Abrupt loss of consciousness or coma
The vomiting and sedation combination is especially dangerous. A person who vomits while deeply sedated cannot protect their airway. Aspiration of stomach contents into the lungs can cause pneumonitis, respiratory failure, and death.
The controlled human study showed that vomiting was dramatically more common with the combined condition, and the authors specifically identified aspiration as one of the most important immediate threats.
The Abrupt Awakening Problem
GHB intoxication has a distinctive feature that complicates management: people can move from deep unresponsiveness to sudden agitation in a short period.
This abrupt awakening can occur even after severe poisoning and can make airway management more difficult. Alcohol does not eliminate this pattern but can make the preceding period of unconsciousness deeper and more dangerous.
Mixing GHB and Alcohol: Overdose Risks
The word “overdose” in the context of GHB does not always mean an extreme or unusual amount. Because GHB’s dose-response curve is so steep, and because illicit preparations vary in concentration, what feels like a normal recreational dose can cross into toxic territory quickly. Alcohol lowers that threshold further.
The following table summarizes the key overdose risks linked to mixing GHB and alcohol, based on the strongest available evidence.
| Risk | Mechanism | Evidence strength |
|---|---|---|
| Respiratory depression | Additive CNS suppression of breathing drive | Strong |
| Oxygen desaturation | Worsened by combined sedation | Strong |
| Aspiration after vomiting | More vomiting plus reduced airway reflexes | Strong |
| Hypotension | Additive cardiovascular depression | Strong |
| Deep or prolonged coma | Greater consciousness depression | Strong |
| ICU admission | More severe overall toxicity | Strong |
| Death | Respiratory or cardiovascular failure, aspiration | Strong contextual evidence |
There is no antidote for GHB poisoning. Treatment is supportive, focused on protecting the airway, maintaining breathing and circulation, and monitoring until the person recovers.
Naloxone does not reverse GHB’s effects. If opioid co-ingestion is also possible, naloxone may still be given, but it will not address the GHB component.
Why Alcohol Makes Dosing Errors More Likely?
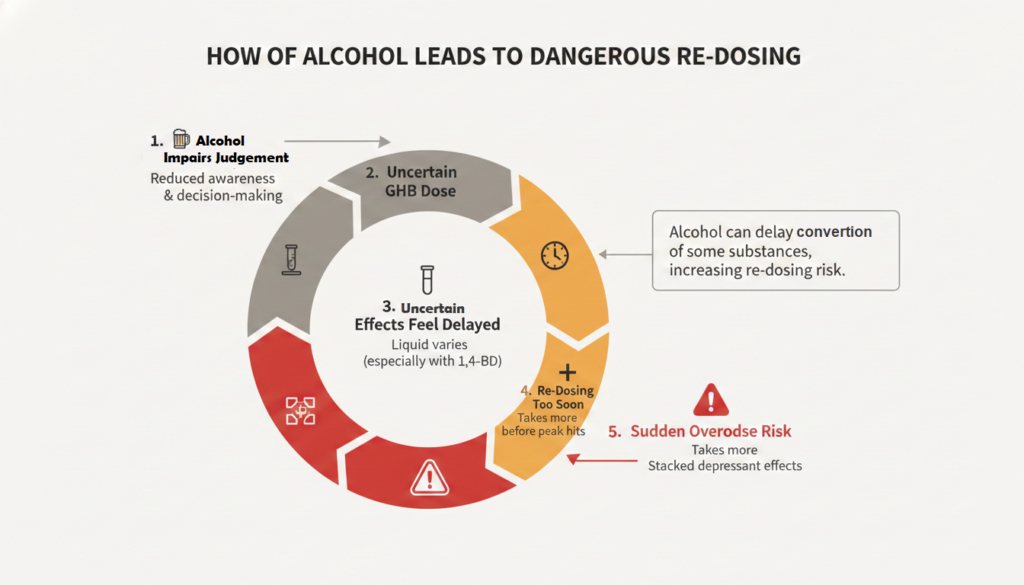
Alcohol impairs judgment and self-monitoring. A person who is already drinking may misjudge how much GHB they have taken, re-dose too soon because effects seem delayed, or fail to notice that a friend is becoming dangerously sedated. GHB sold illicitly often comes as a liquid with no reliable concentration labeling.
Some substances sold as GHB are actually GBL or 1,4-butanediol, which convert to GHB in the body but can have different onset profiles.
Australian surveillance data warn that 1,4-BD combined with alcohol may create delayed toxicity, because alcohol can temporarily slow the conversion of 1,4-BD to GHB, leading people to think the dose is weak and re-dose, only to experience a dangerous CNS depressant effect later.
Vulnerability to Assault and Injury
GHB is amnestic. Alcohol independently worsens memory and incapacitation. Together, they can produce a state of profound vulnerability. A person may be unable to resist assault, unable to recall events afterward, and unable to seek help in time.
California poison control data found that among cases involving suspected malicious intent, 43 percent involved ethanol co-ingestion and 19 percent reported sexual assault. Memory impairment was far more common in those cases than in accidental exposures.
GHB Side Effects With Alcohol: The Longer Picture
The risks of mixing GHB and alcohol do not end with a single episode. People who use GHB regularly can develop dependence quickly, sometimes within weeks of daily use. Dependent users may dose every one to three hours to avoid withdrawal.
GHB withdrawal resembles alcohol withdrawal but can begin more rapidly because of GHB’s short half-life. Symptoms include tremor, anxiety, agitation, sweating, hallucinations, delirium, and seizures.
When a person is dependent on both GHB and alcohol, withdrawal becomes more complex and more dangerous. SA Health clinical guidance specifically identifies co-dependence on alcohol or benzodiazepines as a factor that increases withdrawal risk and changes management decisions.
Treatment typically involves benzodiazepines, sometimes baclofen or phenobarbital in resistant cases, and close inpatient monitoring for high-risk patients.
This means the GHB and alcohol combination creates a two-stage medical problem: acute poisoning risk during use, and complicated, potentially severe withdrawal if dependence develops.
What to Do in an Emergency?
If someone who has mixed GHB and alcohol becomes hard to wake, is breathing slowly or shallowly, vomits while drowsy, or collapses, this is a medical emergency. Call emergency services immediately. While waiting:
- Place the person in the recovery position on their side to reduce aspiration risk
- Do not leave them alone
- Do not assume they are “just drunk” or “just sleeping it off”
- Tell emergency responders about all substances taken, including alcohol and GHB
Do not wait to see if the person improves on their own. GHB toxicity can worsen rapidly, and the window for effective intervention can be short.
The Bottom Line on GHB and Alcohol
The evidence from controlled human studies, multicenter emergency registries, toxicology reviews, and clinical guidance all point to the same conclusion.
Alcohol does not simply make GHB “a bit stronger.” It materially transforms the risk profile of GHB use by deepening sedation, worsening respiratory depression, increasing vomiting and aspiration risk, lowering blood pressure, and raising the likelihood that a person will need emergency medical care or ICU-level monitoring.
The interaction is primarily pharmacodynamic, meaning alcohol amplifies what GHB does to the brain and body rather than simply raising GHB blood levels.
That distinction matters because it means even “normal” GHB concentrations can be associated with severe poisoning when alcohol is present. Clinicians, bystanders, and users themselves should not be reassured by the idea that “the levels weren’t that high.”
If you or someone you care about is struggling with GHB use, alcohol use, or both, reaching out for our professional support is the most important step you can take. Summit Wellness Group’s GHB treatment is here to help you find a path forward.
