7-Hydroxymitragynine, commonly called 7-OH, is a potent alkaloid linked to kratom that acts on opioid receptors in the brain.
While it occurs naturally in kratom leaf at trace levels below 0.05%, concentrated commercial 7-OH products sold in gas stations and smoke shops can reach up to 98% purity and pose serious risks including respiratory depression, addiction, and overdose.
This article explains what 7-OH is, how it differs from traditional kratom, and why health officials are issuing urgent warnings about these high-potency products.
What is 7-Hydroxymitragynine?
7-Hydroxymitragynine is an indole alkaloid associated with the Southeast Asian tree *Mitragyna speciosa*, commonly known as kratom. It exists in three clinically distinct forms: as a trace natural component of kratom leaf, as a metabolite formed when the body processes mitragynine (kratom’s primary alkaloid), and increasingly as a concentrated or semi-synthetic commercial product.
The most important distinction is between natural and commercial forms. Traditional kratom leaf contains less than 0.05% 7-OH by dry weight, with some sources reporting levels below 0.02%.
In contrast, commercial 7-OH products may contain dramatically higher concentrations, sometimes approaching near-pure levels. This concentration gap transforms the pharmacology from a mixed botanical profile into something much closer to a direct opioid-like exposure.
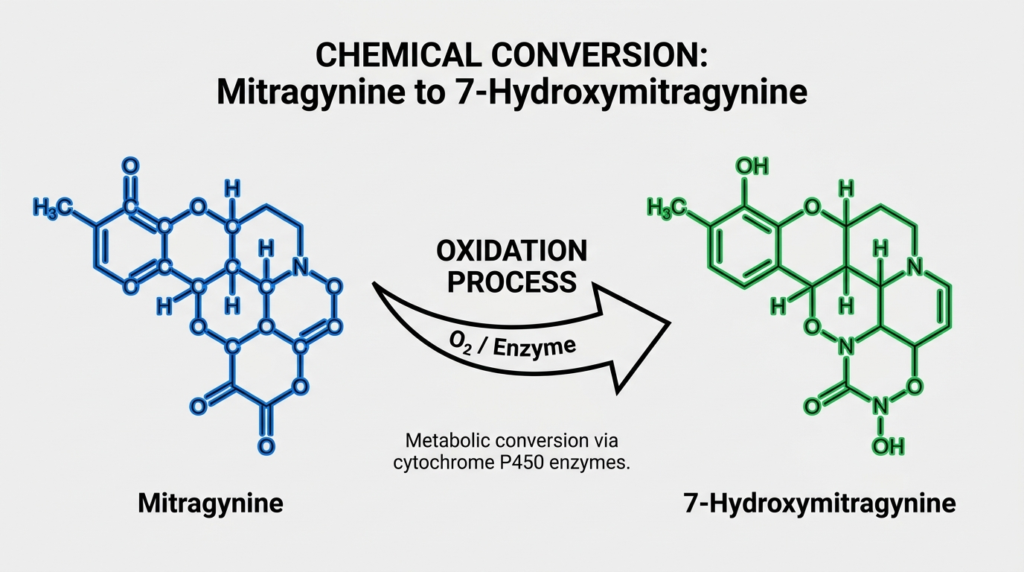
Many commercial 7-OH products are not simply extracted from leaf. Manufacturers often chemically convert mitragynine into 7-hydroxymitragynine through oxidation, then purify it to create tablets, gummies, liquid shots, and powders. This semi-synthetic production route is why regulators increasingly use terms like “chemically manipulated” when describing these products.
How 7-OH Works in the Body?
7-Hydroxymitragynine acts primarily at the μ-opioid receptor (MOR), the same receptor family that mediates effects of morphine and other classical opioids. Research shows that 7-OH has approximately 9-fold higher MOR affinity than mitragynine and behaves as a partial agonist, while mitragynine showed low affinity and antagonist-like behavior in laboratory studies.
This stronger receptor activity explains why 7-OH produces more pronounced opioid-like effects than ordinary kratom use would suggest. The compound is also an active metabolite, meaning that when someone consumes mitragynine, their liver converts some of it into 7-hydroxymitragynine through CYP3A enzyme pathways. This metabolic conversion helps explain why kratom can produce opioid-related effects even though mitragynine itself has relatively weak direct MOR activity.
Some preclinical studies suggest 7-OH may be a G-protein-biased agonist that does not recruit β-arrestin in the same way as classical opioids, potentially offering a different safety profile. However, real-world surveillance data clearly show this theoretical advantage has not prevented serious outcomes including respiratory depression, overdose, and death.
Common Forms of 7-OH Products
Commercial 7-OH products appear in multiple consumer-friendly formats that increase accessibility and may reduce perceived risk:
- Tablets and pills – often labeled with specific milligram amounts
- Rapid-dissolve or chewable tablets – designed for faster onset
- Gummies and edibles – candy-like products with youth appeal
- Liquid shots – concentrated delivery in energy-shot style packaging
- Powders – allowing flexible but imprecise dosing
- Capsules – familiar supplement format
- Drink mixes and beverages – integrated into convenience-store retail
These products are typically sold in gas stations, smoke shops, convenience stores, and online retailers. The form factor matters because rapidly absorbed formats like sublingual tablets and liquid shots may produce quicker, more intense effects that encourage compulsive redosing and increase abuse liability.
What 7-OH is Used For?
Commercial 7-OH products are marketed for pain relief, energy, mood enhancement, anxiety relief, and opioid withdrawal management. Public health agencies note these products are often framed as natural remedies or botanical supplements, which may reduce perceived risk while increasing trial use.
From a pharmacological standpoint, people use 7-OH products to obtain effects associated with μ-opioid receptor activity:
- Analgesia and pain relief
- Euphoria and mood alteration
- Sedation and relaxation
- Relief of opioid withdrawal symptoms
- Sometimes stimulation at lower doses
The deeper reality is that many 7-OH pills and tablets function as legal, easily accessible opioid-like products sold through nonmedical channels.
Because they act on opioid receptors and can cause naloxone-responsive overdose, they should not be understood merely as supplements used for wellness, despite how they are marketed.
Effects and Subjective Experience
The subjective effects of 7-OH vary by dose, route, and formulation, but concentrated products are generally associated with stronger opioid-like effects than whole-leaf kratom. Based on receptor pharmacology, animal studies, and poison center symptom patterns, likely sought effects include:
- Pain relief and bodily comfort
- Warmth and relaxation
- Sedation or drowsiness
- Euphoria in some users
- Relief from anxiety or withdrawal
However, adverse effects are common and can be severe:
- Nausea and vomiting
- Sweating and elevated heart rate
- Agitation and confusion
- Respiratory depression
- Loss of consciousness
- Seizures
The symptom pattern often appears mixed rather than purely sedative, with both autonomic/stimulant-like features and CNS depression. This dual pattern may reflect dose-dependent effects, co-exposures, variable product composition, or individual metabolic differences.
A particularly informative case involved a 23-year-old man using kratom powder who began taking a semi-synthetic 7-OH product at 20 mg three times daily for four days.
During a kratom clinical trial, his subjective kratom effects were blunted, 7-OH was measurable before kratom administration, he developed withdrawal symptoms, and he preferred his stronger 7-OH product over the offered kratom rescue dose. This suggests concentrated 7-OH may quickly create tolerance that makes ordinary kratom feel weak and that users perceive it as more rewarding.
Serious Health Risks
Overdose and Respiratory Depression
Because 7-OH acts on opioid receptors, it can cause respiratory depression and overdose. Public health agencies explicitly recommend naloxone in suspected overdose, though they warn that reversal may be incomplete when other substances are involved.
The Kansas health department states that combining 7-OH with alcohol or other sedatives can cause severe respiratory depression and death.
Dependence and Withdrawal
Traditional kratom itself can cause dependence and withdrawal, but newer literature indicates that concentrated 7-OH products likely pose greater dependence liability than traditional leaf products.
Several mechanisms explain harder withdrawal from concentrated 7-OH: stronger MOR stimulation, repeated high-dose exposure, shorter duration requiring frequent redosing, greater receptor adaptation, and less buffering from the mixed alkaloid profile seen in leaf kratom.
Reported withdrawal symptoms include:
- Restlessness and body aches
- Fatigue and irritability
- Cold sweats and insomnia
- Anxiety and gastrointestinal distress
- Muscle pain and cravings
A 2026 case report addressing acute withdrawal from high-dose chronic 7-OH use concludes that concentrated 7-OH products differ from kratom leaf and can produce dependence and withdrawal requiring careful clinical management, including properly timed buprenorphine initiation.
Seizures and Neurologic Effects
Several sources list seizures among reported harms, along with confusion, sleepiness, and loss of consciousness. America’s Poison Centers includes seizures among reported symptoms in 2025 exposures to 7-OH.
Poison Center Data Shows Sharp Increase
The most important national statistic comes from the CDC’s 2026 Morbidity and Mortality Weekly Report: kratom-related poison center exposure reports increased from 258 in 2015 to 3,434 in 2025, approximately a 1,200% increase. The CDC specifically notes that the sharp 2025 increase coincided with the emergence of high-potency semisynthetic formulations, including 7-OH.
America’s Poison Centers reported 165 exposures to 7-OH in 2025. Among cases involving 7-OH alone, 35% had serious health problems and 67% were treated at a healthcare facility. Texas reported 192 exposures involving kratom or 7-OH products, with 19 exposures to concentrated 7-OH products and 11 of those requiring treatment at a healthcare facility.
These numbers are strong sentinel indicators that concentrated 7-OH products are generating clinically meaningful harm. Local fatalities have also been reported, with Santa Barbara County warning that two deaths in 2025 involved kratom as a contributing factor, and Los Angeles County tying additional fatal overdoses to synthetic kratom products.
Legal and Regulatory Status
As of May 2026, kratom, mitragynine, and 7-OH were not scheduled under the federal Controlled Substances Act. However, the federal status quo was under active challenge. On July 29, 2025, the FDA and HHS announced they had recommended the DEA place certain high-concentration or semi-synthetic 7-OH products into Schedule I.
Multiple sources describe the recommendation as specifically targeting concentrated or synthetic 7-OH products rather than natural leaf kratom.
The DEA had not issued a final scheduling rule as of May 2026, and a formal rulemaking process with public comment would be expected before any federal scheduling becomes final. Even without scheduling, the FDA had taken enforcement actions, issuing warning letters to companies illegally marketing concentrated 7-OH products and stating that 7-OH is not lawful in dietary supplements or conventional foods.
State laws vary significantly. Six states have broad kratom or alkaloid bans: Alabama, Arkansas, Indiana, Louisiana, Vermont, and Wisconsin. Several states including Arizona, Colorado, Oklahoma, Texas, and Utah reportedly cap 7-OH at 2% of alkaloid content.
California state and county public health materials state kratom and 7-OH products are illegal to sell or manufacture for human consumption in California, despite continued retail availability in some locations.
By spring 2026, members of Congress were calling for emergency scheduling, and a bill—H.R. 8000, the END 7-OH Act—had been introduced to schedule synthetic 7-hydroxymitragynine as Schedule I.
Why These Products Are Especially Dangerous?
Several factors make concentrated 7-OH products particularly risky in real-world use:
Mislabeling and consumer misunderstanding: Many products are marketed as kratom, natural products, or wellness aids even when they are concentrated or semi-synthetic, creating an informational hazard.
Unregulated potency: Because 7-OH is unregulated, potency and quality can vary widely. Consumers may not know what dose they are taking or whether the label is accurate.
Retail normalization: Products sold in gas stations, smoke shops, and convenience stores reduce the psychological barrier to purchase and may make a potent opioid-like product seem routine.
Consumer-friendly formats: Gummies, shots, and candy-like packaging increase the chance of broad exposure, including accidental exposure by children and teens.
Fast-onset formats: Rapidly absorbed forms such as sublingual and chewable tablets may produce intense, short-lived euphoria and promote frequent redosing.
How 7-OH Differs From Traditional Kratom?
One of the clearest themes across public health evidence is that concentrated 7-OH products are not the same as traditional kratom products, even though they are often sold under kratom branding.
The Kansas Department of Health and Environment explicitly states that 7-OH is sometimes sold as if it were the same as kratom, but it is not.
Key Differences
| Feature | Traditional Kratom Leaf | Concentrated 7-OH Products |
|---|---|---|
| Composition | 40–50+ alkaloids in botanical matrix | Single alkaloid isolated or enriched |
| Natural 7-OH level | Trace amounts, often <0.05% | Can reach up to 98% purity |
| Main active compound | Mitragynine (~1–2% of leaf) | 7-Hydroxymitragynine |
| Production method | Leaf-based powder, tea, capsules | Often semi-synthetic conversion |
| Typical forms | Powder, tea, capsules | Tablets, gummies, shots, rapid-dissolve tabs |
| Effect profile | Mixed stimulant/sedative botanical effects | Stronger direct opioid-like effects |
| Dependence risk | Possible with regular use | More rapid and clinically concerning |
| Regulatory focus | Mixed and debated | Increasingly targeted specifically |
This distinction matters for concentration, composition, production method, effects, and policy relevance. Treating all kratom-related products the same obscures the real risk gradient inside the market and weakens targeted harm prevention.

Overdose Response and Naloxone
One of the most clinically important findings is that naloxone can reverse opioid overdose from 7-OH. The Kansas health department states that opioid overdose, including from 7-OH, can be reversed with naloxone. Texas advises clinicians to administer naloxone for reversal of respiratory depression.
However, naloxone may not fully reverse effects if 7-OH was mixed with alcohol or other drugs. This reflects the broader concern that multiple-substance exposures are often more severe. The CDC found that 79% of reported kratom-associated deaths involved multiple substances.
Public health guidance generally recommends calling 911 immediately, administering naloxone if available, keeping the person breathing and on their side if unresponsive, staying until help arrives, and contacting poison control if adverse effects occur.
Interactions and Co-Use Risks
The CDC notes that kratom use with alcohol, opioids, benzodiazepines, stimulants, and antidepressants may increase risk through additive central nervous system effects and pharmacokinetic interactions. This is especially concerning for concentrated 7-OH because of its stronger opioid-like receptor activity.
Kansas health officials specifically warn that combining 7-OH with alcohol or other sedatives can cause severe respiratory depression and death. The CDC also highlights links between kratom exposure reports, psychiatric comorbidity, and suicide attempts in multiple-substance reports, suggesting that screening for 7-OH use should include mental health risk assessment.
Evidence-Based Conclusion
Based on the strongest and newest evidence, concentrated 7-OH is best understood as a de facto opioid-like consumer product that has been inaccurately sheltered under the broader cultural label of kratom. This conclusion is most consistent with receptor pharmacology, metabolic data, animal behavioral effects, poison center severity data, state toxicology alerts, and human case reports of dependence and withdrawal.
Three things should change in how people discuss it:
1. Consumers should stop thinking 7-OH and kratom are interchangeable. They are not equivalent exposures.
2. Clinicians should screen for product type, not just ask “Do you use kratom?” A patient taking leaf powder is pharmacologically different from a patient taking 20 mg 7-OH tablets several times a day.
3. Researchers and policymakers should separate botanical kratom from concentrated 7-OH in surveillance and regulation. Failure to do so undermines both harm reduction and accurate risk assessment.
The biased-agonism literature does not justify reassuring messaging about concentrated 7-OH. Real-world data already show enough serious intoxication, dependence, and withdrawal to treat it as a substantial public health concern.
Why Does This Matter?
The emergence of 7-OH products marks a significant turning point in the U.S. kratom-related marketplace. What began as a plant-associated alkaloid present only in trace amounts in natural leaf has become the basis for a rapidly expanding class of concentrated, often semi-synthetic consumer products sold in highly accessible retail formats.
The strongest evidence does not support treating these products as routine herbal supplements. Instead, it supports understanding them as potent opioid-like products used for pain relief, mood alteration, euphoria, sedation, and self-treatment of withdrawal, while carrying substantial risks of addiction, respiratory depression, overdose, and death.
National poison center data, state warnings, and federal regulatory actions all point in the same direction: the risk profile of concentrated 7-OH is materially different from that of traditional whole-leaf kratom, and public health strategy should reflect that distinction.
If you or someone you care about is struggling with substance use involving kratom, 7-OH, or other opioid-like products, our professional support can make a meaningful difference. Consider reaching out to explore The Summit Wellness Group’s evidence-based treatment options that address both the physical and emotional aspects of recovery.
