Substance Interactions: Risks, Effects & Safety Guides
Mixing drugs, alcohol, and marijuana at the same time creates risks that go well beyond what either substance causes on its own. A recent review found that alcohol and cannabis together produce additive impairment in driving skills, cognition, and subjective intoxication, meaning the combined effect is measurably worse than either alone. This guide walks through what the research actually shows, who faces the greatest danger, and what you can do to stay safer.
The evidence consistently shows that combining substances creates a different and more dangerous risk profile than using either one alone. Driving impairment increases, judgment becomes less reliable, and long-term risks may rise. The key takeaway is simple: mixing substances is not neutral—it multiplies risk.
Our dual diagnosis programs offer support to those dealing with substance use, mixing substances, and co-occurring mental health conditions. Our drug rehab centers in Atlanta and Roswell offer individualized partial hospitalization programs, IOP, and outpatient levels of care. We also offer medical detox, inpatient rehab,and sober living through our network of partner facilities.
Not sure which program is right for you? Call us today at 770-299-1677 or read our guide to finding the best rehab in Georgia.
In this article
Resources
- Signs of Drug Abuse
- Rising Mental Health and Substance Abuse Issues Linked to Loneliness
- National Uptick in Human Trafficking: A Growing Crisis in America and Worldwide
- Guide to Recovery in Georgia
- “Unlocked: A Jail Experiment:” Comprehensive Guide to Successful Reintegration
- BIPOC Support
- Drug Overdoses
- Suicide Prevention Resources
- Substance Interactions
- What Does Being High on Drugs Feel Like?
- Tips For Drug Withdrawal
- Search
Drug, Marijuana, and Alcohol Interactions: Why Combined Use Matters
Most people think about alcohol and marijuana as two separate choices. The science says otherwise. When both substances are active in your body at the same time, they interact at a pharmacological level, not just a behavioral one.
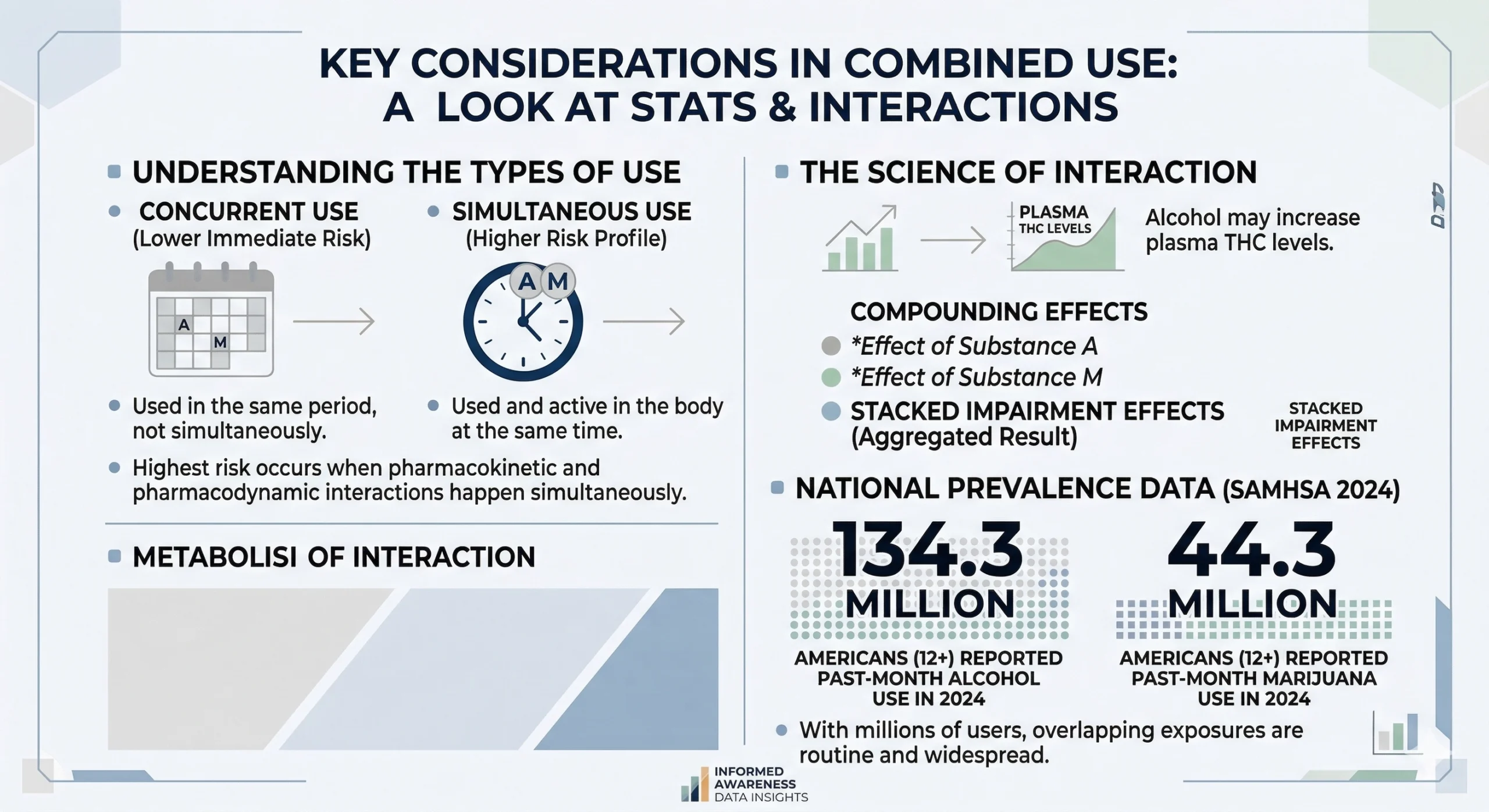
There are two main ways this happens. First, one substance can change how the other is absorbed or metabolized. Research has shown that alcohol can increase plasma THC levels after cannabis use, which means you may end up with more THC in your bloodstream than you expected. Second, both substances affect overlapping systems in the brain, so their sedating, impairing, and judgment-reducing effects stack on top of each other.
The distinction between concurrent use and simultaneous use matters here. Concurrent use means you use both substances in the same general period, say the same week, but not at the same time. Simultaneous use means both are active together. Simultaneous use carries a distinctly higher risk profile because that is when pharmacokinetic and pharmacodynamic interactions actually occur.
According to SAMHSA’s 2024 national data, about 134.3 million Americans aged 12 or older reported past-month alcohol use and 44.3 million reported past-month marijuana use in 2024. With numbers that large, overlapping exposures are not rare. They are routine.
Mixing Alcohol and Drugs
The clearest and most consistent finding across the research is this: combining alcohol and cannabis worsens impairment more than either substance alone, especially for driving and cognitive performance.
A narrative review by Arkell and colleagues concluded that alcohol and cannabis have additive effects on driving skills, cognition, and subjective intoxication. That is not a tentative finding. It is the summary judgment of a review that weighed controlled laboratory studies, simulator research, and subjective effect data together.
At the same time, a 2024 narrative review on subjective effects found that people’s felt experience during simultaneous use is inconsistent across studies. Some people report feeling more impaired, more sedated, or more cognitively slowed. Others describe a “balancing” effect or even increased focus. A qualitative study of college students identified nine broad themes in how simultaneous use felt compared to alcohol alone, and the most frequently reported theme was increased impairment, including greater cognitive, physical, and behavioral dysfunction.
This inconsistency in felt experience is not reassuring. It is actually part of the problem. If you cannot reliably tell how impaired you are, you cannot make safe decisions about driving, operating equipment, or taking more substances.
Tramadol and Alcohol: Using tramadol with alcohol can increase the risk of respiratory depression, sedation, and overdose.
Oxycodone and Alcohol: Combining oxycodone and alcohol significantly raises the risk of slowed breathing and life-threatening complications.
GHB and Alcohol: Mixing GHB with alcohol can cause severe central nervous system depression, leading to unconsciousness or overdose.
Cocaine and Alcohol: Mixing cocaine and alcohol creates cocaethylene, which severely increases the risk of heart failure and sudden death.
Lamictal and Alcohol: Combining Lamictal and alcohol can worsen dizziness and significantly impair coordination or judgment.
Methadone and Alcohol: Mixing methadone with alcohol can cause dangerous respiratory depression, profound sedation, and a high risk of fatal overdose.
What Simultaneous Use Commonly Changes
- Driving-related performance worsens beyond what alcohol or cannabis causes alone
- Reaction time slows and lane control degrades
- Divided attention, the ability to track multiple things at once, suffers more than with single-substance use
- Subjective intoxication increases for many users, though not all
- Risk perception becomes less accurate, meaning people may feel capable when they are not
- Duration of functional impairment may extend, especially with oral cannabis products
Route of administration matters here too. Edibles have a delayed onset, which means someone who drinks alcohol and then eats a cannabis edible may not feel the full combined effect for an hour or more. By then, they may have already made unsafe decisions, including getting behind the wheel.
Mixing Alcohol and Marijuana
Driving is where the evidence is strongest and the stakes are highest. Multiple controlled studies and systematic reviews converge on the same conclusion: cannabis impairs driving, alcohol impairs driving, and combining them is worse than either alone.
A systematic review and meta-analysis of acute THC-induced impairment found that THC meaningfully degrades driving and cognitive skills related to driving. Controlled studies by Hartman and colleagues on lateral vehicle control showed that cannabis and alcohol together produced greater impairment in lane-keeping than either substance alone. Research on divided attention tasks during driving found similar results, with combined exposure degrading performance more than single-substance use.
One of the most important and underappreciated findings in this area is the mismatch between felt safety and actual performance. Studies show that cannabis users’ perception of their own driving safety often does not match their measured impairment. When alcohol is added, that gap can widen further because alcohol reduces inhibition and self-monitoring at the same time that THC degrades motor control and attention.
The Lower-Risk Cannabis Use Guidelines explicitly identify drivers as a subgroup requiring particular caution. The National Academies of Sciences, Engineering, and Medicine similarly recommend public campaigns warning that cannabis use in combination with alcohol or prescription drugs carries elevated risk.
The practical rule is not complicated: do not drive after using cannabis, do not drive after drinking, and especially do not drive after using both, even if each amount seems small.
Weed and Alcohol: Combining these substances can worsen reaction time, coordination, and judgment. Many users feel more intoxicated, but some underestimate their impairment, which increases risk.
CBD and Alcohol: CBD is often perceived as low-risk, but combining it with alcohol may still increase sedation and impair coordination.
Alcohol and Medication Interactions
Alcohol interacts with many medications in ways that increase sedation, impair coordination, or change how drugs are processed in the body. These effects vary by drug type, but most involve either amplified side effects or reduced safety.
Adderall and Alcohol: Mixing Adderall and alcohol can mask intoxication, leading people to drink more than intended. This increases the risk of heart strain, poor judgment, and overdose.
Ambien and Alcohol: Taking Ambien with alcohol can significantly increase drowsiness and impair coordination, raising the risk of accidents and memory loss.
Benadryl and Alcohol: Mixing Benadryl and alcohol can intensify sedation and slow reaction time, making everyday activities like driving dangerous.
Zoloft and Alcohol: Combining Zoloft and alcohol may worsen side effects like dizziness and mood instability, while reducing the effectiveness of treatment.
Lexapro and Alcohol: Lexapro and alcohol together can increase sedation and impair judgment, especially during the early stages of treatment.
Prozac and Alcohol: Mixing Prozac and alcohol may affect mood regulation and increase the risk of emotional instability or impulsive behavior.
Marijuana and Medication Interactions
Cannabis can interact with medications by affecting brain function and altering how drugs are metabolized. These interactions may increase side effects or change how effective a medication is.
Zoloft and Marijuana: Using marijuana with Zoloft may increase side effects like dizziness or anxiety while affecting how the medication works.
Prozac and Marijuana: Combining Prozac and marijuana can influence mood and cognition, sometimes leading to unpredictable psychological effects.
Adderall and Marijuana: Mixing Adderall and marijuana can create opposing effects that strain focus, mood, and cardiovascular function.
Vyvanse and Marijuana: Using Vyvanse with marijuana may alter attention and increase anxiety or heart rate in some individuals.
Xanax and Marijuana: Combining Xanax and marijuana can increase sedation and impair coordination, raising the risk of accidents.
Ambien and Marijuana: Using Ambien with marijuana may intensify drowsiness and disrupt normal sleep patterns.
Prednisone and Marijuana: Mixing prednisone and marijuana may affect immune response and mood, though effects can vary widely.
Lamictal and Marijuana: Combining Lamictal and marijuana may influence mood stability and neurological effects.
Mental Health and Young Adult Risks
Young adults are the group most likely to use alcohol and cannabis simultaneously, and they also face some of the most significant downstream consequences.
A longitudinal study by Thompson and colleagues followed young adults over time and found that higher frequency of simultaneous alcohol and cannabis use was associated two years later with heavier substance use, more substance-related harms, symptoms of psychosis, and externalizing problems. Concurrent but non-simultaneous use was also linked to conduct symptoms and alcohol use disorders compared to alcohol-only use. This is one of the most important findings in the entire evidence base because it shows that simultaneous use is not just an acute impairment issue. It may mark or contribute to escalating risk over time.
Research on co-occurring disorders in mental health treatment settings shows that alcohol use disorder and cannabis use disorder frequently appear alongside anxiety, depression, trauma-related conditions, and psychotic disorders. People with mental health conditions have higher rates of both disorders than the general population, and substance use can worsen symptom burden and complicate treatment.
Bipolar and Marijuana: Using marijuana with bipolar disorder may increase mood instability and worsen episodes of depression or mania.
ADHD and Marijuana: Cannabis use in individuals with ADHD may affect attention, motivation, and long-term symptom management.
Adolescents face additional vulnerability. Reviews of cannabis use in adolescents emphasize that early and frequent use, especially of high-potency products, can affect brain development and increase mental health risk. Layering alcohol co-use on top of that vulnerability strengthens the case for early, targeted prevention.
Mixing Substances Risks: Medications and Other Drugs
The interaction problem does not stop at alcohol and cannabis. Many people also take prescription or over-the-counter medications, and both alcohol and cannabis can interact with those drugs in ways that increase risk. This is especially true with:
- Opioids
- Benzodiazepines
- Sleep medications
These combinations can affect breathing, reaction time, and decision-making in dangerous ways.
The most immediate concern is additive central nervous system depression. Combining cannabis or alcohol with benzodiazepines, opioid pain medicines, sedating antihistamines, or sleep aids can increase drowsiness, slow reaction time, impair coordination, and in serious cases affect breathing. This is not a theoretical risk. It follows directly from the pharmacology of CNS depressants.
Cannabis may also affect the metabolism of certain medications through CYP enzyme pathways, potentially raising or lowering drug concentrations in ways that change their effects or side effects. A 2025 anesthesia safety review from the Anesthesia Patient Safety Foundation recommends that clinicians document cannabis and alcohol use as part of standard preoperative assessment, alongside opioids and sedatives, because of concerns about higher anesthetic requirements, airway reactivity, hemodynamic instability, and possible drug interactions.
The real-world scenario that carries the most risk is not two substances but three or more: alcohol, THC-rich cannabis, and a prescribed or OTC psychoactive drug. That combination can impair reaction time, coordination, blood pressure stability, and decision-making far beyond what any single substance would suggest.
Who Faces the Greatest Risk
Not everyone faces the same level of danger from mixing substances. Several groups deserve particular attention.
Young adults and adolescents face the highest prevalence of simultaneous use and the greatest developmental vulnerability. One survey found that simultaneous use was nearly as common as alcohol-only use in a young adult sample, with about 41 percent using both simultaneously compared to 42 percent using alcohol alone.
Drivers face the clearest and most immediate safety risk. The evidence here is strong enough to support a firm behavioral rule, not just a general caution.
Older adults are increasingly relevant as cannabis use expands across age groups. They tend to take more medications, metabolize substances more slowly, and have less physiologic reserve, all of which increase interaction risk.
People with mental health conditions face compounded risk because substance use can worsen psychiatric symptoms, complicate medication management, and create a self-reinforcing cycle of use and distress.
Surgical patients may not think of cannabis as medically relevant, but the perioperative evidence says otherwise. Acute cannabis intoxication and regular use both carry anesthetic implications that clinicians need to know about before procedures.
Screening, Prevention, and What to Do
One of the clearest gaps identified in the research is that most screening tools and clinical histories ask about alcohol and cannabis separately. They do not ask whether both are used on the same occasion. That gap matters because simultaneous use carries distinct risks that concurrent-but-separate use does not.
Researchers have explicitly called for surveillance and screening tools to ask specifically about simultaneous use so that clinicians and public health systems can identify people at higher risk. The same logic applies to medication reviews: asking about cannabis without asking about alcohol, timing, and other sedating drugs misses the real exposure pattern.
Public health guidance has moved toward harm reduction rather than abstinence-only messaging. The Lower-Risk Cannabis Use Guidelines recommend delaying initiation until after adolescence, avoiding high-potency THC products, reducing frequency and intensity, and exercising particular caution among drivers, pregnant individuals, older adults, and those with comorbidities. The National Academies recommend explicit public campaigns that name combined use with alcohol or prescription drugs as a specific risk, not just a footnote.
If you use cannabis and alcohol together and notice that your use is escalating, affecting your mood, causing vomiting episodes, or impairing your relationships or work, those are signals worth taking seriously. Early assessment and brief intervention in primary care settings have good evidence behind them. Waiting until problems are severe is not necessary and not safer.
Why This Is Not Just a Lifestyle Question
It can be tempting to frame simultaneous alcohol and cannabis use as a personal choice with manageable consequences. The research does not support that framing.
The evidence shows that combining these substances creates a distinct safety profile, not just a stronger version of either one. Driving impairment is amplified. Self-assessment becomes less reliable. Longitudinal risk for heavier use and mental health problems increases. Medication interactions add further complexity. And the newer cannabis environment, with higher-potency products, edibles, and broader legal access, means that older assumptions about cannabis being mild or self-limiting no longer hold.
The National Academies’ policy report frames this clearly: public health campaigns should warn specifically about cannabis use in combination with alcohol and other drugs, and they should target vulnerable populations directly. That is not alarmism. It is the appropriate response to a body of evidence that consistently points in the same direction.
The most honest summary of what the science shows is this: mixing alcohol and marijuana is not a neutral pairing. It is a risk multiplier, and it should be treated as one.
Getting Help
If you or someone you care about is struggling with alcohol, marijuana, or combined substance use, speaking with a treatment professional is a practical and important step. The Summit Wellness Group offers dual diagnosis treatment that addresses both substance use and co-occurring mental health conditions, with individualized care available across multiple levels of support.
We’re Here To Help
Get help now
We’d love the opportunity to help you during this overwhelming and difficult process. The Summit Wellness Group is located in Georgia and all of your calls will be directed to one of our local staff members. Our sincere passion is helping people recover so that they can live full, meaningful and healthy lives.
Call us 24/7 at 770-299-1677. If we aren’t the right fit for you then we’ll utilize our expertise and connections within the treatment industry to assist you in finding the best provider for your specific needs. Alternatively you can fill out our contact form and a member of our staff will contact you shortly.
