Combining Vyvanse and marijuana is more common than many people realize, especially among adults with ADHD who use cannabis to manage stimulant side effects like insomnia or anxiety.
Research shows the two substances create overlapping risks rather than a helpful balance, with daily cannabis use in ADHD populations linked to more than twice the odds of cannabis use disorder compared to non-daily users.
This article walks through what the evidence actually says about mixing Vyvanse and weed, why the combination is often counterproductive, and what to do if you are already using both.
Vyvanse and Marijuana: What the Research Shows?
Vyvanse (lisdexamfetamine) is a central nervous system stimulant approved for ADHD and binge eating disorder. It works by increasing dopamine and norepinephrine in the brain, which improves focus, impulse control, and executive function.
According to MedlinePlus drug information, common side effects include decreased appetite, insomnia, anxiety, dry mouth, dizziness, and increased heart rate.
Cannabis, particularly THC-dominant products, affects many of the same systems. THC can raise heart rate, impair short-term memory and attention, worsen anxiety in some users, and increase appetite.
CBD does not reliably cancel out these effects. A randomized laboratory study found that oral CBD pretreatment did not significantly change the subjective, reinforcing, or cardiovascular effects of smoked cannabis, which matters because many people assume CBD-heavy products are automatically safer when combined with stimulants.
Direct controlled trials on Vyvanse plus cannabis are scarce. However, the absence of dedicated interaction studies does not mean the combination is safe. The stronger evidence comes from what each drug does independently, and those profiles overlap in several clinically important ways.
How Vyvanse and Marijuana Interact in the Body?
The most important interaction is functional rather than metabolic. Cannabis does not appear to change how lisdexamfetamine is processed in the body in a clearly established way.
Lisdexamfetamine is a prodrug converted primarily through enzymatic hydrolysis in red blood cells, not through the liver pathways that many drug interactions involve. What cannabis does instead is work against what Vyvanse is trying to do.
Vyvanse is prescribed to sharpen attention, reduce impulsivity, and support organized thinking. THC commonly impairs exactly those functions.
A systematic review of lisdexamfetamine safety found the drug produced reliable gains in attention and impulse control across trials. Adding a substance that impairs short-term memory, slows processing speed, and reduces motivation works against those gains directly.
The second major interaction is cardiovascular. Vyvanse raises heart rate by about 3 to 6 beats per minute on average, with some patients experiencing larger increases. Active cannabis also raises heart rate.
A short-term cardiovascular trial of lisdexamfetamine found these effects were generally modest in healthy adults without preexisting cardiac conditions, but that finding does not apply to people with hypertension, arrhythmia risk, or structural heart disease.
Adding cannabis to an already elevated sympathetic state increases the cardiovascular burden further.
The third interaction involves anxiety. Both substances can worsen it. Vyvanse causes anxiety or irritability in a meaningful share of patients. THC can produce anxiety, paranoia, or panic-like effects, especially at higher doses or in people who are already prone to these symptoms.
A review of THC, CBD, and anxiety found that cannabinoid effects on anxiety are dose-sensitive and heterogeneous, meaning the same person may feel calmer at one dose and significantly more anxious at another.
What Happens When You Mix Vyvanse and Weed?
Here is a plain summary of what the evidence supports when you combine Vyvanse and weed:
- Attention and focus often get worse, not better, because THC impairs the cognitive functions Vyvanse is meant to support
- Heart rate may increase more than with either substance alone, raising cardiovascular strain
- Anxiety, irritability, and mood instability can worsen, especially with regular or high-dose THC use
- Sleep quality tends to suffer even when cannabis seems to help with falling asleep initially
- Appetite effects conflict directly, with Vyvanse suppressing appetite and THC stimulating it
- The risk of developing cannabis use disorder rises with frequent use, particularly in people with ADHD
That last point comes from a 2025 community-based study of adults with ADHD. Among those who used cannabis daily, 62% met criteria associated with cannabis use disorder, compared to 38% of non-daily users, an odds ratio of 2.67.
Daily users also reported worse general health, with 24% rating their health as fair or poor versus 11% of non-daily users.
Why People Use Weed While Taking Vyvanse?
Understanding why people combine these substances matters as much as knowing the risks. The most common reasons are practical and understandable.
Vyvanse can make it hard to sleep, especially if taken too late or at too high a dose. Cannabis feels like a natural fix. Vyvanse suppresses appetite, sometimes severely, and cannabis is known to stimulate it.
Vyvanse can leave some people feeling tense, overstimulated, or emotionally raw as it wears off, and cannabis seems to smooth that out.
The 2025 ADHD cannabis study found that 42% of participants who had ever used cannabis reported doing so specifically to manage ADHD symptoms. That is not a small or unusual group. It reflects a real gap between what prescribed treatment delivers and what patients feel they need.
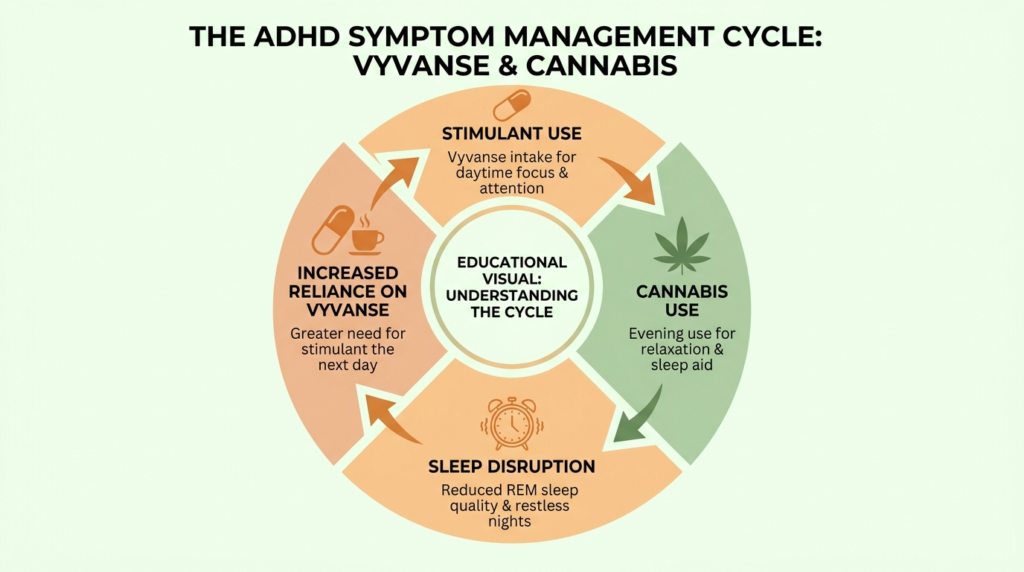
The problem is that this pattern, using one psychoactive substance to offset the side effects of another, tends to become self-reinforcing.
Stimulant by day, cannabis by night, poorer sleep, more cognitive fog the next morning, greater reliance on Vyvanse to function, and then cannabis again to come down.
Lower-quality sleep worsens ADHD symptoms on its own, which can make the stimulant feel less effective, which can prompt dose increases, which worsen the original side effects. The cycle is clinically recognizable and well described in treatment settings.
If you need cannabis regularly to tolerate Vyvanse, that is a signal to reassess the medication plan, not a sign that the combination is working.
Risks by Patient Type
Not everyone faces the same level of risk. The combination is especially concerning in certain groups.
People with cardiovascular disease or symptoms face the clearest danger. FDA prescribing information for lisdexamfetamine warns that stimulants raise blood pressure and heart rate and require monitoring. Adding cannabis adds more cardiovascular uncertainty on top of an already flagged risk.
People with anxiety disorders, bipolar disorder, or a history of psychosis face a particularly unfavorable psychiatric risk balance. Both substances can worsen these conditions independently. Together, the risk of destabilization is higher, not lower.
People using Vyvanse for binge eating disorder face a direct treatment conflict. THC stimulates appetite and can trigger food cravings, which works against the core therapeutic goal of lisdexamfetamine in that context.
Daily cannabis users with ADHD face the highest substance-use risk. The data are clear that frequency matters enormously. Daily use in this population is associated with substantially higher rates of anxiety, depression, bipolar disorder, and PTSD compared to non-daily users, according to the 2025 ADHD cannabis study.
Adolescents and young adults are also a high-concern group. Cannabis can impair cognition during active brain development, and ADHD itself already raises the risk of substance use disorders. A 2024 VA systematic review on ADHD and substance use disorders in adults confirmed that ADHD and substance use commonly co-occur and that treatment decisions in this population require careful, individualized monitoring.
Does THC Content Change the Risk?
Yes, significantly. Most of the risk described above is driven by THC, not CBD. High-THC flower, concentrates, vape oils, and potent edibles carry the most concern.
Lower-THC or CBD-predominant products carry less psychoactive burden, but they are not automatically safe when combined with a stimulant.
Government cannabis guidance from Utah’s medical cannabis program recommends starting at 1 to 2.5 mg THC-equivalent at bedtime and increasing slowly, with many patients staying well below 20 mg per day.
That guidance is not specific to Vyvanse, but it directly addresses a common real-world problem: people often combine stimulants with unmeasured, high-potency cannabis products, which removes any possibility of sensible risk management.
If cannabis is used at all while taking Vyvanse, lower THC content, measured dosing, and infrequent use are meaningfully safer than high-THC products used daily.
Harm Reduction if You Are Already Combining Them
If you are already using cannabis while taking Vyvanse, a few evidence-supported steps can reduce risk.
Tell your prescriber. MedlinePlus specifically advises discussing all substances with your clinician when taking lisdexamfetamine. A prescriber who does not know about cannabis use cannot help you manage the interaction or adjust your treatment plan.
Avoid high-THC products. The cardiovascular, anxiety, cognitive, and psychosis-related risks are primarily driven by THC. Lower-THC or CBD-predominant options carry less risk, though not zero.
Use the lowest possible dose. Starting low and going slow is the standard recommendation in government cannabis guidance, and it applies even more when a stimulant is already in the picture.
Avoid daily use if possible. The data on daily cannabis use in ADHD populations are clear: frequency is one of the strongest predictors of worse outcomes.
Do not drive or operate machinery when impaired. Both substances can affect alertness and judgment. Cannabis adds clear impairment risk on top of any stimulant effects.
Seek urgent care if you experience chest pain, fainting, shortness of breath, or a markedly irregular heartbeat. These are the cardiovascular warning signs flagged in official lisdexamfetamine labeling.
When the Real Answer is a Better Treatment Plan?
The most honest conclusion from the evidence is this: if you need cannabis to tolerate Vyvanse, the medication plan probably needs adjustment, not a cannabis supplement.
Possible issues worth discussing with a clinician include a dose that is too high, a dose taken too late in the day, unaddressed anxiety or sleep disorder, a stimulant formulation that does not suit you, or an emerging cannabis dependence pattern.
A clinician’s guide on ADHD and substance use notes that non-stimulant options like atomoxetine or alpha-2 agonists may be preferable when cannabis use is frequent or when anxiety and misuse risk are significant concerns.
Treating ADHD well and addressing cannabis use are not mutually exclusive goals. But they are best handled together, with a clinician who knows the full picture, rather than through unsupervised self-management.
If you are concerned about how cannabis and Vyvanse are affecting your health or your ADHD treatment, speaking with our specialist in dual diagnosis treatment can help you find a plan that actually works. So reach out to The Summit Wellness Group and start your recovery today!
