The 5 stages of addiction describe how substance use escalates from a first experience to a chronic, compulsive disorder.
Research shows that opioids can produce dependence in weeks, while alcohol and cannabis typically take months to years, meaning the pace varies widely by substance and individual.
This article walks through each stage, explains the brain changes driving them, and maps out what recovery looks like at every point.
The 5 Stages of Addiction
Most clinical frameworks describe addiction as a five-step escalation: first use, regular use or misuse, tolerance, dependence, and addiction.
These stages are not rigid boxes. People can move through them quickly or slowly, and the boundaries often blur. Still, the sequence gives clinicians, families, and people in recovery a shared language for understanding what is happening and why it gets harder to stop over time.
Here is what each stage looks like in practice.
Stage 1: First Use
First use is exactly what it sounds like: the initial exposure to a substance. This might be a prescription painkiller after surgery, a drink at a party, or a vape pen passed around by friends. At this point, most people experience the reward the substance offers without yet developing any pattern of use.
Not everyone who tries a substance moves forward. But certain factors raise the risk of progression, including sensation-seeking personality traits, peer use, early age of exposure, and genetic vulnerability.
Research from the ABCD Study found that modifiable factors like peer substance use and availability were among the strongest predictors of whether adolescents moved from first use to regular use by early adolescence.
Stage 2: Regular Use and Misuse
Regular use means the substance has become a pattern. A person might drink every weekend, vape daily, or use cannabis to manage stress. At this stage, use is often social or coping-driven, and the person may not yet see it as a problem.
Misuse begins when use crosses into territory that carries risk: taking more than prescribed, using in situations where it is dangerous, or relying on a substance to function emotionally.
The brain is starting to build associations between cues, contexts, and the reward the substance provides. Habit circuits are being recruited, and the substance is gaining motivational weight it did not have before.
Stage 3: Tolerance
Tolerance means the body has adapted. The same dose no longer produces the same effect, so a person needs more to feel what they once felt with less. This is a sign that neuroadaptations are underway.
Product design can accelerate this stage dramatically. Nicotine salt pod-mods like JUUL deliver nicotine at concentrations as high as 60 mg/mL, enabling rapid and efficient absorption.
A nationally representative PATH study found that exclusive e-cigarette users among youth developed nicotine dependence signs at a pace similar to combustible cigarette smokers, showing how device engineering can compress what might otherwise take much longer.
Stage 4: Dependence
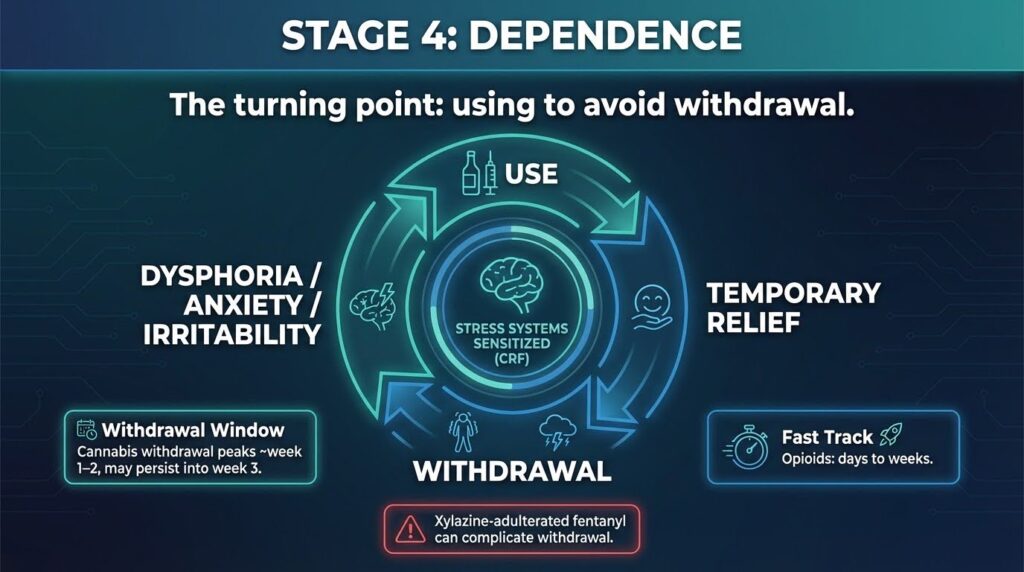
Dependence is the stage where the body and brain have reorganized around the substance. Two things define it: withdrawal symptoms appear when use stops, and the person is now using partly to avoid feeling bad rather than purely to feel good.
This shift from positive to negative reinforcement is a key neurobiological turning point. Stress systems in the brain, including circuits involving corticotropin-releasing factor, become sensitized.
Dysphoria, anxiety, and irritability during abstinence push the person back toward use. For adolescents using cannabis, withdrawal research documents irritability, sleep difficulty, restlessness, and cravings peaking in the first two weeks of abstinence, sometimes persisting into week three.
For opioids, dependence can arrive in days to weeks, especially with potent synthetic opioids. When xylazine adulterates the fentanyl supply, withdrawal becomes more complex and may require specialized management with agents like clonidine, as a 2025 systematic review on xylazine management details.
Stage 5: Addiction
Addiction, or severe substance use disorder (SUD), is defined by compulsive use despite clear harm. The person may want to stop and try repeatedly without success. Relationships, work, health, and safety suffer. The substance has become the organizing principle of daily life.
Under the DSM-5, a SUD diagnosis replaces the older “abuse vs. dependence” split. Clinicians now count symptoms across 11 criteria spanning impaired control, social problems, risky use, and physical dependence. Mild SUD is 2 to 3 symptoms, moderate is 4 to 5, and severe is 6 or more.
This framework, explained clearly by the Addiction Policy Forum, anchors treatment intensity to measurable impairment rather than a single label.
How Many Stages of Addiction Are There?
The five-stage model is the most widely used clinical framework, but it sits alongside two other important systems. The NIDA neurocircuitry model organizes addiction into three stages: binge and intoxication, withdrawal and negative affect, and preoccupation and anticipation.
These map onto the five clinical stages and explain the brain mechanisms driving each transition. The DSM-5 adds a third layer by quantifying severity through symptom counts.
Together, these three frameworks form what researchers call a stage-severity-mechanism map: stages for communication, DSM-5 for diagnosis, and neurocircuitry for targeting treatment.
How Substance Type Shapes the Timeline?
Not all substances follow the same pace. The table below summarizes how progression typically differs across common substances.
| Substance | Key accelerating factors | Typical pace to dependence |
|---|---|---|
| E-cigarettes (nicotine salts) | High nicotine concentration, efficient delivery, flavors | Weeks to months, similar to combustible cigarettes in youth |
| Combustible cigarettes | Rapid pulmonary delivery, social cues | Months, intensifies through adolescence |
| Cannabis (high potency, dabbing) | High THC dose per episode, normalization, concentrates | Months to years, faster with early onset |
| Alcohol | Binge patterns, peer environment, impulsivity | Months to years, highly variable |
| Opioids (illicit fentanyl) | Extreme potency, polysubstance adulteration | Days to weeks for severe dependence |
Adolescents using cannabis concentrates through dabbing show greater persistence and frequency of use over 6 to 12 months compared with peers who do not dab, according to USC research on adolescent cannabis trajectories.
Meanwhile, legalization has not markedly increased adolescent cannabis use overall, but it has lowered perceived risk, which matters because current evidence links early, frequent, high-potency cannabis exposure to adverse outcomes in brain development, mental health, and multiple physical systems.
What the Brain is Doing at Each Stage?
Understanding the neuroscience helps explain why willpower alone is rarely enough to stop progression.
* At the regular use and tolerance stages, the mesolimbic dopamine system is being sensitized. Drug cues gain disproportionate motivational weight, and habit circuits in the dorsal striatum begin to take over from goal-directed decision-making.
* At the dependence stage, opponent processes rise. Stress systems produce dysphoria and anhedonia during abstinence, making negative reinforcement the dominant driver of use.
* At the addiction stage, prefrontal executive control is weakened. Top-down inhibition fails under stress or cue exposure, which is why relapse risk stays high even after long periods of abstinence.
Brain imaging research from the ABCD Study found that resting-state connectivity measured in children aged 9 to 12 predicted which youth would initiate substance use by about age 14, and these brain signatures correlated with neighborhood pollution and socioeconomic disadvantage.
This means structural and environmental factors shape neurological vulnerability long before first use.
What Are the Stages of Change in Addiction Recovery?
Recovery follows its own progression, described by the Transtheoretical Model as five stages of change: precontemplation, contemplation, preparation, action, and maintenance. Relapse is part of the cycle, not a sign of failure.
The SAMHSA definition of recovery is broader than abstinence alone. It includes symptom remission and active pursuit of health, purpose, and community. For substances with high mortality risk, especially opioids, evidence strongly favors medication-supported remission combined with harm reduction and psychosocial care.
Here is what each recovery stage involves and what works at each point.
Precontemplation
The person is not yet considering change. The most effective response is not confrontation but low-threshold engagement: naloxone distribution, nonjudgmental connection, and offering medications without prerequisites.
For opioid use disorder, methadone and buprenorphine reduce all-cause mortality by about half while a person is in treatment, making access at this stage genuinely life-saving.
Contemplation
Ambivalence is the defining feature here. Motivational interviewing works well because it draws out the person’s own reasons for change rather than imposing them. The goal is to tip the decisional balance without creating resistance.
Preparation
The person intends to act soon. Barriers like logistics, fear of withdrawal, and lack of childcare or transportation can stall this stage indefinitely. Same-day starts for buprenorphine or methadone, bridge prescriptions, and emergency department-initiated treatment remove those barriers and move people into action faster.
Action
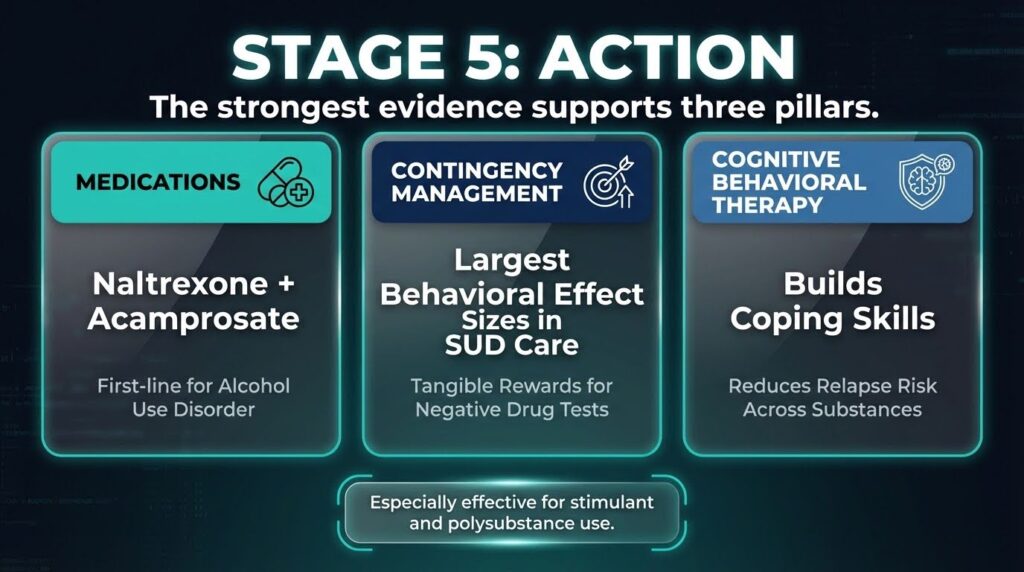
This is the stage of active change. The strongest evidence supports a combination of medications where available, behavioral therapies, and peer support. Contingency management, which provides tangible rewards for objective behaviors like negative drug tests, produces some of the largest behavioral effect sizes in SUD care, especially for stimulant and polysubstance use.
Cognitive behavioral therapy builds coping skills and reduces relapse risk across substances. For alcohol use disorder, naltrexone and acamprosate are first-line medications with meaningful effects on heavy drinking and abstinence rates.
Maintenance
Sustaining recovery over months and years requires more than willpower. Recovery capital, which includes stable housing, employment, supportive relationships, and community connection, becomes the primary protective factor.
A Cochrane review found that Alcoholics Anonymous and 12-step facilitation can increase long-term abstinence rates and reduce healthcare costs compared with other active treatments for alcohol use disorder, making mutual-help a valuable part of a recovery portfolio for many people.
Relapse is Not the End of Recovery
Relapse rates for SUD are comparable to those for diabetes and hypertension. That framing matters because it shifts the response from punishment to adjustment. When symptoms return, the right move is rapid, nonjudgmental re-engagement and a change in the care plan, not discharge.
The NIDA treatment principles are clear on this: addiction is a chronic, relapsing condition, and treatment should be designed for continuity. Same-day medication restarts, flexible levels of care, and peer recovery coaching during transitions all reduce the harm that can follow a lapse, including the elevated overdose risk that comes after a period of reduced tolerance.
Digital tools are also emerging as a way to catch warning signs earlier. Smartphone sensors and ecological momentary assessment can track sleep disruption, mobility changes, and craving patterns in real time, offering a pathway to just-in-time support before a lapse becomes a full relapse.
A 2024 review of digital mental health tools found promising early validity for these approaches across alcohol and mental health populations, though standardization and longer-term validation remain priorities.
Why Early Intervention Changes the Trajectory?
The earlier a person receives support, the less neuroadaptation has occurred and the more modifiable the trajectory remains. Adolescent SBIRT, which stands for Screening, Brief Intervention, and Referral to Treatment, delivered in primary care settings can identify risk before dependence sets in.
A multisite trial protocol comparing standard adolescent SBIRT with a family-based version found that systematic screening catches 25 to 35 percent of youth who would otherwise go unidentified.
Family involvement matters because it addresses the social and environmental factors that accelerate stage transitions: availability of substances, peer norms, and supervision.
Mechanism-targeted modules addressing sensation-seeking and peer influence, combined with digital just-in-time supports, offer the most realistic path to slowing or preventing the shift from regular use to dependence, especially in an era of high-potency products and efficient delivery devices.
The five-stage model remains a useful scaffold. But modern care works best when it pairs that scaffold with DSM-5 severity thresholds, neurobiological insight, and a recovery plan built around the person’s actual stage of change, not a fixed timeline.
If you or someone you care about is anywhere along this continuum, from early misuse to active addiction, professional support can make a real difference. Reach out to The Summit Wellness Group to learn about evidence-based treatment options personalized to where you are right now.
