Mixing tramadol and alcohol is not safe, and the danger is not subtle. FDA-approved tramadol labeling states directly that combining these two substances can cause profound sedation, respiratory depression, coma, and death.
This article explains exactly what happens when you mix tramadol and alcohol, why the risks go beyond simple drowsiness, and what to do if someone may have already combined them.
Tramadol and Alcohol: Why the Combination is Dangerous?
Tramadol is a prescription opioid used for moderate to severe pain. Alcohol is a central nervous system depressant that most people encounter in everyday social settings. When both are present in the body at the same time, each one amplifies the other’s most dangerous effects.
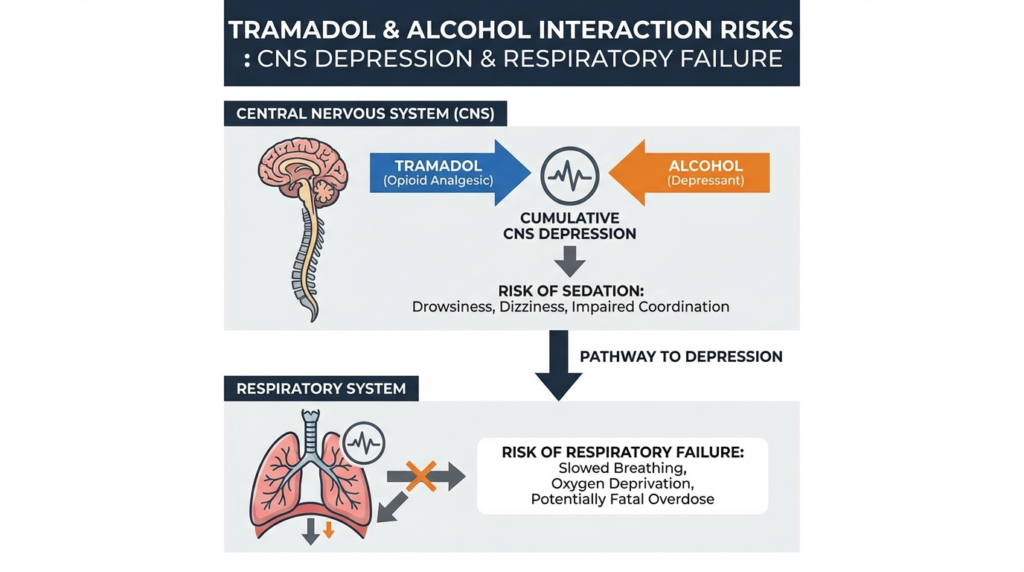
The core problem is additive CNS depression. Both substances slow brain activity, reduce alertness, and suppress the signals that tell your lungs to keep breathing. Together, they can push that suppression past a safe threshold far more quickly than either substance would alone.
This is not a theoretical concern. DailyMed prescribing information states that case reports show fatal overdose risk is further increased when tramadol is abused concurrently with alcohol or other CNS depressants.
That language is precise and deliberate. Alcohol is not a minor co-factor here. It is a recognized contributor to fatal tramadol overdose.
How Tramadol Works?
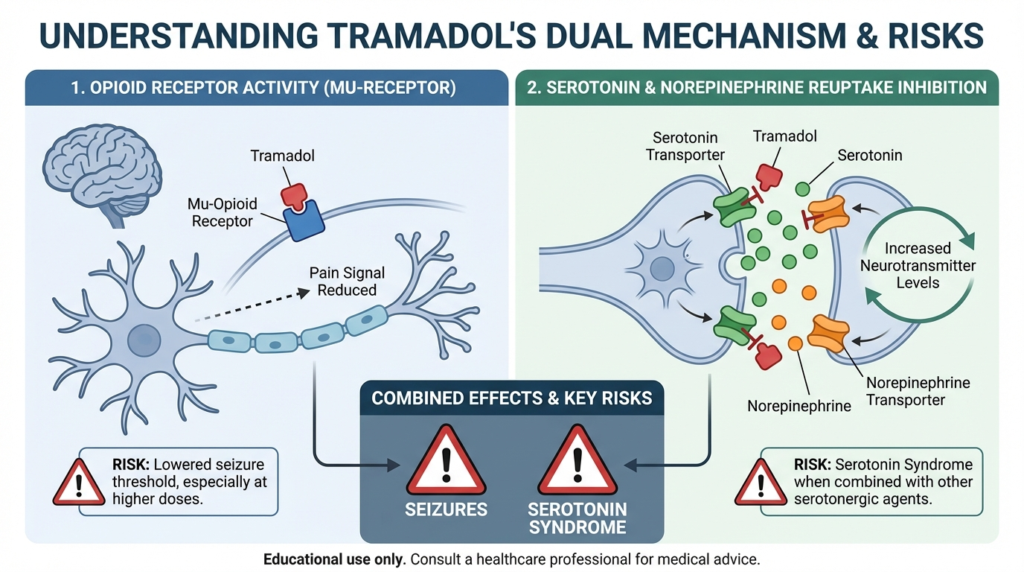
Tramadol is not a straightforward opioid. It acts on mu-opioid receptors, which explains its pain-relieving effects and its ability to cause respiratory depression and sedation. But it also inhibits the reuptake of serotonin and norepinephrine. That dual mechanism is why tramadol’s danger profile is broader than many patients expect.
The opioid side drives sedation and breathing suppression. The monoaminergic side creates a real risk of seizures and, in some circumstances, serotonin toxicity.
Add alcohol to that picture and you are not just dealing with one depressant on top of another. You are dealing with a drug that already carries seizure risk, serotonin-related complications, and respiratory depression risk, all made worse by a second CNS depressant.
StatPearls clinical reference confirms that tramadol’s metabolism runs through CYP2D6 and CYP3A4 pathways, meaning genetic differences, liver function, and interacting drugs can all change how much tramadol is actually circulating in the body at any given time. That variability makes casual self-assessment of safety unreliable.
How Alcohol Makes Things Worse?
Alcohol depresses the same brain systems that tramadol targets. It reduces ventilatory drive, impairs coordination, weakens protective airway reflexes, and clouds judgment.
In practical terms, that last point matters enormously. A person who has been drinking may forget they already took tramadol and take another dose.
They may combine tramadol with a sleep aid or muscle relaxant without thinking twice. They may feel “just tired” when they are actually entering a dangerous level of respiratory depression.
The NIAAA resource on alcohol-medication interactions makes clear that alcohol’s CNS depressant properties are well established and that combining it with other depressants is a recognized source of serious harm.
Can You Overdose on Tramadol and Alcohol Together?
Yes! The answer here is not ambiguous.
FDA labeling states that tramadol taken with alcohol can cause severe drowsiness, decreased awareness, breathing problems, coma, and death.
The older extended-release label goes further, noting that tramadol in excessive doses, either alone or in combination with other CNS depressants including alcohol, is a major cause of drug-related deaths and that fatalities within the first hour of overdose are not uncommon.
An overdose does not always mean someone swallowed a dramatically large amount. It means the total drug effect exceeded what the body could safely handle. Alcohol can convert what might have been a nonfatal tramadol exposure into a fatal one by narrowing the margin of safety.
What Overdose Can Look Like?
Recognizing the signs early can save a life. Across official labeling, clinical references, and toxicology literature, the warning signs of a tramadol and alcohol overdose include:
- Extreme drowsiness or inability to stay awake
- Slow, shallow, or irregular breathing
- Confusion or disorientation
- Cold, clammy, or pale skin
- Blue or gray lips or fingernails
- Pinpoint pupils
- Vomiting with reduced consciousness
- Atypical snoring or gurgling sounds
- Seizures
- Unresponsiveness or collapse
If any of these appear after someone has mixed tramadol and alcohol, call 911 immediately. Do not assume the person is sleeping it off.
Opioid respiratory depression can worsen gradually, and a person who looks merely intoxicated may be entering a fatal overdose.
Tramadol and Alcohol Interaction Risks Beyond Respiratory Depression
Most people understand that opioids and alcohol both slow breathing. What many do not realize is that tramadol brings additional risks that make the alcohol and tramadol interaction more complex and more dangerous than a standard opioid-alcohol warning suggests.
Seizure Risk
Tramadol lowers the seizure threshold. FDA labeling warns that seizures can occur even at recommended doses and that risk increases with several interacting conditions, including alcohol and drug withdrawal, head trauma, metabolic disorders, and co-use of drugs that also lower seizure threshold.
The toxicology literature supports this concern. A study published in Epidemiology and Health examining 359 severe tramadol overdose cases found seizures in 14.5% of patients and respiratory depression in 18.5%, with three deaths.
A separate cohort of 909 acute tramadol poisoning cases reported seizures in 60% of patients. These numbers vary across populations and settings, but they consistently show that tramadol overdose carries a real seizure burden.
A seizure during intoxication is especially dangerous because it can cause trauma, aspiration, abrupt loss of airway protection, and recurrent hypoxia. For someone already sedated by alcohol, the ability to protect themselves or call for help is severely reduced.
Serotonin-Related Complications
Tramadol’s serotonin reuptake inhibition means that in certain circumstances, particularly at high doses or when combined with antidepressants such as SSRIs, SNRIs, or MAOIs, it can trigger serotonin syndrome.
A PMC case report documents serotonin syndrome occurring with tramadol combined with selective serotonin reuptake inhibitors.
Alcohol is not the classic trigger for serotonin syndrome, but it complicates the picture by masking early mental status changes and increasing the chance of co-ingestions.
If someone is also taking an antidepressant and then mixes tramadol with alcohol, the risk profile shifts significantly.
Cognitive and Motor Impairment
Even when the combination does not produce a life-threatening event, it can still cause serious harm. Both substances impair reaction time, balance, coordination, and judgment. Together, they raise the risk of falls, vehicle crashes, burns, and other accidents.
A person may feel only mildly impaired while their actual ability to drive or operate machinery is severely compromised.
Who Faces the Highest Risk?
Risk is not uniform. Some people face a much steeper danger when mixing tramadol and alcohol.
Older adults clear both substances more slowly because of age-related changes in liver and kidney function. That means sedation and respiratory depression can be deeper and last longer.
People with respiratory conditions such as COPD, asthma, or sleep apnea have less breathing reserve to begin with, so any additional suppression is more likely to become critical.
Those with a history of seizures face elevated risk because tramadol already lowers the seizure threshold. People with liver or kidney impairment may have higher tramadol blood levels than expected from the dose alone.
Patients taking benzodiazepines, sleeping pills, gabapentinoids, muscle relaxants, or other opioids face compounded danger.
FDA prescribing information explicitly warns that potentially fatal additive effects may occur when tramadol is combined with benzodiazepines or other CNS depressants, including alcohol. Adding alcohol to that mix can push the combination into fatal territory.
People with depression, substance use disorder, or a history of misuse are also at elevated risk because impaired judgment and impulsive behavior increase the chance of accidental overdose or intentional self-harm.
The “Just One Drink” Question
Many people ask whether a small amount of alcohol is really that dangerous with tramadol. The honest answer is that no reliably safe threshold can be defined across patients.
Risk depends on the tramadol dose, whether the product is immediate-release or extended-release, the timing of the last dose, individual metabolism, liver and kidney function, age, body size, other medications, and how much alcohol is consumed and how quickly.
Extended-release tramadol maintains drug levels over a longer window, so a patient may incorrectly believe the medication has worn off when significant pharmacologic effect remains.
The only recommendation supported by the strongest available evidence is to avoid alcohol entirely while taking tramadol. There is no comparably strong source in the medical literature that argues casual co-use is generally acceptable.
Long-Term Risks of Combining Tramadol and Alcohol
Repeated mixing introduces a different set of harms beyond acute overdose.
Over time, tolerance can develop, meaning more of one or both substances is needed to achieve the same effect. That promotes dose escalation and increases overdose risk.
Tramadol prescribing information notes that risks of addiction and misuse are increased in patients with personal or family histories of substance abuse, including alcohol abuse, or mental illness such as major depression.
Chronic combined use can also strain the liver and kidneys, worsen mood and cognitive function, and increase the likelihood of a relapse-related overdose.
When tolerance decreases after a period of abstinence, returning to a previously tolerated amount of tramadol or alcohol can overwhelm the body, especially if both are resumed together.
A 2025 systematic review of tramadol’s psychological side effects found associations with manic episodes, psychosis, cognitive impairment, and serotonin syndrome, with risk factors including psychiatric history, polydrug use, and prolonged use.
Alcohol use often occurs in exactly these vulnerable populations, which means the long-term mental health picture can deteriorate significantly with continued combined use.
Naloxone: Helpful but Not a Complete Answer
Naloxone can reverse opioid-mediated respiratory depression and should be given if tramadol overdose is suspected. FDA labeling and MedlinePlus both encourage patients and caregivers to have naloxone available and to know how to use it.
However, naloxone does not fully reverse all tramadol toxicity. Because tramadol’s mechanism goes beyond opioid receptor activity, naloxone may not address seizures or serotonin-related effects.
FDA labeling also notes that seizure risk may increase with naloxone administration in tramadol overdose, though clinical evidence on this point is mixed.
The practical implication is clear: give naloxone if it is available and opioid-type respiratory depression is present, but do not assume the person is safe afterward. Emergency medical care is still required. Call 911 first.
What to Do in an Emergency?
If someone has mixed tramadol and alcohol and shows any warning signs of overdose, act immediately.
1. Call 911. Do not wait to see if symptoms improve.
2. Give naloxone if available and opioid overdose is suspected.
3. Begin rescue breathing or CPR if the person has stopped breathing or breathing is very weak.
4. Place the person in the recovery position if breathing resumes but they remain impaired.
5. Call Poison Control at 1-800-222-1222 for expert guidance if the situation is not yet clearly life-threatening.
6. Tell emergency responders exactly what was taken, how much, and when.
Do not leave the person alone. Do not assume that heavy snoring or deep sleep means they are safe. Opioid respiratory depression can worsen silently, and vomiting during reduced consciousness creates a serious aspiration risk.
Why is Tramadol Often Misjudged?
Tramadol’s reputation as a “weaker” opioid creates a false sense of security. Patients sometimes assume that because it is Schedule IV rather than Schedule II, it carries less danger. That assumption is not supported by the evidence.
FDA labeling places tramadol within the same framework of life-threatening respiratory depression warnings, overdose reversal access, and additive CNS depressant risk as other opioid analgesics.
The seizure and serotonin-related risks add layers of danger that are not present with many other opioids. And alcohol does not introduce a novel risk so much as it magnifies tramadol’s existing ones, especially respiratory depression and impaired consciousness, while simultaneously reducing the person’s ability to recognize that something is wrong.
Nearly 12 million people in the United States received a tramadol prescription in 2022. Alcohol is one of the most widely consumed substances in the country. The overlap between these two populations is large, and the consequences of that overlap can be fatal.
The Bottom Line on Tramadol and Alcohol Interaction Risks
The evidence across regulatory labeling, clinical references, and toxicology literature points in one direction. Tramadol and alcohol should not be mixed.
The combination materially increases the risk of respiratory depression, profound sedation, overdose, seizures, and death. There is no dependable general safety margin that applies across patients, doses, formulations, and individual health profiles.
If you are taking tramadol and want to drink alcohol, speak with your prescriber before doing so. If you or someone you know is struggling with combined use of tramadol and alcohol, that pattern carries real risks of dependence, escalating harm, and overdose, and it deserves professional attention.
If you are ready to take the next step toward recovery, the team at The Summit Wellness Group offers evidence-based addiction treatment programs designed to meet you where you are.
