High-THC cannabis use is linked to a meaningfully greater risk of psychosis and schizophrenia-spectrum illness, and that risk is not the same as it was twenty years ago.
Research now shows that daily use of high-potency cannabis is associated with roughly five times the odds of developing a psychotic disorder compared with never using cannabis at all.
This article walks through what the evidence actually says, why modern cannabis is different from older forms, and what these findings mean for anyone concerned about mental health.
High-THC Cannabis and Schizophrenia Risk: What the Evidence Shows?
The cannabis available today is not the same drug that circulated in prior decades. Average THC concentrations in legal-market flower now commonly exceed 15% to 20%, and concentrates can reach 60% to 90% or higher. Older cannabis typically contained far less THC and often more cannabidiol, or CBD, which may reduce some of THC’s psychosis-promoting effects. That shift in product composition matters enormously when we look at schizophrenia risk.
A large multicenter case-control study across 11 European sites, known as the EU-GEI study, found that daily cannabis users were about three times more likely to have a first episode of psychosis than people who never used cannabis.
Among daily users of high-potency cannabis specifically, that figure rose to roughly five times the odds. The same study estimated that about 20% of new psychosis cases across those 11 sites could be linked to daily cannabis use, and about 12% to high-potency use in particular.
This is not a single outlier finding. It sits within a broader body of evidence that has grown more consistent, not less, as research methods have improved.
How Potency and Frequency Shape Psychosis Risk?
One of the clearest patterns in the research is that psychosis risk is not a simple yes-or-no property of cannabis use. It rises with exposure intensity.
A 2023 systematic review and meta-analysis published in *Psychological Medicine* examined 10 studies covering 7,390 participants and found a significant log-linear dose-response relationship between how often someone uses cannabis and their risk of developing psychosis.
The results broke down like this:
- Yearly use: no significant increase in psychosis risk
- Monthly use: no significant increase in psychosis risk
- Weekly use: 35% greater risk compared with nonuse
- Daily use: 76% greater risk compared with nonuse
The threshold effect here is important. Occasional use does not appear to carry the same measurable risk as frequent use. But once someone crosses into weekly or daily territory, the association becomes statistically clear and clinically meaningful.
Potency adds another layer on top of frequency. A 2009 case-control study from South London found that among cannabis users, 78% of first-episode psychosis cases had used high-potency cannabis, compared with 37% of healthy controls.
That produced an odds ratio of 6.8 for high-potency use among cannabis users, meaning high-potency users were nearly seven times more likely to be in the psychosis group than lower-potency users. Crucially, simply having ever used cannabis was not the main differentiator. Daily use and high-potency use were.
A recent systematic review in the *American Journal of Psychiatry* examined observational and experimental studies on high-potency cannabis and health outcomes.
For psychosis specifically, the review found that findings generally pointed in a detrimental direction, and that the pattern became stronger when analysis was restricted to higher-quality studies. That is the opposite of what you would expect if the association were a methodological artifact.
Why is Modern Cannabis More Concerning Than Older Cannabis?
The comparison between older and modern cannabis is not just about THC percentage in isolation. It involves at least two simultaneous changes.
First, absolute THC content has risen substantially. Products that were once considered strong now sit in the middle of the market. Concentrates represent a category that barely existed in earlier eras of cannabis research.
Second, the ratio of THC to CBD has shifted. Traditional cannabis often contained meaningful amounts of CBD alongside THC. Research cited in a *World Psychiatry* review notes that THC can induce transient psychosis in otherwise healthy people, and that CBD may attenuate those effects. Modern high-potency products often contain very little CBD relative to THC, which plausibly removes a natural buffer against psychotomimetic effects.
This means that when someone uses a high-THC concentrate today, they may be receiving a qualitatively different neurochemical experience than someone who used lower-potency cannabis in the 1990s, not just a larger dose of the same thing.
The EU-GEI symptom study, which analyzed 901 first-episode psychosis patients and 1,235 controls across six countries, found a linear relationship between positive symptom severity and lifetime cannabis exposure. Daily users of high-potency cannabis had the highest positive symptom scores among all exposure groups. This suggests that stronger cannabis affects not only whether psychosis occurs but how severe it is when it does.
Cannabis-Induced Psychosis and the Path to Schizophrenia
Cannabis-induced psychosis, or CIP, is sometimes dismissed as a temporary intoxication effect. The evidence does not support that dismissal. A 2026 systematic review and meta-analysis published in *BMC Psychiatry* examined 13 studies covering 7,515 patients who had been diagnosed with cannabis-induced psychosis. The pooled results showed that about one in five later received a schizophrenia-spectrum diagnosis, while about 5% later received a bipolar disorder diagnosis.
That 20% conversion rate is not a minor footnote. It means that a cannabis-associated psychotic episode is a serious prognostic event, not a benign side effect to wait out.
A large 2026 cohort study of 463,396 adolescents screened in routine pediatric care and followed through age 26 found that past-year cannabis use was associated with a 2.19 times greater risk of psychotic disorder and a 2.0 times greater risk of bipolar disorder.
This was in a setting where average THC concentrations in legal-market flower already exceeded 20%. The cannabis-psychosis signal persists in the current high-potency era, even in very large modern samples.
The progression from cannabis use to psychosis to schizophrenia-spectrum illness is not inevitable, but it follows a recognizable pattern. Early symptoms often include paranoia, unusual perceptual experiences, intensified anxiety, and social withdrawal. These can escalate to hallucinations, delusions, and disorganization. Some people recover fully with abstinence. Others relapse when re-exposed. A meaningful minority transition to chronic psychotic illness.

What Happens After a First Psychotic Episode?
The evidence on relapse is among the most clinically actionable in this entire field. A 10-year prospective cohort study of 220 people presenting to psychiatric services in London found that periods of cannabis use were associated with increased odds of psychosis relapse compared with periods of nonuse.
Continued cannabis use over the full 10 years was associated with a 59.1% higher risk of relapsing psychosis, compared with a 28.5% increased risk among those who stopped using entirely.
The OPTiMiSE study, which followed remitted first-episode schizophrenia-spectrum patients, found that cannabis use increased relapse risk with an adjusted hazard ratio of 3.03. Critically, this association held even among patients who were compliant with their antipsychotic medication, with a hazard ratio of 2.89. Cannabis use also preceded symptomatic worsening and later medication nonadherence, rather than simply accompanying an already-deteriorating course.
This temporal ordering matters. It rebuts the common argument that people only use cannabis because relapse is already starting. The data from the OPTiMiSE study suggest the reverse is often true: cannabis use comes first, and worsening follows.
Who is Most Vulnerable?
Not everyone who uses high-THC cannabis develops psychosis. Risk is concentrated in specific groups, and understanding those groups is essential for honest communication about this topic.
The factors that appear to amplify cannabis-related psychosis risk include:
- Adolescent age at first use, when the brain is still developing
- Daily or near-daily frequency of use
- Use of high-potency THC products, especially concentrates
- Family history of psychotic disorders
- Personal history of psychotic-like experiences
- Genetic variants associated with dopamine function, including AKT1 and COMT
A 2024 case-control study found that cannabis use and schizophrenia genetic predisposition both independently raised psychosis risk, and that the combination of greater genetic liability with high-potency daily cannabis use corresponded to the highest-risk profile overall.
Adolescents deserve particular attention. The developing brain, especially circuits involved in executive control and emotional regulation, remains active into the mid-20s. Early THC exposure may have disproportionate effects compared with adult-onset exposure.
The 2026 adolescent cohort study concluded that its results were consistent with cannabis being a risk factor for psychiatric disorders rather than only resulting from preexisting conditions, a notably strong statement for an observational paper.
What the Research Does and Does Not Say?
It is worth being precise about what this evidence establishes and what it does not.
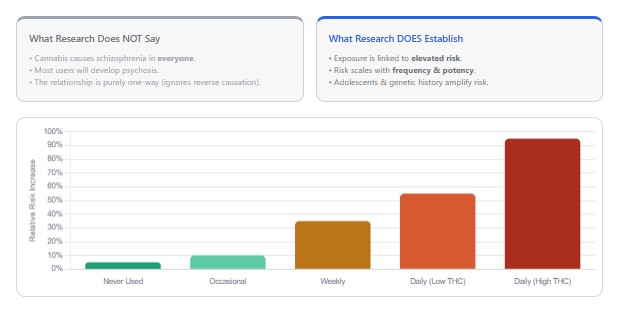
The evidence does not show that cannabis alone causes schizophrenia in everyone who uses it. Most cannabis users do not develop psychosis. The relationship is probabilistic, not deterministic. Reverse causation is real: some people at risk for psychosis may be more likely to use cannabis, partly because of shared genetic liability and partly because of self-medication of distress.
What the evidence does show, with enough consistency to guide clinical practice, is that:
- Cannabis exposure is associated with elevated psychosis risk
- Risk rises with greater frequency and higher THC potency
- The combination of daily use and high-potency cannabis carries the greatest observed risk
- Cannabis-induced psychosis is a serious prognostic event with a meaningful rate of transition to schizophrenia-spectrum illness
- Continued cannabis use after a first psychotic episode worsens outcomes even in medicated patients
- Adolescents and people with family history or genetic vulnerability face amplified risk
The Marconi et al. meta-analysis of 66,816 individuals found that higher levels of cannabis use were associated with increased psychosis risk in a dose-response pattern, and prior meta-analyses had reported roughly a twofold increase in risk of psychotic disorder among cannabis users compared with nonusers.
That signal has not weakened as research has improved. If anything, it has sharpened as studies have moved from crude ever-use comparisons to frequency and potency gradients.
Why Does This Matter Now?
The timing of this evidence matters. Cannabis legalization has expanded access, normalized use, and shifted the market toward higher-potency products. Warning labels in most U.S. states do not yet reflect the psychosis risk from high-potency THC.
A 2024 review of state cannabis warning labels found that only two states required a warning about mental health risks on all products, and only two required a warning about psychosis specifically for high-potency THC products.
Public health messaging has often lagged behind the science. The science now supports a specific and targeted message: modern high-potency cannabis, used frequently, especially by adolescents or people with personal or family vulnerability to psychosis, carries a meaningfully greater risk of psychotic illness than older, lower-potency cannabis did. That is not a speculative claim. It is the most defensible reading of the best available evidence.
If you or someone you care about is using cannabis heavily and experiencing symptoms like paranoia, unusual perceptions, or social withdrawal, those signs deserve serious attention, not reassurance.
Reaching out to a professional who understands co-occurring substance use and psychiatric conditions is a reasonable and important next step. The Summit Wellness Group offers dual diagnosis treatment for adults navigating exactly this kind of overlap between substance use and mental health.
